Metastasectomy: Basics - Goal-Oriented Snipping
- Definition: Surgical excision of metastatic lesions.
- Primary Aim: Improve overall survival (OS); potential cure in oligometastases.
- Other Aims: Symptom palliation, diagnosis, local control.
- Core Principle: Achieve complete R0 resection (microscopically negative margins).
- Crucial Selection Factors:
- Primary tumor controlled.
- Patient fit for major surgery (ECOG 0-1).
- Resectable metastatic disease (number, location).
- Longer disease-free interval (DFI) often favorable.
⭐ Complete (R0) resection is the most significant prognostic factor for survival after metastasectomy.
Patient Selection Criteria - Picking Prime Patients
- Primary Tumor: Controlled or controllable (no active local disease).
- Metastases:
- Resectable with clear margins (R0 resection is the goal).
- Limited number (oligometastases, typically defined as ≤ 3-5 lesions).
- No widespread, unresectable disease elsewhere.
- Patient Status:
- Good performance status (e.g., ECOG 0-1, Karnofsky >70).
- Adequate organ function to tolerate major surgery.
- Timing & Biology:
- Longer Disease-Free Interval (DFI) from primary treatment (e.g., > 12-24 months preferred).
- Slow tumor doubling time.
⭐ For pulmonary metastasectomy, a DFI > 36 months, a single metastasis, and complete (R0) resection are strong positive prognostic factors.
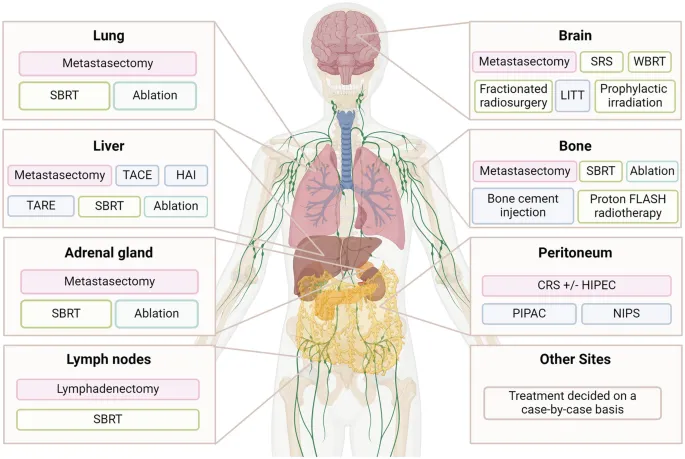
Site-Specific Metastasectomy - Hotspot Hitlist
- Liver (Hepatic):
- Common for CRC. Key: R0 resection, Future Liver Remnant (FLR >20-25% normal, >30-40% chemo-exposed).
- Parenchymal-sparing preferred.
⭐ For CRC liver metastases, 5-year survival post-resection can reach 40-50%.
- Lung (Pulmonary):
- For CRC, sarcoma, RCC. Key: Primary controlled, R0 resection, pulmonary reserve (FEV1 >1L or >30-40% pred).
- Wedge resection common, VATS ideal.
- Brain:
- Solitary/few lesions, controlled primary.
- Often + Stereotactic Radiosurgery (SRS)/Whole Brain Radiotherapy (WBRT).
- Primaries: Lung, breast, melanoma.
- Peritoneum (CRS):
- For peritoneal surface disease (CRC, ovarian, appendiceal).
- Goal: Complete cytoreduction (CC-0/CC-1). Often + HIPEC.
- Adrenal:
- Isolated metastasis (e.g., lung, RCC).
- Laparoscopic adrenalectomy if feasible.
Prognosis & Combined Therapy - Future Factors & Friends
- Prognostic Factors (Influence Outcomes):
- Favorable (Friends):
- Long Disease-Free Interval (DFI > 12-24 months).
- Solitary or few metastases (e.g., < 3-5).
- Complete (R0) resection achievable.
- Primary tumor type (e.g., Colorectal CRC, Renal RCC).
- Good patient performance status (ECOG 0-1).
- Unfavorable (Foes): Short DFI, multiple/bilateral mets, incomplete resection (R1/R2), aggressive tumor biology.
- Favorable (Friends):
- Combined Therapy (Synergy for Success):
- Systemic Therapy: Chemotherapy, immunotherapy, targeted therapy.
- Neoadjuvant: To downstage, assess tumor biology.
- Adjuvant: Eradicate micrometastases, improve DFS/OS.
- Other Local Therapies: SBRT, RFA, MWA for unresectable, residual, or new lesions.
- Systemic Therapy: Chemotherapy, immunotherapy, targeted therapy.
- Future Directions:
- Liquid biopsies (ctDNA) for early detection & monitoring.
- Advanced molecular profiling for personalized therapy selection.
⭐ The single most important prognostic factor for survival following metastasectomy is achieving a complete (R0) resection.
High‑Yield Points - ⚡ Biggest Takeaways
- Metastasectomy: surgical resection of metastases, aiming for cure or improved survival.
- Best for oligometastatic disease (limited number/sites of metastases).
- Prognostic factors: disease-free interval (DFI), R0 resection, number/site of metastases.
- Common sites: liver (colorectal cancer), lung (sarcoma, colorectal), brain.
- Crucial selection: good performance status, controlled primary tumor.
- Pulmonary metastasectomy: wedge resection common; R0 resection vital.
- Liver metastasectomy: requires adequate future liver remnant (FLR).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

