Laryngeal Anatomy & Physiology - Voice Box Virtuoso

- Cartilages:
- Unpaired: Thyroid, Cricoid, Epiglottis.
- Paired: Arytenoid, Corniculate, Cuneiform.
- Muscles:
- Intrinsic: Control sound production (phonation); fine movements of vocal cords.
- Extrinsic: Support & move larynx as a whole during swallowing.
- Nerve Supply:
- Superior Laryngeal Nerve (SLN):
- External branch: Cricothyroid (tensor).
- Internal branch: Sensory above vocal cords.
- Recurrent Laryngeal Nerve (RLN): All other intrinsic muscles; sensory below vocal cords.
- 📌 SLN Sensory above, RLN Remaining muscles & Reaches below.
- Superior Laryngeal Nerve (SLN):
⭐ All intrinsic muscles of the larynx are supplied by the recurrent laryngeal nerve (RLN), except the cricothyroid muscle, which is supplied by the external branch of the superior laryngeal nerve (SLN).
Congenital & Inflammatory Disorders - Airway Alarms
-
Laryngomalacia: Most common congenital stridor cause in infants; omega-shaped epiglottis. Inspiratory stridor, improves prone.
⭐ Laryngomalacia is the most common congenital laryngeal anomaly and the most frequent cause of stridor in infants.
-
Acute Laryngitis:
- Etiology: Viral.
- Tx: Voice rest, hydration.
-
Chronic Laryngitis:
- Causes: Smoking, Laryngopharyngeal Reflux (LPR), voice abuse.
-
Croup vs. Acute Epiglottitis:
Feature Croup (LTB) Acute Epiglottitis Etiology Parainfluenza virus Haemophilus influenzae type b (Hib) Onset Gradual Rapid Cough Barking Muffled/Absent Drooling Absent Present Fever Low-grade High Posture Any Tripod X-ray Sign Steeple sign Thumb sign 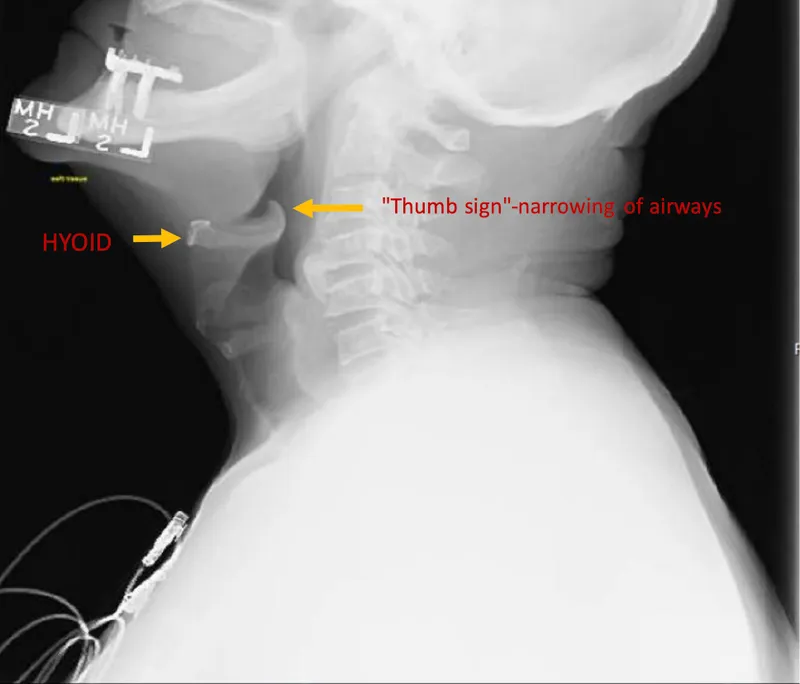
📌 Epiglottitis (AIR RAID): Airway inflammation, Increased pulse, Restlessness, Retractions, Anxiety, Inspiratory stridor, Drooling.
Benign Vocal Fold Lesions - Hoarseness Hurdles
Common causes of hoarseness, often linked to voice use or specific exposures.
- Vocal Nodules (Singer's/Screamer's Nodes)
- Bilateral, symmetric lesions.
- Junction of anterior 1/3 & posterior 2/3 of vocal folds.
- Etiology: Voice abuse/misuse.
- Vocal Polyps
- Usually unilateral, often pedunculated or sessile.
- Can be hemorrhagic.
- Etiology: Voice abuse, single traumatic event.
- Vocal Cord Cysts
- Unilateral, submucosal, mucus-retention or epidermoid.
- Etiology: Blocked mucus gland, congenital.
| Feature | Vocal Nodules | Vocal Polyps | Vocal Cord Cysts |
|---|---|---|---|
| Laterality | Bilateral | Unilateral | Unilateral |
| Appearance | Symmetric, whitish | Often reddish | Submucosal, firm |
| Main Cause | Chronic voice abuse | Acute/chronic | Gland blockage |
* Diffuse, gelatinous swelling of superficial lamina propria (Reinke's space).
* Strongly associated with smoking; low-pitched, husky voice.
- Laryngeal Papillomatosis
- Caused by HPV types 6 and 11.
- Juvenile (aggressive, multiple recurrences) vs. Adult (often single lesion).
⭐ Vocal nodules typically occur bilaterally at the midpoint of the membranous vocal folds (junction of anterior one-third and posterior two-thirds).
