HCC Basics - Liver's Dark Side
- Definition: Primary malignancy of the liver arising from hepatocytes.
- Epidemiology: 6th most common cancer worldwide; 3rd leading cause of cancer death. Significant burden in India due to Hepatitis B (HBV) & C (HCV) prevalence.
- Risk Factors:
- Chronic Viral Hepatitis (HBV, HCV)
- Alcoholic Liver Disease
- Non-alcoholic Fatty Liver Disease (NAFLD) / Non-alcoholic steatohepatitis (NASH)
- Aflatoxin B1 exposure (e.g., contaminated groundnuts, corn)
- Cirrhosis (present in ~80-90% of HCC cases, from any cause)
- 📌 Mnemonic: 'HH AAN' (HBV, HCV, Alcohol, Aflatoxin, NAFLD)
⭐ Hepatocellular carcinoma (HCC) is the most common primary malignant tumor of the liver, accounting for approximately 75-85% of all primary liver cancers globally.
Diagnosis - Spotting the Enemy
- Screening (High-Risk: Cirrhosis, Chronic HBV/HCV):
- Ultrasound (USG) every 6 months.
- Serum Alpha-fetoprotein (AFP); ↑AFP > 20 ng/mL is abnormal.
- Diagnostic Imaging (Key):
- Multiphase CT or MRI (preferred):
- Hallmark: Arterial Phase Hyperenhancement (APHE) & Portal/Venous Phase Washout.
- LI-RADS (Liver Imaging Reporting and Data System) used for characterization.

- Multiphase CT or MRI (preferred):
- Tumor Markers:
- AFP > 400 ng/mL highly suggestive.
- Others: AFP-L3, PIVKA-II (DCP).
- Biopsy:
- For LI-RADS 3/4 or indeterminate lesions.
- If imaging non-diagnostic, or in non-cirrhotic liver.
- Risk: Needle-track seeding.
⭐ In cirrhotic patients, classic imaging features (arterial phase hyperenhancement and portal/venous phase washout) are diagnostic for HCC, often obviating biopsy.
Staging & Prognosis - Sizing Up Trouble
- Core Principle: Staging dictates therapy & predicts survival.
- BCLC (Barcelona Clinic Liver Cancer): Gold standard.
⭐ The Barcelona Clinic Liver Cancer (BCLC) staging system is preferred as it links stage with treatment strategy and prognosis.
- BCLC Stages & Treatment:
- 0 (Very Early) / A (Early): Curative intent (resection, transplant, RFA).
- B (Intermediate): TACE.
- C (Advanced): Systemic therapy (e.g., Sorafenib, Lenvatinib).
- D (Terminal): Best supportive care.
- Key Prognostic Factors:
- Tumor burden: Size, number, vascular invasion (MVI).
- Liver function reserve: Child-Pugh score.
- Patient's overall health: ECOG performance status.
- Serum Biomarkers: AFP levels.
Treatment - Battle Plan
- BCLC 0 & A (Very Early & Early Stage): Curative Intent
- Surgical Resection: Child-Pugh A, adequate liver reserve.
- Liver Transplantation: 📌 Milan Criteria: Single tumor ≤5 cm, or up to 3 tumors each ≤3 cm; no macrovascular invasion; no extrahepatic spread.
- Ablation (RFA/MWA): For tumors <3 cm, non-surgical candidates.
- BCLC B (Intermediate Stage): Loco-regional Therapies
- TACE (Transarterial Chemoembolization): Multinodular, preserved liver function.
- TARE/SIRT (Y-90 Radioembolization): Alternative for TACE-unsuitable/refractory.
- BCLC C (Advanced Stage): Systemic Therapy
- Atezolizumab + Bevacizumab (Preferred 1st line).
- TKIs (Sorafenib, Lenvatinib).
- BCLC D (Terminal Stage): Best Supportive Care.
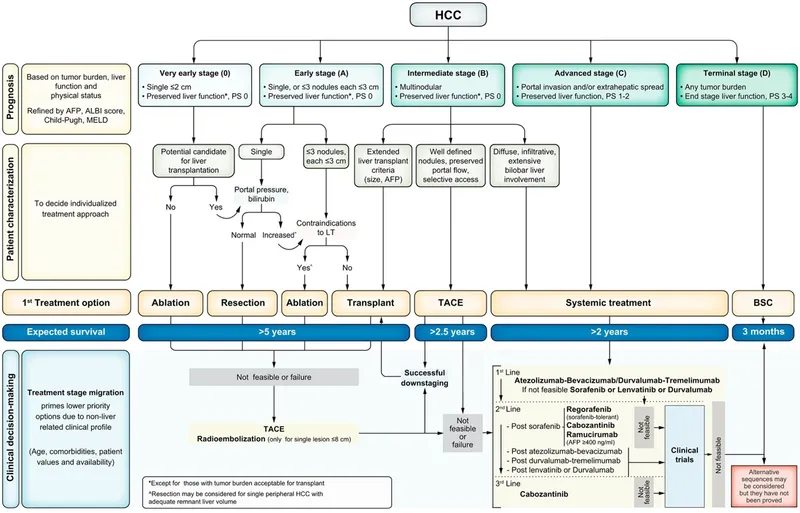
⭐ For advanced HCC (BCLC C), Atezolizumab-Bevacizumab is a preferred first-line systemic therapy, showing improved survival over Sorafenib monotherapy.
High‑Yield Points - ⚡ Biggest Takeaways
- Chronic Hepatitis B & C and cirrhosis are major risk factors for HCC.
- Screening in high-risk patients involves serum AFP and ultrasound every 6 months.
- Diagnosis often relies on characteristic imaging: arterial phase hyperenhancement and venous/delayed phase washout on CT/MRI.
- Milan criteria (single tumor ≤5 cm, or up to 3 tumors each ≤3 cm) are key for liver transplant eligibility.
- Surgical resection offers the best chance for cure in non-cirrhotic patients or those with well-compensated cirrhosis and solitary tumors.
- TACE (Transarterial Chemoembolization) is a primary palliative treatment for unresectable, localized HCC.
- Sorafenib and Lenvatinib are first-line systemic therapies for advanced HCC with preserved liver function.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

