Indications & Contraindications - Snip or No Snip?
- Indications:
- Symptomatic gallstones (biliary colic, cholecystitis)
- Acalculous cholecystitis
- Gallstone pancreatitis (post-resolution)
- GB polyps (>1 cm / symptomatic)
- Porcelain gallbladder (malignancy risk)
- Contraindications (Absolute):
- Uncontrolled coagulopathy
- Unfit for GA/pneumoperitoneum
- Diffuse peritonitis
- Suspected GB cancer (open preferred)
- Contraindications (Relative):
- Severe cardiorespiratory disease
- Cirrhosis & portal HTN (↑ bleeding)
- Pregnancy (safest 2nd trimester)
- Multiple prior upper abdominal surgeries
⭐ Symptomatic cholelithiasis remains the primary indication for laparoscopic cholecystectomy.
Pre-op Prep & Patient Positioning - Setting the Stage
- Pre-operative:
- Informed consent obtained.
- NPO: 6-8 hrs solids, 2 hrs clear fluids.
- IV access, prophylactic antibiotics (e.g., Cefazolin 1-2g).
- DVT prophylaxis (risk-stratified).
- Patient Positioning:
- Supine initially.
- Intra-op: Reverse Trendelenburg (15-20°), slight left lateral tilt.
- Arms: Typically one abducted, one tucked. Secure patient well.
⭐ Reverse Trendelenburg position is crucial for optimal visualization by displacing bowel inferiorly.
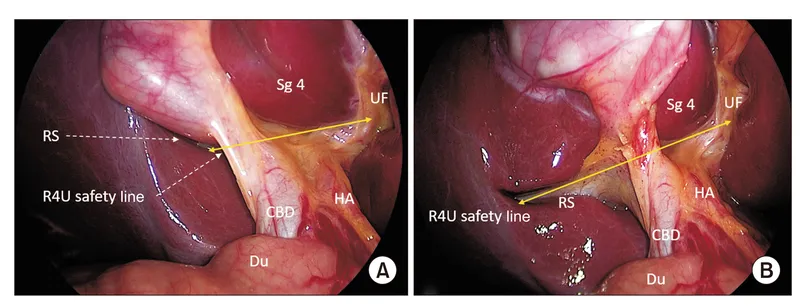
Surgical Anatomy & Critical View - X Marks the Spot!
- Calot's Triangle (Hepatocystic):
- Boundaries: Cystic duct (inf.), Common Hepatic Duct (med.), Liver edge (sup.).
- Contents: Cystic artery (key!), Calot's node.
- Critical View of Safety (CVS): Prevents Bile Duct Injury (BDI).
- Clear hepatocystic triangle.
- Expose cystic plate (GB base off liver).
- Only 2 structures enter GB: cystic duct & artery.
- Key Landmarks:
- Rouviere's Sulcus: Plane of CBD.
- Moynihan's Hump: Coiled RHA (⚠️ risk).
⭐ The cystic artery usually originates from the right hepatic artery within Calot's triangle.
Lap Chole Steps & Ports - Keyhole Magic
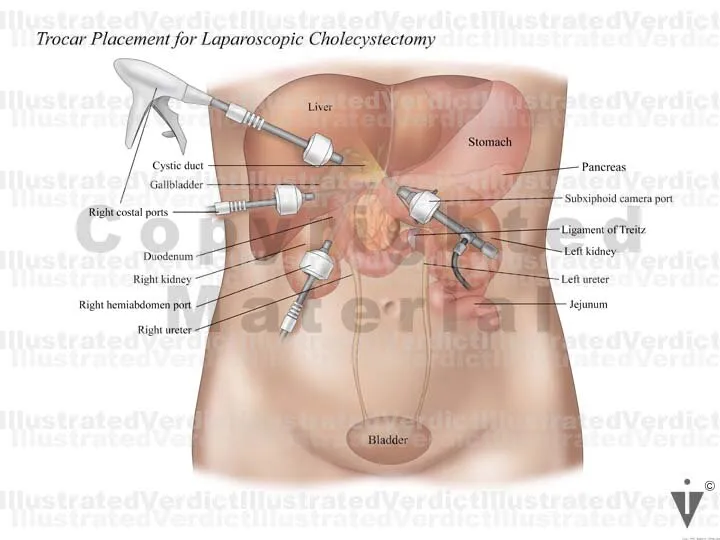
- Ports (Usually 4):
- Umbilical (10-12mm): Camera, CO2 insufflation (Veress/Hasson).
