Lap UGIE Fundamentals - Peeking & Prepping
- Pneumoperitoneum:
- CO2 insufflation: 12-15 mmHg.
- Access: Veress (blind), Hasson (open), optical.
- Physiology: ↑IAP → CV (↑MAP, ↑SVR) & respiratory effects.
- Patient & OR Setup:
- Position: Supine, reverse Trendelenburg, arms tucked.
- OR: Ergonomic monitors, insufflator, light source.
- Anesthesia: GA, ETT, muscle relaxation.
- Ports & Instruments:
- Ports: Triangulation; umbilical camera port.
- Trocars (5-12mm), Laparoscope (0°/30°).
- Instruments: Graspers, dissectors, energy (mono/bipolar, ultrasonic).
- Pre-op Prep:
- NPO, consent.
- DVT & antibiotic prophylaxis.
⭐ Veress needle entry is typically at Palmer's point (left subcostal margin, mid-clavicular line) in patients with previous midline surgery to avoid adhesions.
Lap Fundoplication - GERD Gone Gently
Gold standard surgical treatment for severe/refractory Gastroesophageal Reflux Disease (GERD) and large hiatus hernias. Aims to restore Lower Esophageal Sphincter (LES) competence.
- Indications:
- Chronic GERD unresponsive to Proton Pump Inhibitors (PPIs)
- GERD complications: Barrett's esophagus, peptic stricture, severe esophagitis (e.g., LA Grade C/D)
- Symptomatic paraesophageal or large mixed hiatus hernia (Type II-IV)
- Pre-operative Essentials:
- Upper GI Endoscopy (EGD) + biopsy
- Esophageal manometry (crucial for wrap choice, assesses peristalsis)
- 24-hour pH monitoring (confirms abnormal acid exposure)
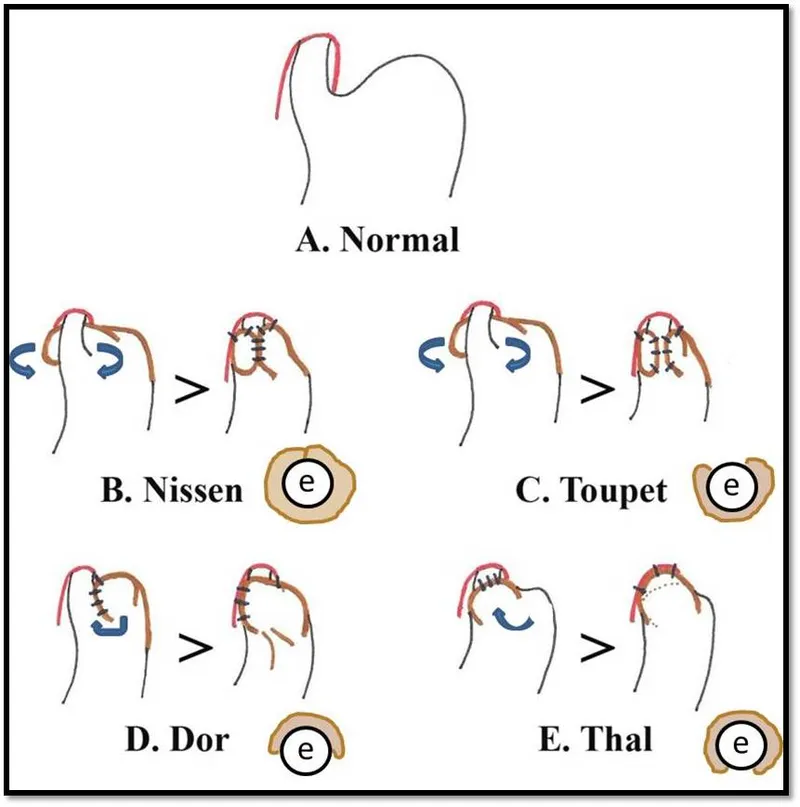
- Types of Fundoplication (Wrap):
- Nissen: Total (360°) fundoplication; most common, highest anti-reflux efficacy.
- Toupet: Posterior partial (270°) fundoplication; less postoperative dysphagia.
