MIS Complications Overview - Tiny Cuts, Key Concerns
- MIS: Small incisions, specialized tools. Benefits: ↓ pain, faster recovery, ↓ scarring, shorter hospital stay.
- Risks: Mirrors open surgery risks plus unique MIS issues (e.g., related to access, insufflation).
- General Risks (MIS Nuances):
- Infection: ↓ SSI rates typical; deep infections remain a concern.
- Bleeding: Initial detection/control can be challenging.
- DVT/PE: Early mobility helps; prolonged procedures ↑ risk.
- MIS-Specific Issues:
- Access: Trocar injury (vessels, bowel), port-site hernia.
- Insufflation (CO₂): Embolism (rare), cardiovascular/respiratory strain.
- Energy Devices: Unintended thermal injury to adjacent structures.
⭐ Laparoscopic cholecystectomy generally demonstrates lower wound infection rates (~1%) versus open procedures (~5-8%).
Access & Pneumoperitoneum - Entry Errors, Gas Grief
- Access:
- Veress needle: Blind; risk of injury.
- Trocars: Bladed (↑injury), Bladeless (dilating), Optical (visual).
- Max pressure: 12-15 mmHg.
- Entry Injuries:
- Vascular: Aorta, IVC, iliacs.
⭐ Most common: Right common iliac artery.
- Visceral: Bowel (most common), bladder.
- Solid organ: Liver, spleen.
- Palmer's Point: L mid-clavicular, 3cm below costal margin (alt. entry).
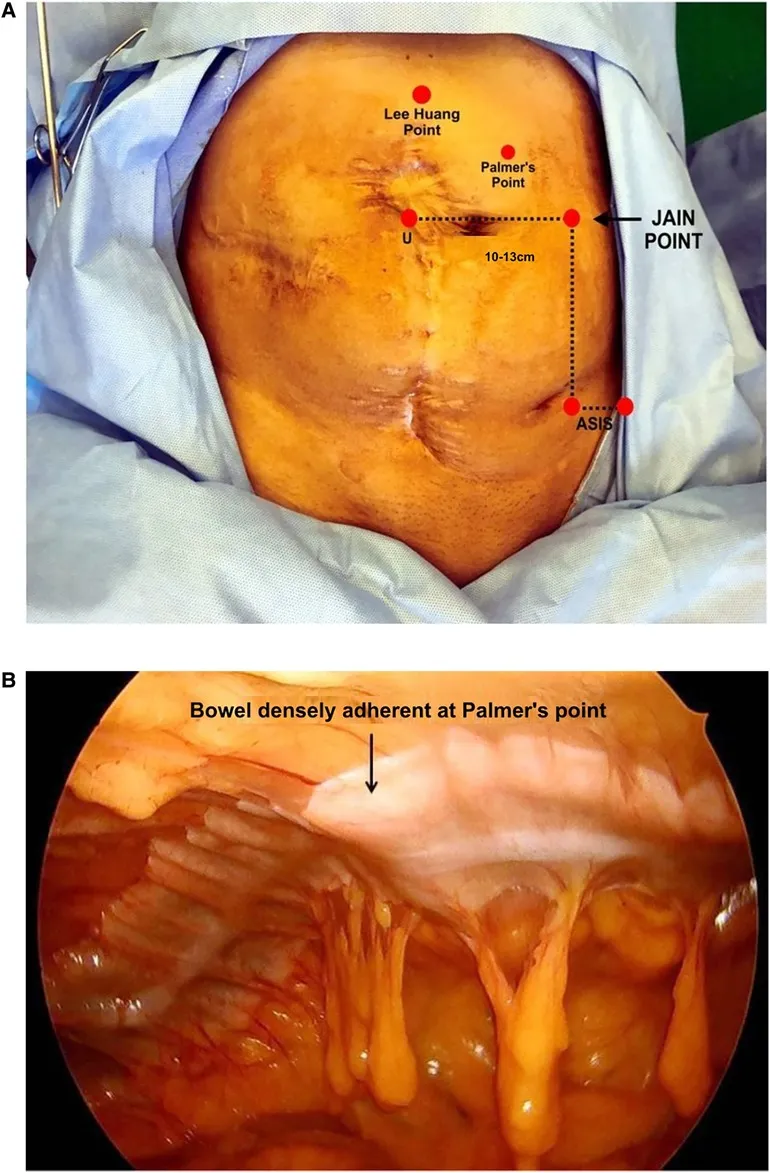
- Vascular: Aorta, IVC, iliacs.
