Parathyroid Essentials - Calcium's Captains

- Typically 4 small glands, located posterior to the thyroid gland.
- Histology: Chief cells (synthesize & secrete PTH) and Oxyphil cells (function less clear, appear around puberty).
- Parathyroid Hormone (PTH): 84-amino acid peptide; primary regulator of calcium & phosphate balance.
- Net effect of PTH: ↑ serum $Ca^{2+}$, ↓ serum $PO_4^{3-}$.
- Key target organs:
- Bone: ↑ osteoclastic activity, promoting $Ca^{2+}$ and $PO_4^{3-}$ release.
- Kidney: ↑ $Ca^{2+}$ reabsorption (DCT), ↓ $PO_4^{3-}$ reabsorption (PCT), ↑ 1α-hydroxylase activity (converts 25-hydroxyvitamin D to active 1,25-dihydroxyvitamin D).
- Intestine (indirect): Active Vitamin D enhances $Ca^{2+}$ and $PO_4^{3-}$ absorption.
⭐ Hypomagnesemia can impair PTH secretion and cause end-organ resistance to PTH, leading to hypocalcemia despite normal or even elevated PTH levels (functional hypoparathyroidism).
Hyperparathyroidism - HyperPTH Hijinks
-
Types & Etiology:
- Primary (PHPT): Most common. ↑PTH, ↑Ca.
- Parathyroid Adenoma (~80-85%), Hyperplasia, Carcinoma.
- Secondary: ↑PTH, normal/↓Ca.
- Chronic Kidney Disease (CKD), Vitamin D deficiency.
- Tertiary: Autonomous PTH secretion after prolonged secondary. ↑PTH, ↑Ca. Often post-renal transplant.
- Primary (PHPT): Most common. ↑PTH, ↑Ca.
-
Clinical Features: 📌 "Bones, stones, groans, moans."
- Bones: Osteitis fibrosa cystica (brown tumors), bone pain, fractures, subperiosteal resorption (phalanges).
- Stones: Recurrent nephrolithiasis, nephrocalcinosis.
- Groans: Constipation, PUD, pancreatitis, nausea.
- Moans: Fatigue, depression, confusion, weakness.
-
Investigations:
- Labs: ↑ Serum Ca, ↑ PTH (or inappropriately normal for ↑Ca), ↓ Serum PO₄ (in PHPT), ↑ ALP, ↑ 24hr Urine Ca.
- Localization (for surgery in PHPT): Sestamibi scan, Ultrasound neck, 4D CT.
-
Diagnostic Algorithm for Hypercalcemia:
- Management:
- Primary: Parathyroidectomy (if symptomatic or meets criteria). Medical: Cinacalcet, Bisphosphonates.
- Secondary: Treat underlying cause (e.g., Vit D, phosphate binders).
- Tertiary: Parathyroidectomy.
⭐ Familial Hypocalciuric Hypercalcemia (FHH) is an important differential for PHPT, characterized by ↑Ca, ↑PTH, but ↓ urine calcium excretion (Urine Calcium/Creatinine Clearance Ratio < 0.01). It's usually benign and managed conservatively_
Hypoparathyroidism - HypoPTH Havoc
- Definition: Deficient parathyroid hormone (PTH) leading to hypocalcemia (↓ $Ca^{2+}$) & hyperphosphatemia (↑ $PO_4^{3-}$).
- Etiology:
- Post-surgical (most common): Thyroid/parathyroid surgery.
- Autoimmune (APS-1).
- Congenital: DiGeorge syndrome (22q11.2 deletion).
- Radiation, severe hypomagnesemia.
- Clinical Features (due to ↓ $Ca^{2+}$): 📌 CATS go numb:
- Convulsions, seizures.
- Arrhythmias (prolonged QT interval).
- Tetany (neuromuscular irritability):
- Chvostek's sign: Facial nerve tap → facial twitch.
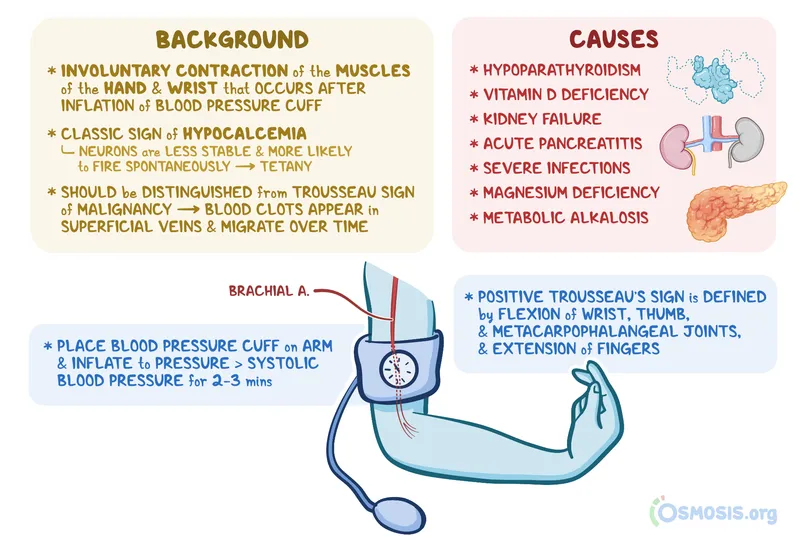
- Trousseau's sign: Cuff inflation → carpal spasm.
- Spasms (laryngospasm), paresthesias (circumoral, digital).
- Chronic: Cataracts, basal ganglia calcification.
- Investigations:
- ↓ Serum $Ca^{2+}$ (total & ionized), ↑ Serum $PO_4^{3-}$, ↓ Serum PTH.
- ECG: Prolonged QT interval.
- Management:
- Acute (symptomatic): IV Calcium gluconate.
- Chronic: Oral calcium, Vitamin D (calcitriol).
⭐ Pseudohypoparathyroidism (Albright's hereditary osteodystrophy) shows ↓ $Ca^{2+}$, ↑ $PO_4^{3-}$, but with ↑PTH (end-organ resistance), plus short 4th/5th metacarpals.
Surgical Aspects & MEN - Glandular Targets
- Indications: Symptomatic PHPT; Asymptomatic if: Age <50y, Ca >1mg/dL high, T-score < -2.5, CrCl <60 mL/min.
- Procedures: MIP (localized adenoma); BNE (MGD, failed localization).
- ioPTH: >50% drop, 10min post-excision (Miami criterion).
- MEN & Parathyroid:
- MEN 1 (📌3Ps): Parathyroid (hyperplasia 90%), Pancreas, Pituitary.
- MEN 2A: Parathyroid (adenoma/hyperplasia 20-30%), MTC, Pheo.
⭐ MEN 1: Parathyroid involvement is earliest & most common. oka
High‑Yield Points - ⚡ Biggest Takeaways
- Primary Hyperparathyroidism (PHPT): Caused mainly by parathyroid adenoma. Symptoms: "bones, stones, groans, moans".
- PHPT labs: ↑ Serum Calcium, ↑ PTH, ↓ Serum Phosphate.
- Secondary Hyperparathyroidism: Often due to CKD or Vitamin D deficiency.
- Hypoparathyroidism: Typically post-surgical; causes hypocalcemia (Chvostek's, Trousseau's signs).
- MEN 1 and MEN 2A syndromes frequently involve parathyroid tumors.
- Sestamibi scan: Gold standard for localizing parathyroid adenomas.
- Hungry Bone Syndrome: Severe post-parathyroidectomy hypocalcemia.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

