Gross & Segmental Anatomy - Liver's Grand Design
- Gross: RUQ. Glisson's capsule. Bare area (no peritoneum).
- Lobes (Anatomical): R, L, Caudate, Quadrate. Falciform ligament divides R/L.
- Lobes (Functional/Surgical): True R/L by Cantlie's line (IVC fossa to GB fossa).
- Ligaments: Falciform, Coronary, Triangular, Teres hepatis, Venosum.
- Segmental (Couinaud): 8 functional segments, portal triad inflow each.
- Cantlie's Line: Divides R (V-VIII) & L (I-IV) hemilivers. MHV runs in it.
- Segment I (Caudate): Posterior, distinct supply/drainage to IVC.
- Left Hemiliver:
- Lateral (II, III); Medial (IVa sup, IVb inf).
- Right Hemiliver:
- Anterior (V inf, VIII sup); Posterior (VI inf, VII sup).
- Hepatic Veins (HV): Intersegmental. RHV, MHV, LHV.
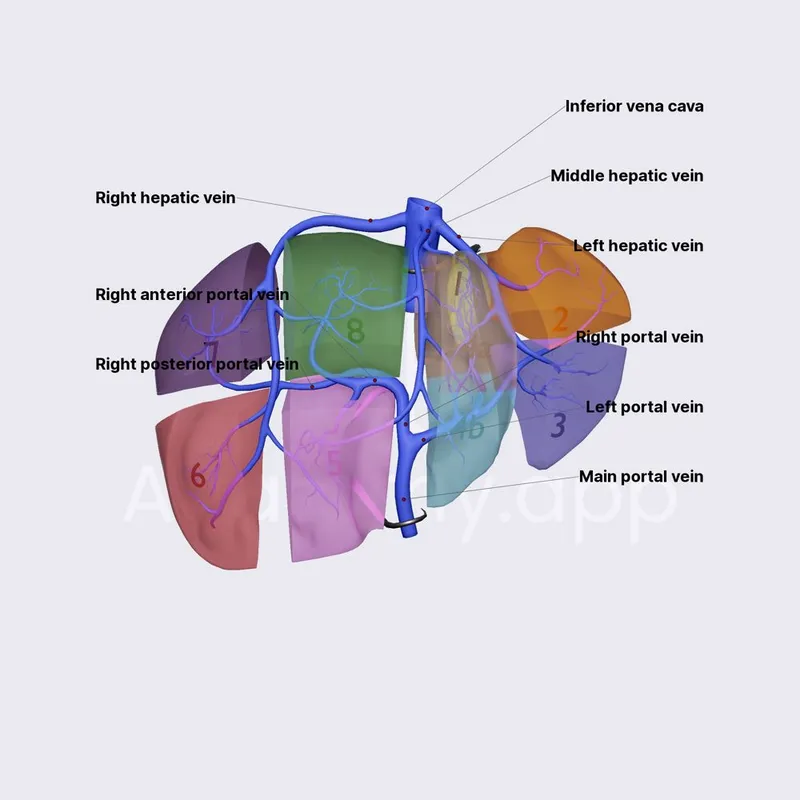
⭐ Cantlie's line, demarcating true R/L hemilivers (portal & hepatic venous anatomy based), is key for major hepatectomies.
Vascular & Biliary Tree - Lifeblood & Bile Flow
- Dual Blood Supply:
- Portal Vein (PV): ~75% of blood flow; nutrient-rich, O₂-poor.
- Hepatic Artery (HA): ~25% of blood flow; O₂-rich.
- Components run together in portal triads (PV, HA, Bile Duct). 📌 Mnemonic: "PhD" (Portal vein, Hepatic artery, Ductus choledochus).
- Venous Drainage: Hepatic veins → Inferior Vena Cava (IVC).
- Biliary Drainage Pathway:
- Intrahepatic: Canaliculi → Ducts of Hering → Interlobular ducts → R/L Hepatic Ducts.
- Extrahepatic: R/L Hepatic Ducts merge → Common Hepatic Duct (CHD).
- CHD + Cystic Duct (from Gallbladder) → Common Bile Duct (CBD).
- CBD + Main Pancreatic Duct → Ampulla of Vater (regulated by Sphincter of Oddi) → Duodenum.
