Biopsy & Diagnosis - The First Cut
- Goal: Confirm malignancy, grade, type; guide treatment.
- Key Principles:
- Plan incision for future surgery; resect biopsy tract.
- Adequate, representative tissue.
- Avoid tumor spillage/seeding.
- Proper handling (e.g., 10% formalin).
- Types & Utility:
- FNAC: Cytology; screening (e.g., thyroid, LN).
- Core Needle (Tru-Cut): Histology; preferred for solid tumors (breast, sarcoma).
- Incisional: Wedge from large tumor; diagnostic.
- Excisional: Complete removal of small lesion; diagnostic & therapeutic (e.g., skin melanoma <2cm, small LN).
- Frozen Section: Intraoperative; rapid diagnosis, margin assessment. Accuracy ~95-98%.
⭐ Tru-Cut biopsy is the gold standard for pre-operative diagnosis of most solid tumors, providing tissue architecture.
Staging & Imaging - Mapping the Enemy
- Purpose: Defines disease extent (local, regional, distant); guides therapy; predicts prognosis.
- TNM System (AJCC/UICC):
- T: Primary Tumor (size, local extent/invasion)
- N: Regional Lymph Nodes (involvement, number, site)
- M: Distant Metastasis (presence/absence)
- Staging Types:
- Clinical (cTNM): Pre-treatment (exam, imaging, biopsy).
- Pathological (pTNM): Post-surgery; most accurate.
- ypTNM: Post-neoadjuvant therapy.
- Key Imaging Modalities:
- CT: Workhorse for chest, abdomen, pelvis; contrast essential.
- MRI: Superior for soft tissue (e.g., rectal, brain, liver); DWI.
- PET-CT (FDG): Metabolic activity; detects occult mets, assesses treatment response.

- USG/EUS: Initial assessment, guided biopsies (e.g., thyroid, pancreas); GI staging.
- SLNB (Sentinel Lymph Node Biopsy): Nodal staging (e.g., breast, melanoma), avoids extensive dissection if negative.
⭐ Pathological staging (pTNM), derived from surgically resected tissue, remains the strongest prognostic factor for most solid malignancies after curative intent surgery.
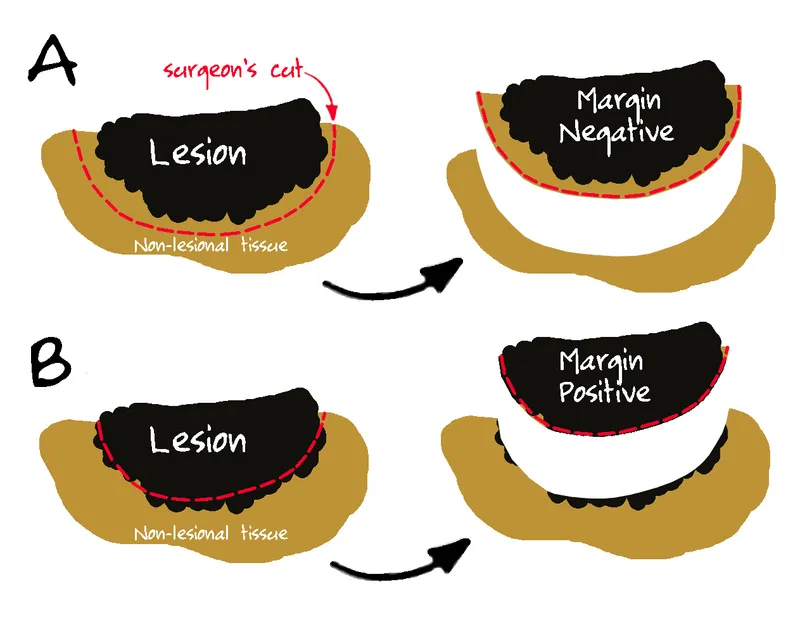
Resection & Margins - Clearance Ops
- Goal: Achieve R0 resection (microscopically clear margins) for cure.
- Margin Types:
- R0: No tumor at margin.
- R1: Microscopic tumor at margin.
- R2: Macroscopic residual tumor.
- Clear Margin: No tumor cells at inked edge. Width varies:
- Sarcoma: 1-2 cm.
- Basal Cell Carcinoma (BCC): 3-5 mm.
- Melanoma: Varies by Breslow depth (e.g., 1 cm for ≤1mm depth).
- "En bloc" Resection: Tumor + surrounding tissue removed as one unit.
- Intraoperative Assessment: Frozen section guides further excision if margins positive/close.
- Palliative Resection: Symptom relief, may be R1/R2.
- Debulking: Reduces tumor burden, not curative.
⭐ R0 resection is the single most important prognostic factor for survival in most solid tumors.
Multimodal Treatment - Combined Arms
- Integrates surgery with chemotherapy (CT), radiotherapy (RT), targeted therapy, immunotherapy.
- Aims: ↑ cure rates, organ preservation, better Quality of Life (QoL).
- Key Approaches:
- Neoadjuvant: Therapy before surgery (downstages tumor, assesses treatment response).
- Adjuvant: Therapy after surgery (targets micrometastases, ↓ recurrence risk).
- Concurrent: Therapies given together or in close sequence (e.g., chemoradiation).
- Palliative: Surgery/therapy for symptom relief (pain, obstruction), not curative; improves QoL.
- Prophylactic: Risk-reducing surgery in high-risk individuals (e.g., BRCA+ mastectomy).
⭐ Neoadjuvant therapy can convert unresectable tumors to resectable, improving surgical outcomes and prognosis.
High‑Yield Points - ⚡ Biggest Takeaways
- R0 resection (microscopically negative margins) is paramount for curative intent in solid tumors.
- Sentinel Lymph Node Biopsy (SLNB) is standard for staging in melanoma and breast cancer, guiding further treatment.
- Multimodal therapy (surgery, chemotherapy, radiotherapy) is often required for locally advanced or aggressive cancers.
- Accurate tumor staging (TNM) and histological grade are critical for prognosis and treatment planning.
- Achieving adequate negative surgical margins is a primary goal; specific widths vary by tumor type and biology.
- Palliative surgery focuses on symptom relief (e.g., obstruction, pain) and improving quality of life, not cure.
- Neoadjuvant therapy aims to downstage tumors, improving resectability and organ preservation chances before surgery.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more