- Dor: Anterior partial (180-200°) fundoplication; often used with Heller's myotomy for achalasia.
- Key Complications:
- Dysphagia (most frequent, often transient)
- Gas bloat syndrome
- Wrap failure (slippage, migration, disruption), recurrent hernia
⭐ Toupet (posterior partial 270°) fundoplication is generally preferred over Nissen in patients with documented impaired esophageal motility to minimize the risk and severity of postoperative dysphagia.
Lap Heller Myotomy - Esophageal Ease
- Definitive surgical treatment for Achalasia Cardia, relieving dysphagia.
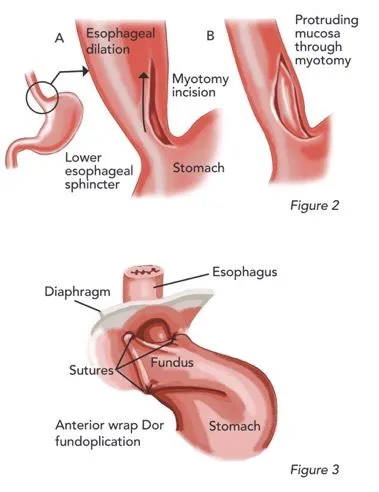
- Procedure: Longitudinal extramucosal myotomy of Lower Esophageal Sphincter (LES) & proximal stomach.
- Myotomy length: 6-7 cm on esophagus, 2-3 cm onto gastric cardia.
- Commonly combined with an anti-reflux procedure (fundoplication) to prevent iatrogenic GERD:
- Dor fundoplication (anterior partial, 180-200°) is frequently preferred.
- Toupet fundoplication (posterior partial, 270°) is an alternative.
- Key Complications: Esophageal perforation (most common intra-operatively), postoperative GERD, persistent/recurrent dysphagia.
- High success rates (>90%) in relieving symptoms.
⭐ The most common reason for persistent dysphagia after Heller myotomy is an incomplete myotomy, particularly inadequate extension onto the gastric cardia or too tight fundoplication wrap.
Lap PPU & Bariatric Bits - Ulcers & Weight Wins
- Lap PPU Repair (Graham Patch)
- Indication: Perforated peptic ulcer (PPU), commonly duodenal.
- Diagnosis: Pneumoperitoneum (X-ray/CT). Free air under diaphragm.
- Procedure: Laparoscopic omental (Graham) patch over perforation.
- Benefits: ↓pain, ↓hospital stay, ↑earlier recovery & return to work.
- Bariatric Surgery
- Indications: BMI ≥ 40 kg/m², or BMI ≥ 35 kg/m² with major comorbidities (e.g., T2DM, OSA, HTN).
- Common Procedures:
- Lap Sleeve Gastrectomy (LSG): Restrictive. Removes ~80% of stomach along greater curvature.
- Roux-en-Y Gastric Bypass (RYGB): Restrictive & malabsorptive. Small gastric pouch (~30ml) + biliopancreatic & Roux limb.
- ⚠️ Key Risks: Anastomotic leaks, DVT/PE, nutritional deficiencies (Fe, B12, Ca, Vit D), dumping syndrome (esp. RYGB), internal hernias (RYGB).
> ⭐ Sleeve gastrectomy is currently the most performed bariatric procedure worldwide due to its relative simplicity and good outcomes.
High‑Yield Points - ⚡ Biggest Takeaways
- Laparoscopic Nissen fundoplication: gold standard for GERD; watch for dysphagia, gas bloat.
- Laparoscopic Heller's myotomy (+ partial fundoplication): treatment of choice for achalasia cardia.
- Pneumoperitoneum (CO2): causes shoulder tip pain (phrenic nerve); risks gas embolism, hypercarbia.
- Laparoscopic omental patch repair: standard for perforated peptic ulcer.
- Laparoscopic gastrectomy: for early gastric cancer, offers MIS benefits with comparable oncological outcomes.
- Key MIS benefits: ↓ pain, ↓ hospital stay, ↑ recovery speed, better cosmesis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

