Cancer Basics & Staging - Know Thy Enemy
- Cancer: Uncontrolled cell growth with local invasion & potential for metastasis.
- TNM System (AJCC/UICC): Standard for describing cancer's anatomical extent.
- T (Primary Tumor): Describes size/local extent (e.g., T0, Tis, T1-T4).
- N (Regional Lymph Nodes): Indicates involvement (e.g., N0, N1-N3).
- M (Distant Metastasis): Presence/absence of spread (M0/M1).
- Staging Types:
- Clinical (cTNM): Pre-treatment (physical exam, imaging).
- Pathological (pTNM): Post-surgery (histopathology); often more accurate.
- Purpose: Guides treatment, predicts prognosis, standardizes research.
⭐ Pathological staging (pTNM), based on surgical specimen analysis, is generally more accurate for prognosis than clinical staging (cTNM).
Diagnosis & Biopsy - Pinpointing Foe
- Evaluation: History, clinical exam. Imaging (USG, CT, MRI, PET-CT) for staging.
- Biopsy: Gold Standard
- Key: Representative tissue, avoid tumor seeding.
- Types:
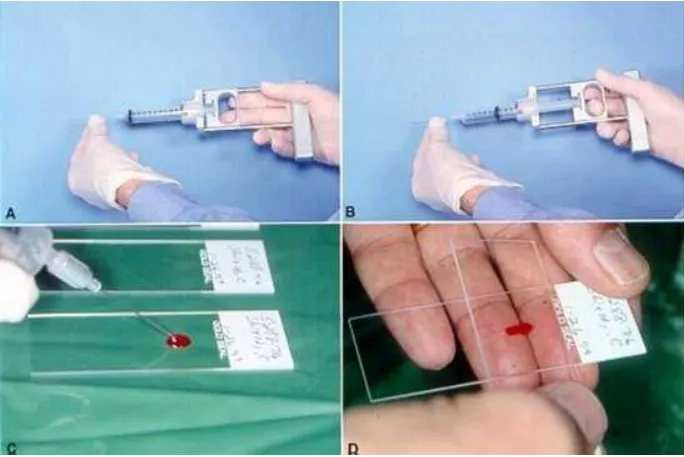
- FNAC: Cytology; palpable lesions (thyroid, LN).
- Core Needle (Tru-Cut): Histology; solid tumors (breast, liver).
- Incisional: Part of tumor removed.
- Excisional: Whole lesion removed (small, accessible).
- Endoscopic: GI, respiratory tract.
- Tumor Markers: Blood tests; aid diagnosis, prognosis, monitoring.
- AFP: HCC, yolk sac tumor.
- β-hCG: Germ cell tumors, choriocarcinoma.
- CEA: Colorectal, GI, breast, lung.
- CA-125: Ovarian. PSA: Prostate.
⭐ For suspected sarcoma, biopsy incision should be planned along lines of definitive surgery to allow en-bloc resection of the biopsy tract.
Surgical Principles & Margins - Scalpel Tactics
- Primary Goal: R0 resection (microscopically negative margins) for curative intent.
- En Bloc Resection: Tumor with normal tissue cuff & regional lymphatics; avoid tumor spillage.
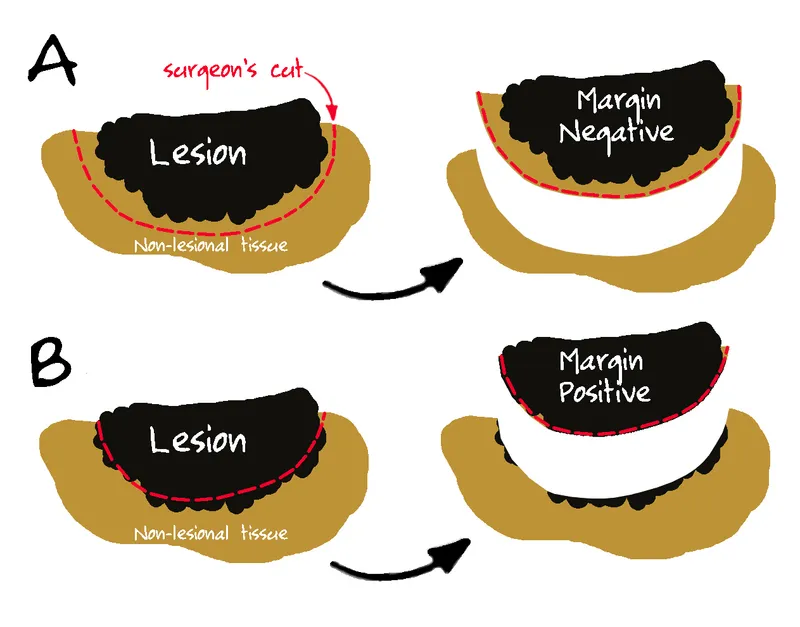
- Margin Status:
- R0: No tumor cells at inked margin.
- R1: Microscopic tumor at margin.
- R2: Macroscopic residual tumor.
- Margin Width: Tumor-specific (e.g., Sarcoma: 1-2 cm; Melanoma: Breslow depth-dependent).
- Techniques: Sharp dissection, meticulous hemostasis, "no-touch" isolation.
- Lymph Nodes: SLNB or regional lymphadenectomy based on tumor type/stage.
⭐ Achieving an R0 resection is the most critical prognostic factor for local control in many solid tumors.
Multimodal Treatment - Cancer's United Front
- Combines surgery, chemotherapy (CTX), radiotherapy (RTX), immunotherapy, & targeted therapy.
- Goal: ↑cure rates, organ preservation, Quality of Life (QoL).
- Neoadjuvant Therapy:
- Given before primary local therapy (e.g., surgery).
- Aims: ↓tumor size, ↑resectability, treat micrometastases early.
- Adjuvant Therapy:
- Given after primary local therapy.
- Aims: Eradicate residual microscopic disease, ↓recurrence risk.
- Concurrent Therapy:
- Two or more therapies given simultaneously (e.g., Chemoradiation - CRT).
- Often synergistic; ↑efficacy but also ↑toxicity.
- Multidisciplinary Team (MDT): Essential for integrated treatment planning & coordination.
⭐ Neoadjuvant chemotherapy (NACT) in locally advanced breast cancer (LABC) can downstage tumors, potentially enabling breast conservation surgery instead of mastectomy. This improves cosmetic outcomes and QoL without compromising survival for suitable patients when part of an MDT approach.
High‑Yield Points - ⚡ Biggest Takeaways
- Biopsy principles are crucial: Needle core biopsy is often preferred for diagnosis. Avoid tumor seeding during procedures.
- TNM staging (AJCC standard) is paramount for prognosis and guiding treatment strategy.
- The primary goal of curative surgery is achieving R0 resection (microscopically negative margins).
- Sentinel Lymph Node Biopsy (SLNB) is vital for staging in clinically node-negative melanoma and breast cancer.
- Multimodal therapy, combining surgery with chemotherapy, radiotherapy, or targeted therapy, often yields optimal outcomes.
- Palliative surgery focuses on symptom relief and improving quality of life, not cure, in advanced cancers.
- Understand oncologic emergencies like SVC obstruction or spinal cord compression for prompt management.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

