Surgical Complications - Setting the Stage
- Definition: Deviation from ideal post-op course.
- Timing:
- Immediate: <24 hrs (e.g., hemorrhage, anesthetic reaction).
- Early: 1-30 days (e.g., SSI, DVT, atelectasis).
- Late: >30 days (e.g., hernia, adhesions, pain).
- Severity Grading: Clavien-Dindo Classification (I-V).
- I: Minor deviation; no specific treatment.
- II: Pharmacological Rx (incl. transfusion, TPN).
- III: Surgical, endoscopic, or radiological intervention.
- IIIa: Intervention w/o GA.
- IIIb: Intervention w/ GA.
- IV: Life-threatening; ICU care.
- IVa: Single organ dysfunction.
- IVb: Multi-organ dysfunction.
- V: Death.
- Suffix 'd': Disability at discharge.
⭐ Clavien-Dindo Grade IIIb requires surgical, endoscopic, or radiological intervention, typically under general anesthesia.
Surgical Complications - Wound Woes
- Hematoma: Collection of blood.
- Risk: Inadequate hemostasis, anticoagulants.
- Mx: Small - observe; Large/expanding - evacuate.
- Seroma: Collection of serous fluid.
- Mx: Aspiration (sterile), pressure dressing; recurrent - sclerosant/drain.
- Surgical Site Infection (SSI): Infection at/near surgical incision within 30 days (or 1 year if implant).
- Types: Superficial, Deep incisional, Organ/space.
- Mx: Antibiotics, drainage, debridement.
⭐ Staphylococcus aureus is the most common pathogen in SSIs.
- Wound Dehiscence: Partial/complete separation of wound layers.
- Risk factors: ↑intra-abdominal pressure, poor nutrition, infection.
- Evisceration: Protrusion of viscera through dehisced wound (surgical emergency!).
- Mx: Sterile saline-soaked gauze, immediate OR.
- Fistula: Abnormal communication between two epithelial surfaces.
- Incisional Hernia: Protrusion of abdominal contents through previous incision site.

Surgical Complications - Systemic Storms
⭐ The "5 W's" (Wind, Water, Wound, Walking, Wonder drugs/What did we do?) is a classic mnemonic for causes of post-operative fever based on timing.
- Post-Op Fever (📌 5 W's):
- Wind (Atelectasis, Pneumonia): POD 1-3.
- Water (UTI): POD 3-5.
- Wound (Infection): POD 5-7.
- Walking (DVT/PE): POD 7+.
- Wonder Drugs (Drug fever): Anytime.
- Key Systemic Issues:
- Respiratory: Atelectasis (commonest early fever), Pneumonia, PE (DVT prophylaxis).
- Cardiovascular: DVT (Wells, Doppler), MI (peri-op stress).
- GI: Ileus (prolonged >3-5 days), Anastomotic leak (fever, ↑HR).
- GU: UTI (CAUTI), AKI (monitor UO).
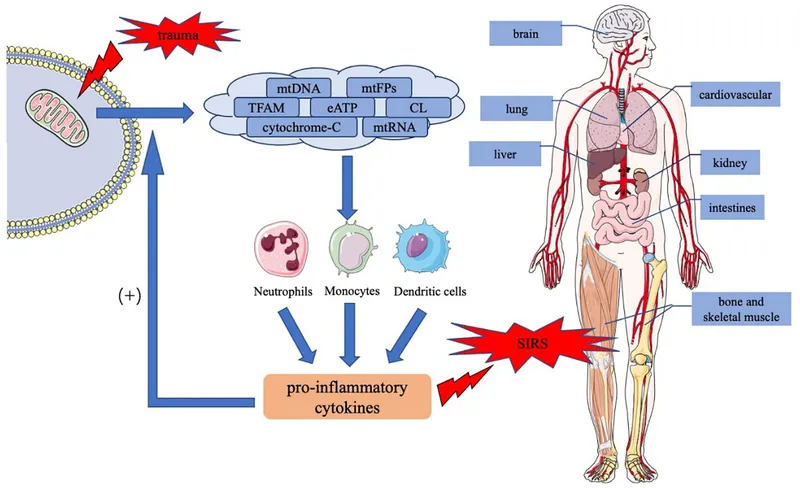
- SIRS/Sepsis:
- SIRS: ≥2 (T >38°C/<36°C, HR >90, RR >20 or $P_aCO_2 < \textbf{32}$ mmHg, WBC >12k/<4k/>10% bands).
- Sepsis: SIRS + infection → MODS.
Surgical Complications - Critical Crises
- Shock: Acute circulatory failure.
- Hypovolemic: ↓Volume (hemorrhage). