ERCP Basics - Scope & Purpose
- ERCP: Endoscopic Retrograde Cholangiopancreatography. Combines upper GI endoscopy & fluoroscopy.
- Purpose: Primarily therapeutic; diagnostic role diminishing with MRCP/EUS.
- Diagnostic: Jaundice, suspected bile duct/pancreatic duct pathology.
- Therapeutic: Stone extraction, stenting, sphincterotomy, biopsy, stricture dilation.
- Key Indications: Biliary obstruction (stones, strictures, tumors), pancreatitis (selected cases), sphincter of Oddi dysfunction.
- Contraindications (Absolute): Patient refusal, perforated viscus, medically unstable.
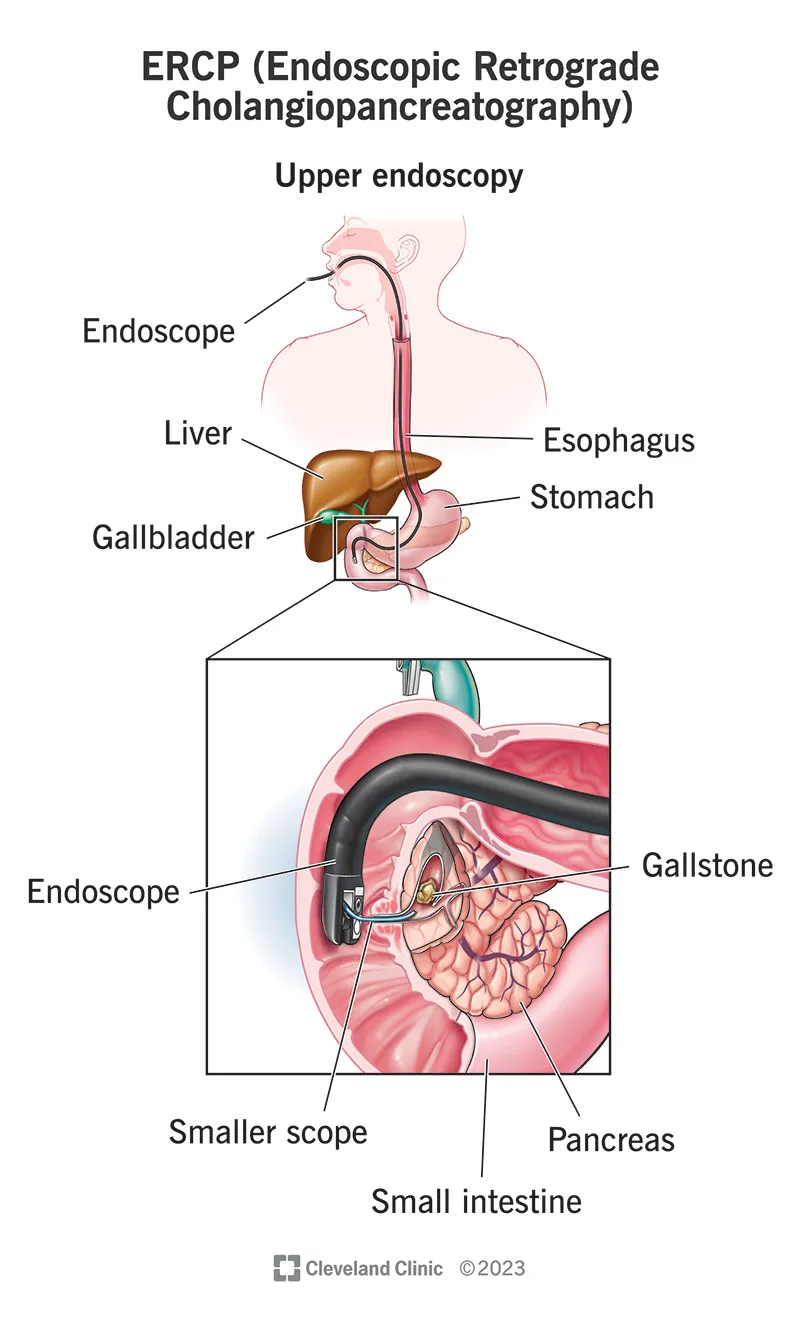
⭐ ERCP allows direct visualization and intervention in the biliary and pancreatic ducts, unlike MRCP which is purely diagnostic.