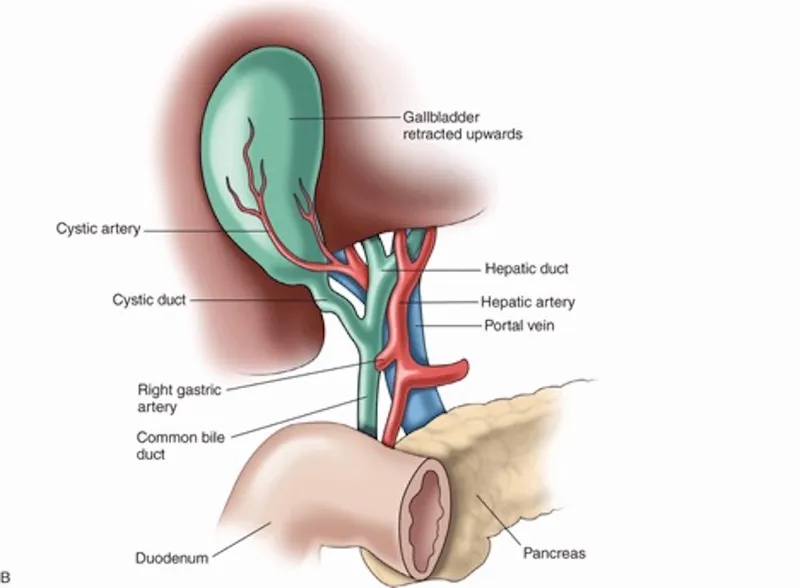
⭐ Calot's Triangle (Hepatobiliary Triangle): Critical surgical landmark. Boundaries: Cystic duct (inferiorly), Common Hepatic Duct (medially), Inferior surface of liver (superiorly). Cystic artery is typically found within.
Microscopic Anatomy & Zonation - Cellular Work Zones
- Hepatic Acinus (Rappaport): Functional unit. Blood flows from portal triad (PT) to central vein (CV).
- Space of Disse: Between hepatocytes & sinusoids; contains stellate (Ito) cells (Vitamin A storage, fibrosis).
- Kupffer cells: Macrophages lining sinusoids.
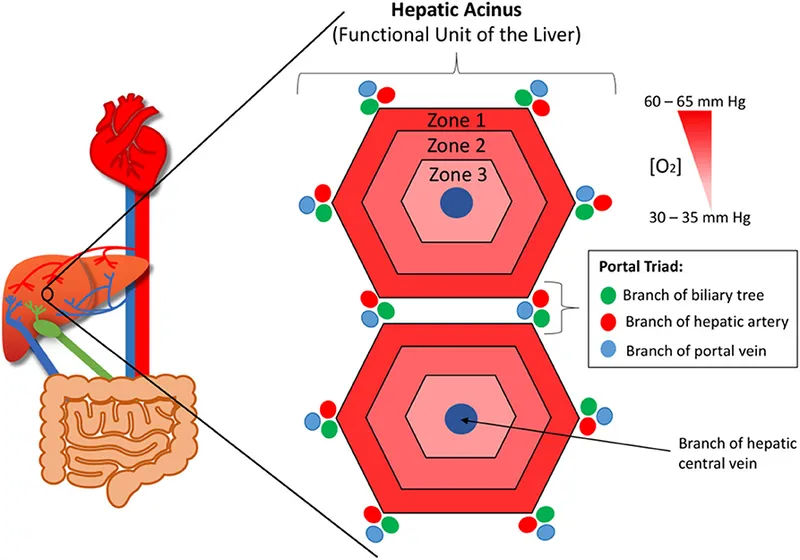
⭐ Zone 3 (Pericentral) is most vulnerable to ischemic injury and toxic damage (e.g., paracetamol, CCl₄) due to its lowest oxygen supply and high concentration of CYP450 enzymes.
- 📌 Zonal Vulnerability: Zone 1 (Viral, Phosphorus); Zone 3 (Ischemia, Toxins, Alcohol - "VITA").
Major Liver Functions - The Metabolic Multitasker
- Metabolic Hub:
- Carbs: Glucose homeostasis (glycogenesis, glycogenolysis, gluconeogenesis).
- Proteins: Synthesis (albumin, clotting factors); urea cycle ($NH_3 \rightarrow$ urea).
- Lipids: Cholesterol, lipoproteins, bile acids, ketogenesis.
- Synthetic Powerhouse:
- Albumin (oncotic pressure).
- Clotting Factors (II, VII, IX, X, Protein C, S).
- Bile (fat digestion/absorption).
- Detoxification & Excretion:
- Bilirubin conjugation & excretion.
- Drug metabolism (CYP450, Phase I/II).
- Hormone inactivation.
- Storage: Glycogen, Vitamins (A,D,E,K, B12), Iron (ferritin), Copper.
- Immunity: Kupffer cells (phagocytosis, cytokine release).
⭐ The liver synthesizes most coagulation factors, except Factor VIII (endothelial cells) & vWF (endothelial cells, megakaryocytes).
High‑Yield Points - ⚡ Biggest Takeaways
- Couinaud classification: 8 functional liver segments.
- Portal triad: Portal vein, hepatic artery, bile duct within Glisson's capsule.
- Dual blood supply: ~75% portal vein (nutrients), ~25% hepatic artery (oxygen).
- Kupffer cells: Resident macrophages in liver sinusoids.
- Space of Disse: Contains stellate (Ito) cells (Vitamin A storage, fibrosis).
- Hepatic acinus: Zone 1 (periportal) best oxygenated; Zone 3 (centrilobular) most vulnerable to ischemia & toxins.
- Major functions: Bile production, detoxification (e.g., urea cycle), albumin synthesis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