- Pneumoperitoneum ($CO_2$):
- Effects: $CO_2 + H_2O \leftrightarrow H_2CO_3 \leftrightarrow H^+ + HCO_3^-$ (resp. acidosis).
Parameter Trend HR ↑ then ↓ BP ↑ ET$CO_2$ ↑ - Complications:
- Subcutaneous emphysema.
- Gas Embolism (⚠️): 📌 Signs (Hypotension, ET$CO_2$ ↓ sudden, Arrhythmia, Desaturation, Sound: mill-wheel murmur). Mgmt: Durant's (LLD, Trendelenburg).
- Effects: $CO_2 + H_2O \leftrightarrow H_2CO_3 \leftrightarrow H^+ + HCO_3^-$ (resp. acidosis).
Intraop & Energy Devices - Operative Oops, Zap Traps
- Intraop Injuries:
- Types: Mechanical (trocars, instruments), Thermal (energy devices).
- Common sites:
- Bowel: Most common delayed diagnosis; thermal injury often missed.
- Bladder: Trocar, dissection.
- Ureteric: Near uterine artery/pelvic brim.
- Recognition: Direct view, leak tests. Early detection crucial.
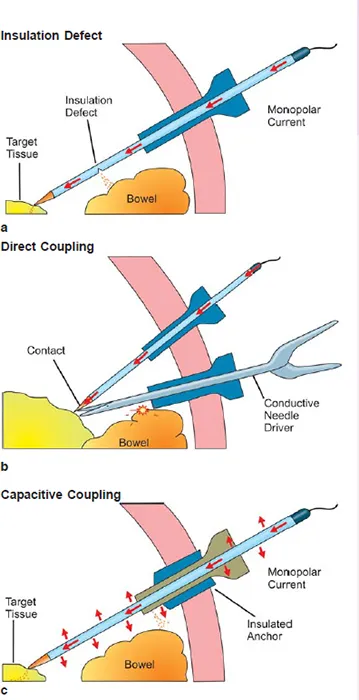
- Energy Device Complications: 📌 Mnemonic (Monopolar): BIC (Burns, Insulation failure, Capacitive coupling).
- Comparison:
Energy Mechanism Key Risks Monopolar Current via patient to pad Direct/capacitive coupling, insulation failure, alternate site burns Bipolar Current between tips Direct thermal spread Ultrasonic Vibration Lateral thermal spread, mechanical trauma
⭐ Capacitive coupling: risk unique to monopolar MIS, especially with hybrid trocars.
- Comparison:
- Prevention: Check insulation, lowest power, avoid "buzzing" metal, prefer bipolar near vital structures.
- Bleeding: Limited access challenges control. Use clips, energy, sutures.
Post-Op & Long-Term - Aftermath Woes, Lasting Marks
- Port-Site Complications:
- Infection, hematoma.
- Hernia: Incisional, with Richter's type (bowel wall entrapment) being common.
⭐ Richter's hernia is more common at port sites than other incisional hernias.
- Port-Site Metastasis (PSM):
- Tumor cell implantation. Risk factors: aggressive tumors, inadequate specimen retrieval. Prevention: wound protectors, careful extraction.
- Delayed Presentations:
- Missed bowel injury: Presents as peritonitis days later.
- Diaphragmatic hernia: Especially after upper abdominal/thoracoscopic procedures.
- Neuropathies:
- Patient positioning can cause nerve injury (e.g., brachial plexus, common peroneal).
- Adhesions:
- Less frequent than open surgery, but still occur; risk of bowel obstruction.
High‑Yield Points - ⚡ Biggest Takeaways
- Access injuries to vessels, bowel, or bladder are critical risks, especially at primary port insertion.
- CO2 gas embolism: sudden ↓ETCO2, hypotension, mill-wheel murmur; manage with left lateral decubitus, Trendelenburg.
- Hypercarbia & respiratory acidosis from CO2 absorption are common; monitor ETCO2.
- Port-site hernias for ports >10 mm; fascial closure is key to prevention.
- Thermal bowel injury from electrosurgery often presents late.
- Nerve injuries from prolonged/improper positioning; shoulder tip pain from diaphragmatic irritation.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