ERCP Technique - Duct Diving
- Prep: NPO 6-8 hrs, consent, IV. Antibiotics if high-risk (e.g., incomplete drainage).
- Position: Prone or left lateral.
- Sedation: Moderate sedation or MAC (propofol).
- Steps:
- Side-viewing duodenoscope to major papilla in D2.
- Selective guidewire-assisted cannulation of CBD/PD.
- Contrast injection under fluoroscopy (cholangio/pancreatogram).
- Therapeutic interventions: sphincterotomy, stone removal, dilation, stenting.

⭐ Guidewire-assisted cannulation is preferred; it reduces papillary trauma and significantly lowers post-ERCP pancreatitis (PEP) risk.
PEP - Fiery Aftermath
- Definition: Most common ERCP complication (1-10%); acute inflammation of pancreas post-procedure.
- Pathophysiology: Premature trypsinogen activation within pancreas → acinar cell injury.
- Diagnosis:
- New/worsened epigastric pain (often radiating to back).
- Serum amylase and/or lipase ≥3x ULN within 24 hours post-ERCP.
- Key Risk Factors:
- Patient-related: Young female, suspected Sphincter of Oddi Dysfunction (SOD), prior PEP, normal bilirubin.
- Procedure-related: Difficult/multiple cannulation attempts, pancreatic duct injection/acinarization, precut sphincterotomy.
- Prevention Strategies:
⭐ Prophylactic rectal NSAIDs (e.g., indomethacin 100mg) significantly reduce PEP risk, especially in high-risk patients.
- Management: Primarily supportive (NPO, IV fluids, analgesia). Severe cases require intensive care.
- 📌 PEP: Pain (abdominal), Elevated enzymes, Post-ERCP.
Other ERCP Risks - Beyond Pancreas
- Bleeding:
- Incidence: 0.3-2%.
- Risk factors: Sphincterotomy, coagulopathy, antiplatelet/anticoagulant use.
- Management: Endoscopic (clips, adrenaline), angioembolization, surgery.
- Infection (Cholangitis/Cholecystitis):
- Cholangitis: 0.5-3%; ↑ risk with incomplete drainage.
- Prophylactic antibiotics if biliary obstruction or anticipated incomplete drainage.
- Perforation:
- Incidence: 0.1-0.6%.
- Types: Duodenal (scope/guidewire), bile duct (guidewire), retroperitoneal (sphincterotomy).
⭐ Perforation risk is notably increased with pre-cut sphincterotomy and in patients with Billroth II anatomy.
- Cardiopulmonary Events:
- Aspiration, arrhythmias, MI, respiratory depression (often sedation-related).
- Sedation-Related Complications:
- Hypoxemia, hypotension.

ERCP Safety - Smooth Scoping
- Pre-procedure: Careful patient selection; assess indications, contraindications, coagulation.
- Antibiotic prophylaxis: For high-risk patients (e.g., biliary obstruction, incomplete drainage).
- Technique: Experienced operator, guidewire cannulation, limit attempts, judicious contrast.
- PEP Prophylaxis: Pancreatic duct stent and/or rectal NSAIDs (indomethacin 100mg) for high-risk.
⭐ Routine pre-procedural rectal indomethacin or diclofenac significantly reduces Post-ERCP Pancreatitis (PEP) incidence.
High‑Yield Points - ⚡ Biggest Takeaways
- ERCP: Primarily therapeutic for biliary (e.g., CBD stones, strictures) & pancreatic duct issues.
- Post-ERCP Pancreatitis (PEP): Most common complication (~3-5% incidence).
- PEP Risk Factors: Young female, prior PEP, difficult cannulation, pancreatic sphincterotomy, SOD.
- PEP Prophylaxis: Rectal NSAIDs (indomethacin/diclofenac) are crucial.
- Other Major Complications: Bleeding (post-sphincterotomy), perforation (duodenal/ampullary), cholangitis.
- Technique: Guidewire cannulation preferred to reduce PEP.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