Vocal Cord Paralysis & Laryngeal Cancer - Larynx Under Siege
-
Vocal Cord Paralysis (VCP)
-
Causes:
- Unilateral: Iatrogenic (thyroid surgery - Recurrent Laryngeal Nerve injury), malignancy, idiopathic.
- Bilateral: Iatrogenic (thyroid surgery), neurological.
-
📌 Semon's Law: In RLN palsy, abductors paralyze before adductors.
-
Vocal Cord Positions & Effects:
Position Cord Voice Airway Median Midline Good Poor (stridor) Paramedian 1-2mm lateral Breathy Fair Cadaveric 3.5-4mm lateral Aphonic Good

-
-
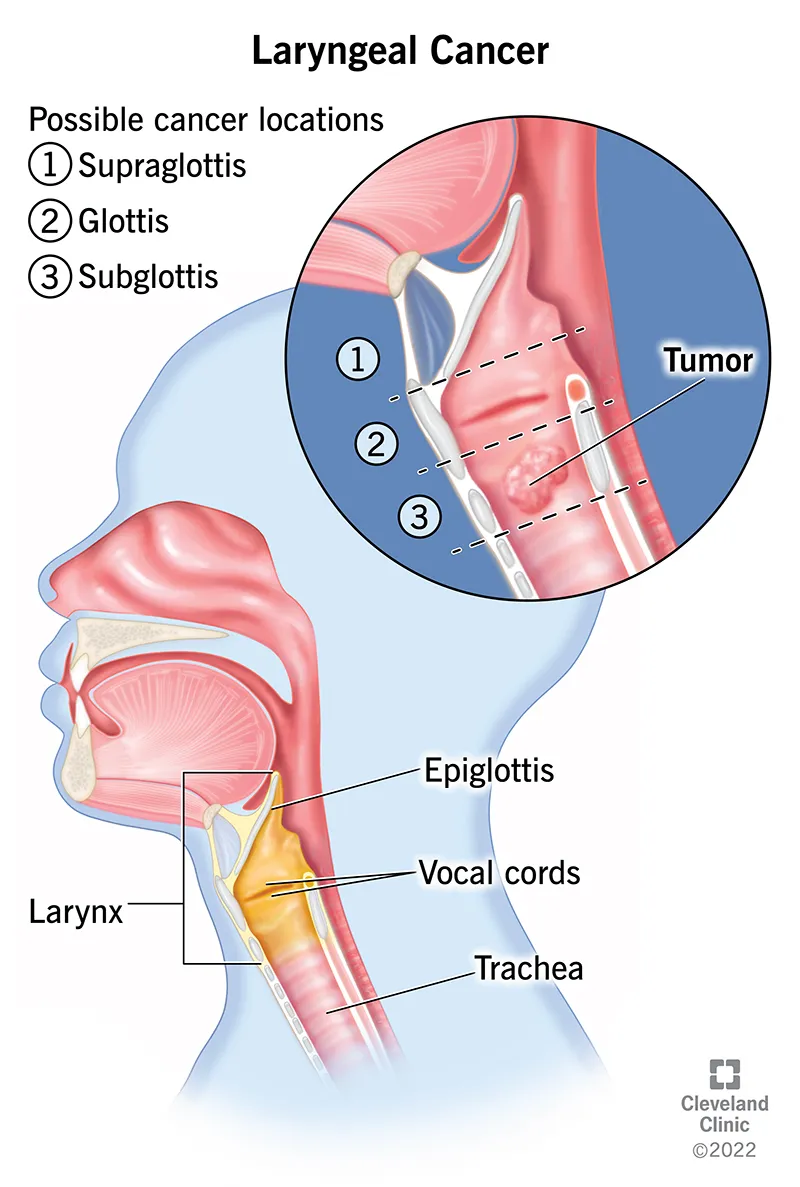
Laryngeal Cancer
- Most common: Squamous Cell Carcinoma (SCC) >90%.
- Risk Factors: Smoking, alcohol.
- Sites & Prognosis:
- Glottic (60-65%): Best prognosis. Hoarseness early.
- Supraglottic (30-35%): Rich lymphatics, ↑mets. Dysphagia, odynophagia.
- Subglottic (<5%): Poorest. Late symptoms, stridor.
- Simplified Glottic T-staging:
- T1: Normal mobility (T1a one cord, T1b both).
- T2: Extends supra/subglottis OR impaired mobility.
- T3: Cord fixation.
- T4: Invades cartilage/beyond larynx.
- Treatment: Radiotherapy (RT), Surgery (e.g., laryngectomy), Chemotherapy.
-
Flowchart: Management of T1a Glottic Cancer
⭐ The most common cause of bilateral abductor vocal cord paralysis is iatrogenic injury during thyroid surgery.
High‑Yield Points - ⚡ Biggest Takeaways
- Hoarseness: The cardinal symptom of laryngeal disease.
- Laryngomalacia: Most common congenital anomaly, causing infantile inspiratory stridor.
- Acute epiglottitis: Medical emergency; thumb sign on X-ray; H. influenzae b.
- Vocal cord nodules: Bilateral, from chronic voice abuse; voice therapy is key.
- Laryngeal SCCa: Most common malignancy; smoking & alcohol are major risk factors; persistent hoarseness is a red flag.
- Vocal cord palsy: Unilateral causes breathy voice; Bilateral presents risk of airway compromise.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

