Single Incision Laparoscopic Surgery - One Port Wonder
- Concept: All surgical instruments and laparoscope enter the abdomen via ONE multi-channel port placed in a single skin incision (often umbilical, ~1.5-2.5 cm).
- Aliases: LESS (Laparo-Endoscopic Single-Site), SPA (Single Port Access).
- Vs. Conventional Laparoscopy: Single incision vs. multiple (3-5) ports.
- Benefits:
- Enhanced cosmesis (near "scarless" surgery).
- Potential for ↓ pain & quicker recovery.
- Limitations:
- Technical difficulty: instrument clashing, ↓ triangulation.
- Requires specialized articulating/curved instruments.
- Longer operative times initially.
⭐ The umbilicus is the most common access site for SILS, leveraging its natural scar-hiding properties and embryological significance as a natural orifice remnant for access.
Single Incision Laparoscopic Surgery - Unlocking the One Hole
- Concept: Laparoscopy via one small umbilical incision (typically 1.5-2.5 cm), often concealed within the navel.
- Key Benefits: Superior cosmesis ("scarless"); potential for ↓pain, faster recovery.
- Access Methods:
- Single multi-channel port (e.g., SILS™ Port, GelPOINT®) for instruments & camera.
- Multiple trocars via separate fascial stabs within the single skin incision.
- Specialized Instrumentation:
- Articulating, rotaculating, or pre-bent instruments to overcome space limits.
- Specialized laparoscopes (e.g., 5mm, 30° or flexible tip).
- Core Challenges:
- Instrument "sword fighting" (clashing) & internal crowding.
- Reduced triangulation, increasing technical difficulty & learning curve.
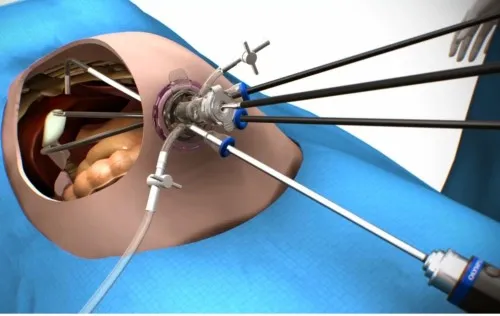
⭐ SILS offers superior cosmesis, its main advantage, with the scar typically hidden within the umbilicus.
Single Incision Laparoscopic Surgery - Gains & Pains
Gains (Advantages):
- Cosmesis: Superior; single, often hidden umbilical scar.
- Pain: ↓ Postoperative pain & analgesic needs.
- Port Complications: Potentially ↓ port-site issues (e.g., infection, hernia).
- Recovery: Faster return to normal activities.
- Patient Satisfaction: High, mainly due to cosmetic results.
Pains (Disadvantages & Challenges):
- Ergonomics: Significant; instrument clashing ("sword fighting"), loss of triangulation, ↓ surgeon comfort.
- Learning Curve: Steeper; requires specific skill acquisition.
- Operative Time: Can be longer, especially during initial experience.
- Instrumentation: Needs specialized, often articulating & costlier, instruments.
- Indications: Limited; unsuitable for very complex procedures or some patient groups (e.g., severe obesity).
- Fascial Defect: Larger single incision needs meticulous closure to prevent hernia.
⭐ Loss of triangulation and the "chopstick effect" (instrument crowding and clashing) are the most significant ergonomic challenges in SILS, impacting surgical dexterity and potentially increasing operative time.
Single Incision Laparoscopic Surgery - Scope & Stops
-
Scope (Indications):
- Cholecystectomy, appendectomy
- Benign adnexal masses, hysterectomy
- Select colectomies, nephrectomy
- Sleeve gastrectomy
-
Patient Selection Criteria:
- BMI < 30-35 kg/m² (ideal)
- No extensive prior abdominal surgeries
- Localized, non-bulky pathology
-
Stops (Contraindications):
- Absolute: Hemodynamic instability, generalized peritonitis, uncorrectable coagulopathy.
- Relative: Morbid obesity (BMI > 40 kg/m²), large/malignant tumors, extensive adhesions, surgeon inexperience.
-
Specific Complications & Considerations:
- ↑ Risk of incisional hernia at port site.
- Instrument crowding/clashing, loss of triangulation.
- Longer learning curve; may convert to standard laparoscopy.
⭐ The primary advantage of SILS is improved cosmesis due to a single, often umbilical, incision, making it a patient-preferred option for suitable cases.
High‑Yield Points - ⚡ Biggest Takeaways
- SILS utilizes a single umbilical incision (often 2-2.5 cm) for all instruments.
- Primary benefit: Superior cosmesis with scar hidden in the umbilicus.
- Requires specialized instruments (articulating, curved) for co-axial instrument passage.
- Loss of triangulation and instrument clashing are key technical challenges.
- Features a steeper learning curve compared to multi-port laparoscopy.
- Common procedures: cholecystectomy, appendectomy, and select colectomies.
- Incisional hernia risk at port site; meticulous fascial closure is vital.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