- Epigastric (10mm): Main working port (dissectors, clippers).
- Right Mid-Clavicular (5mm): Fundal retraction (superior-lateral).
- Right Anterior Axillary (5mm): Infundibular retraction (lateral).
- Key Steps:
- Pneumoperitoneum (CO2 to 12-15 mmHg).
- Port insertion.
- Gallbladder retraction.
- Calot's triangle dissection.
- Achieve Critical View of Safety (CVS).
- Clip & divide cystic duct & artery.
- Dissect gallbladder from liver bed.
- Specimen retrieval.
- Hemostasis & closure.
⭐ The Critical View of Safety (CVS) - ensuring only two structures (cystic duct, cystic artery) enter the gallbladder base - is paramount to prevent bile duct injury.
Complications & Conversions - Uh Oh Moments
-
Intra-op Complications:
- Bile Duct Injury (BDI): Most feared; Strasberg classification.
- Bleeding: Cystic artery/vein, liver bed.
- Bowel/Vascular injury.
-
Post-op Complications:
- Port-site hernia/infection.
- Retained CBD stones; Bile leak.
- Post-Cholecystectomy Syndrome (PCS).
-
Conversion to Open Surgery Triggers (HALT-IF): 📌
- Hemorrhage (uncontrolled).
- Anatomy unclear (Calot's Δ obscured).
- Large CBD stone (unexpected/unmanageable).
- Tumor suspected (e.g., incidental Gallbladder Cancer).
- Injury (BDI, bowel).
- Failure to progress/Dense adhesions.
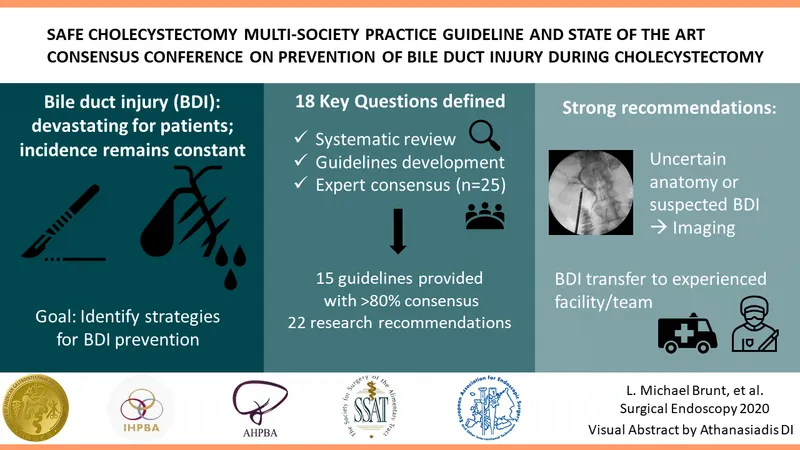
⭐ The "Critical View of Safety" (CVS) technique is paramount to prevent BDI. Failure to achieve CVS is a strong indication for conversion to open surgery.
Post-op Care & Advantages - Swift & Smooth
- Post-operative Care:
- Early ambulation encouraged.
- Diet: Clear liquids, advanced as tolerated.
- Pain management: Multimodal (NSAIDs, minimal opioids).
- Discharge: Typically same day or within 24 hours.
- Wound care: Keep dressings clean, dry.
- Advantages (Laparoscopic vs. Open):
- Reduced post-operative pain.
- Shorter hospital stay (↓).
- Faster return to activity (↑).
- Improved cosmesis (smaller scars).
- Lower risk of ileus & respiratory complications.
⭐ Most patients resume normal activities within 1 week post-laparoscopic cholecystectomy.
High‑Yield Points - ⚡ Biggest Takeaways
- Laparoscopic cholecystectomy is the gold standard for symptomatic gallstones.
- Critical View of Safety (CVS) is crucial to prevent bile duct injury (BDI).
- Key complications include BDI, vascular injury, and post-op bile leak.
- Pneumoperitoneum is usually established with CO2 at 12-15 mmHg.
- Calot's triangle (cystic duct, common hepatic duct, liver edge) is key anatomy.
- Conversion to open surgery is a safety measure, not a complication.
- Early cholecystectomy is preferred for acute cholecystitis within 72 hours.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

