Core Concepts & Aims - Setting the Stage
- Neoadjuvant Therapy (NAT): Systemic or local therapy administered before definitive surgery.
- Aims: Downstage tumor, improve resectability, assess biological response, early micrometastasis control.
- Adjuvant Therapy (AT): Systemic or local therapy administered after definitive surgery.
- Aims: Eradicate residual micrometastases, reduce recurrence risk, improve overall survival.
- Perioperative Therapy: Treatment strategy involving therapy both before and after surgery, aiming for comprehensive tumor control.
⭐ Neoadjuvant therapy provides a unique opportunity for in-vivo assessment of tumor sensitivity to specific treatments, guiding further management strategies.
Neoadjuvant Approach - Shrink Smart
Administered before definitive surgery.
- Goal: Shrink tumor (downstage), ↑ resectability, early micrometastasis control.
- Key Indications:
- Locally advanced tumors (e.g., breast, rectal, esophageal, H&N, sarcoma).
- Borderline resectable cases.
- Organ preservation (e.g., breast, larynx, rectal sphincter).
- Advantages:
- Assesses in vivo chemo/radio-sensitivity.
- ↑ R0 resection rates.
- Enables less radical surgery.
- Disadvantages:
- Surgery delay.
- Treatment toxicity.
- Rare risk of progression.
- Modalities: Chemo (NACT), Radio (NART), CRT, Hormonal, Targeted, Immuno.
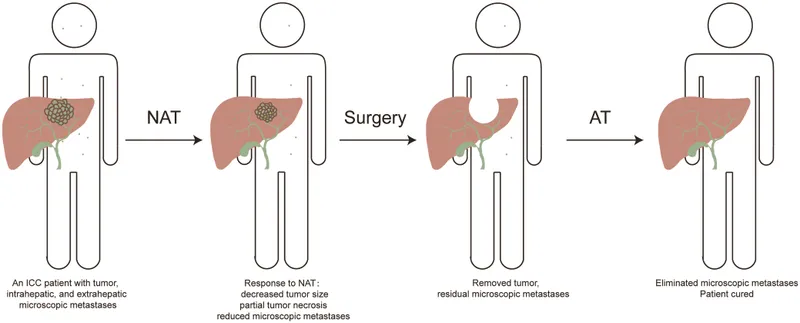
⭐ Pathological Complete Response (pCR) post-neoadjuvant therapy is a strong prognostic indicator in many cancers like breast and rectal.
Adjuvant Approach - Safety Net Strategy
- Therapy after surgery; targets micrometastases to ↓ recurrence & ↑ survival.
- Key Rationale: "Safety net" post-primary tumor removal.
- Indications:
- High-risk pathology: positive margins, nodal spread (e.g., pN+), high grade.
- Certain cancers (e.g., breast, colorectal, lung).
- Modalities: Chemotherapy (CTX), Radiotherapy (XRT), Hormonal, Targeted, Immunotherapy.
- Pros: Addresses occult disease; pathology-informed.
- Cons: Overtreatment risk; toxicity; potential delay.

⭐ Adjuvant therapy in Stage III colon cancer or HER2+ breast cancer is a standard of care, significantly boosting cure rates post-surgery.
Comparative Analysis - Tale of Two Timings
| Feature | Neoadjuvant Therapy | Adjuvant Therapy |
|---|---|---|
| Timing | Before primary local therapy | After primary local therapy |
| Primary Goal | Shrink primary tumor, improve resectability, assess chemo-sensitivity | Eradicate residual micrometastases, reduce recurrence risk |
| Tumor Status | Locally advanced, borderline resectable, or initially unresectable | Completely resected tumor, but high risk of systemic recurrence |
| Response Assess | Clinical/pathological response pre-op | DFS, OS, surveillance |
| Surgery Impact | May allow less extensive surgery, organ preservation | No impact on completed primary surgery |
Tumour-Specific Protocols - Real-World Tactics
- Breast Cancer:
- Neoadjuvant: For downstaging (e.g., LABC), HER2+ (TCHP), TNBC (AC-T ± Pembrolizumab).
- Adjuvant: Based on receptor status & risk (e.g., Endocrine Tx, Trastuzumab, Chemo).
- Colorectal Cancer (CRC):
- Rectal (locally advanced): Neoadjuvant Chemoradiotherapy (CRT) (e.g., Capecitabine/5-FU + RT) is standard.
- Colon (Stage III, high-risk Stage II): Adjuvant FOLFOX or CAPOX.
- Esophageal/Gastric Cancer:
- Adenocarcinoma (Gastric/Esophageal): Perioperative FLOT (5-FU, Leucovorin, Oxaliplatin, Docetaxel).
- Esophageal SCC: Neoadjuvant CRT (CROSS protocol: Carboplatin/Paclitaxel + RT) or definitive CRT.
- Soft Tissue Sarcomas (High-Risk):
- Neoadjuvant RT ± Chemo (e.g., Doxorubicin/Ifosfamide) for limb preservation, large/deep tumours. Adjuvant if upfront surgery.
⭐ For locally advanced rectal cancer, neoadjuvant chemoradiotherapy (CRT) followed by Total Mesorectal Excision (TME) is the standard of care, significantly improving local control and sphincter preservation rates.
High‑Yield Points - ⚡ Biggest Takeaways
- Neoadjuvant therapy: given before surgery to downstage tumors, improving resectability.
- Adjuvant therapy: given after surgery to target micrometastases, reducing recurrence.
- Modalities: chemotherapy, radiotherapy, hormone therapy, immunotherapy, targeted therapy.
- Indications vary by tumor type, stage, grade, and patient factors.
- Response assessment (e.g., RECIST for neoadjuvant) guides further treatment.
- Timing: Adjuvant therapy usually starts 4-6 weeks post-surgery.
- Goals: Improve disease-free survival (DFS) and overall survival (OS).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

