Neck Dissection Basics - Unraveling the Layers
Neck dissection (ND) is a surgical procedure to remove cervical lymph nodes, primarily for managing metastatic spread from head and neck cancers. Its goal is oncologic control.
- Types of Neck Dissection:
- Radical Neck Dissection (RND):
- Removes levels I-V, Sternocleidomastoid muscle (SCM), Internal Jugular Vein (IJV), Spinal Accessory Nerve (SAN).
- Modified Radical Neck Dissection (MRND):
- RND principles with preservation of ≥1 non-lymphatic structures (SAN, IJV, SCM).
- Type I: Preserves SAN.
- Type II: Preserves SAN, SCM.
- Type III (Functional ND): Preserves SAN, SCM, IJV.
- Selective Neck Dissection (SND):
- Removes specific nodal groups at risk, preserving all major non-lymphatic structures.
- E.g., Supraomohyoid ND (Levels I-III).
- Radical Neck Dissection (RND):
⭐ George Crile Sr. performed the first RND in 1906, standardizing the procedure for head and neck cancer treatment.
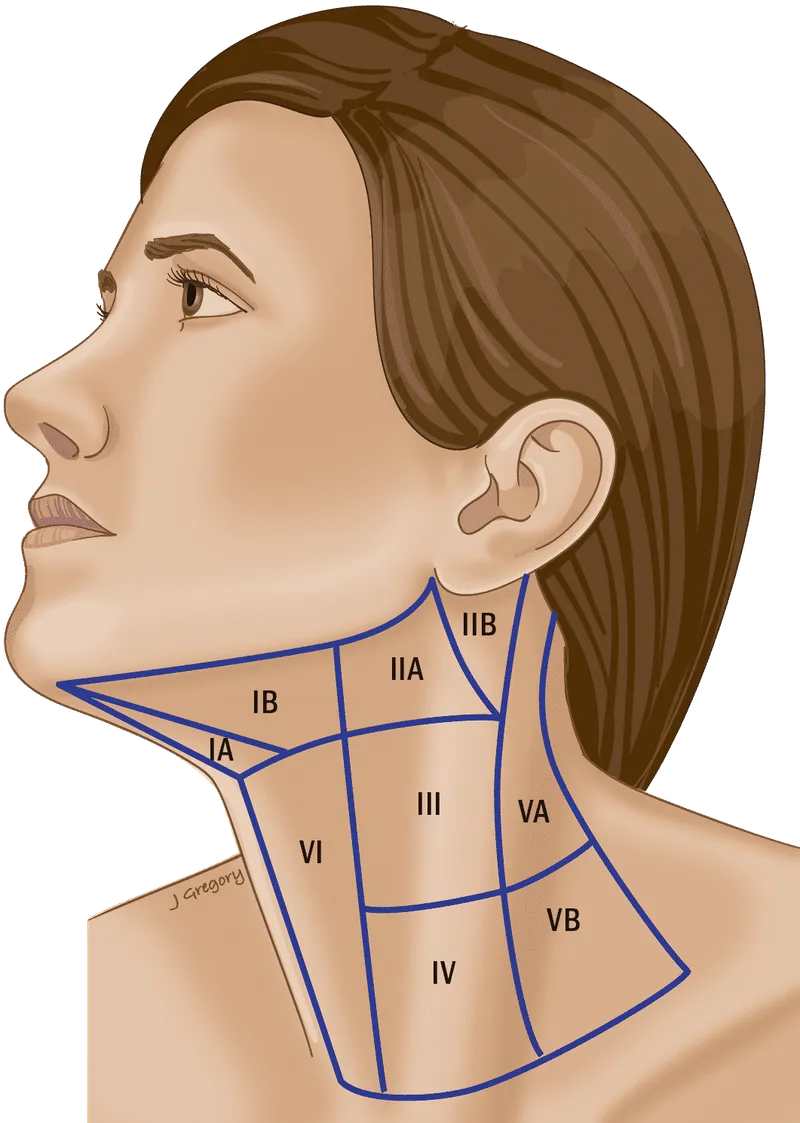
Nodal Levels & Anatomy - Landmarks & Landmines
- Level I (Submental IA, Submandibular IB):
- IA: Ant. digastric bellies, hyoid. IB: Post. digastric, mandible.
- ⚠️ Marginal mandibular n. (lip droop).
