Recon Principles & Ladder - Building Blocks
- Goals & Principles:
- Restore form & function.
- Replace "like with like" (e.g., mucosa for mucosa).
- Minimize donor site morbidity.
- Simple to complex approach.
- Reconstructive Ladder: Guides choice of technique. Ascend if simpler options are inadequate.
- Healing by secondary intention
- Direct/Primary closure
- Skin grafts (Split/Full Thickness)
- Local flaps (e.g., rotation, transposition)
- Regional flaps (e.g., PMMC, Deltopectoral)
- Free tissue transfer (microvascular anastomosis)
⭐ The choice of reconstructive technique is guided by the "reconstructive ladder," starting with the simplest effective method for the defect presented.
Skin Grafts & Local Flaps - Covering Ground
-
Skin Grafts: Transfer of epidermis & variable dermis; rely on recipient bed vascularity.
- Split-Thickness Skin Graft (STSG): Epidermis & part of dermis. Higher take, can contract. Donor site heals by re-epithelialization.
- Full-Thickness Skin Graft (FTSG): Epidermis & entire dermis. Better cosmesis, less contraction. Donor site needs primary closure or grafting.
- Meshing: Expands STSG, allows drainage.
- Indications: Superficial defects, burns, lining cavities.
-
Local Flaps: Tissue moved from adjacent area with intact blood supply.
- Types: Advancement, rotation, transposition, interpolation.
- Examples: Rhomboid flap, Z-plasty, nasolabial flap.
- Advantages: Good color/texture match, robust vascularity.
⭐ McGregor (Z-plasty) Flap: Angles of 60° theoretically lengthen the scar by 75%. Used for scar revision and contracture release.
📌 Mnemonic for flap survival: Plan, Perfusion, no Pressure, no Pull (tension).
Pedicled Regional Flaps - Workhorse Wonders
- Maintain own blood supply; rotated/transposed from nearby/distant areas.
- Pectoralis Major Myocutaneous (PMMC) Flap:
- Artery: Thoracoacromial (pectoral branch).
- Uses: Oral cavity, oropharynx, hypopharynx, neck.
- Reliable, versatile; can be bulky.
- Deltopectoral (DP) Flap:
- Artery: Internal mammary perforators.
- Uses: Pharyngoesophageal, neck resurfacing. Thinner.
- Latissimus Dorsi (LD) Flap:
- Artery: Thoracodorsal.
- Uses: Large defects (scalp, skull base).
- Trapezius Flap: (Upper, Lateral, Lower based on pedicle)
- Arteries: Occipital, transverse cervical, dorsal scapular.
- Uses: Posterior scalp, lateral face, neck.
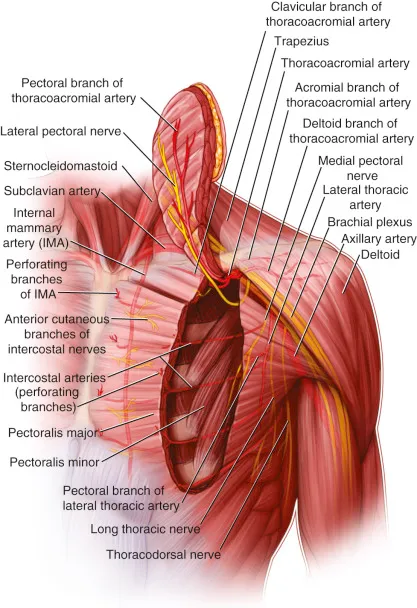
⭐ The PMMC flap is a workhorse for intraoral reconstruction due to its robust thoracoacromial artery pedicle and versatility.
Microvascular Free Flaps - Advanced Arsenal
- Tissue (skin, muscle, bone, or composite) transferred with its own artery & vein; anastomosed to recipient site vessels.
- Indications: Large, complex defects; composite tissue requirements (e.g., bone and soft tissue).
- Advantages: Superior vascularity, versatility, single-stage reconstruction, allows like-for-like tissue replacement.
- Key Flaps & Pedicles:
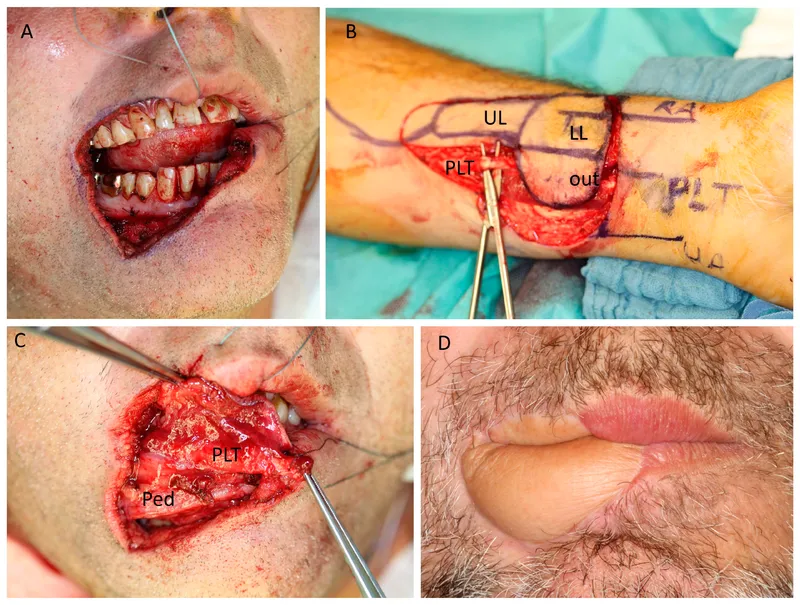
- Radial Forearm Free Flap (RFFF): Radial a. (Thin, pliable; excellent for oral lining).
- Anterolateral Thigh (ALT) Flap: Descending branch of Lat. circumflex femoral a. (Versatile; skin/fascia/muscle).
- Fibula Free Flap (FFF): Peroneal a. (Osseous/osteocutaneous; gold standard for mandibular reconstruction).
- Monitoring: Crucial. Clinical (color, temperature, capillary refill, turgor, bleeding on pinprick), handheld Doppler. Flap checks q1h for first 24h, then progressively less frequent.
- Complications: Thrombosis (venous > arterial), hematoma, infection, partial/total flap loss.
⭐ Venous thrombosis is the most common cause of free flap failure, typically occurring within the first 48-72 hours post-operatively. Early detection and intervention are key to salvage.
High‑Yield Points - ⚡ Biggest Takeaways
- PMMC flap: Workhorse for intraoral defects, pedicled on thoracoacromial artery.
- Radial Forearm Free Flap (RFFF): Thin, pliable for tongue/FOM reconstruction, pedicled on radial artery.
- Anterolateral Thigh (ALT) flap: Versatile for large soft tissue defects, pedicled on descending branch of LCFA.
- Fibula free flap: Gold standard for mandibular reconstruction, pedicled on peroneal artery.
- Latissimus Dorsi flap: For extensive defects, pedicled on thoracodorsal artery.
- Local flaps (e.g., nasolabial, forehead): Key for smaller facial defects reconstruction.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