- Level II (Upper Jugular IIA/IIB): Skull base to hyoid.
- SAN divides IIA (ant.) & IIB (post.).
- ⚠️ SAN, IJV, Hypoglossal n. (deep).
- Level III (Middle Jugular): Hyoid to cricoid.
- ⚠️ Vagus n., IJV.
- Level IV (Lower Jugular): Cricoid to clavicle.
- ⚠️ Thoracic duct (L), Phrenic n. (on ant. scalene), Brachial plexus.
- Level V (Posterior Triangle VA/VB): SCM, Trapezius, Clavicle.
- SAN divides VA (sup.) & VB (inf.). 📌 SAN vulnerable at Erb's point.
- ⚠️ SAN, Brachial plexus.
- Level VI (Anterior/Central): Hyoid to suprasternal notch, b/w carotids.
- Nodes: Pre/paratracheal, Precricoid (Delphian).
- ⚠️ Recurrent Laryngeal Nerves.
- Level VII (Superior Mediastinal): Suprasternal notch to innominate a.
⭐ The Spinal Accessory Nerve (CN XI) is a key landmark, often at risk; injury causes shoulder droop/impaired abduction. Divides Level II (A/B) & V (A/B).

Indications & Choice - The Dissection Decision
- Therapeutic Neck Dissection (TND):
- Indicated for clinically palpable nodes (cN+).
- Goal: Remove existing metastases, achieve regional control.
- Elective Neck Dissection (END):
- Indicated for clinically negative neck (cN0) with high risk (>15-20%) of occult metastases.
- Risk factors: Primary tumor site (e.g., oral cavity, oropharynx), T-stage (esp. T2 or higher), depth of invasion (DOI >3-4 mm for oral SCC), perineural invasion (PNI), lymphovascular invasion (LVI).
- Choice of Dissection Type:
- cN0 (END): Selective Neck Dissection (SND) tailored to primary site.
- Oral Cavity: SND (Levels I-III).
- Oropharynx, Hypopharynx, Larynx: SND (Levels II-IV).
- cN+ (TND):
- N1: Comprehensive SND or Modified Radical Neck Dissection (MRND).
- N2-N3 / Extranodal Extension (ENE): MRND. Radical Neck Dissection (RND) is rarely performed.
- cN0 (END): Selective Neck Dissection (SND) tailored to primary site.
⭐ For cN0 oral cavity squamous cell carcinoma, END (typically SND I-III) is indicated if DOI >4 mm or T-stage ≥T2, as risk of occult nodal metastasis often exceeds 20%.
Complications & Care - Navigating the Risks
- Intraoperative Risks:
- Nerve Injury: Spinal Accessory (SAN) (most common in posterior triangle), Marginal Mandibular, Hypoglossal.
- Vascular Injury: Carotid Artery, Internal Jugular Vein.
- Chyle Leak (Left > Right): Thoracic duct injury.
- Postoperative Concerns & Management:
- Hemorrhage, Hematoma, Seroma.
- Wound Infection.
- Nerve Palsies:
- SAN: 📌 Shoulder drop, winging scapula. Early physiotherapy vital.
- Marginal Mandibular: Lower lip weakness. Often transient.
- Chyle Fistula (Persistent):
- Initial: NPO, TPN, low-fat/Medium-Chain Triglyceride (MCT) diet, pressure dressing.
⭐ If chyle leak persists (>500-600 mL/day or >1-2 weeks despite conservative measures), escalate to octreotide or surgical intervention (e.g., duct ligation).
High‑Yield Points - ⚡ Biggest Takeaways
- Radical Neck Dissection (RND): Removes Sternocleidomastoid (SCM), Internal Jugular Vein (IJV), Spinal Accessory Nerve (SAN), and lymph nodes Levels I-V.
- Modified RND (MRND): Preserves one or more key structures, most commonly the SAN, followed by IJV and SCM.
- Selective Neck Dissection (SND): Removes specific at-risk nodal groups based on primary tumor site.
- Spinal Accessory Nerve (SAN) injury causes shoulder droop and impaired arm abduction; its preservation is crucial.
- Common complications include chyle leak (especially left-sided, thoracic duct injury) and nerve injuries (SAN, marginal mandibular).
- Levels I-V are standard dissection fields; Level VI (anterior compartment) is addressed for thyroid/laryngeal cancers.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

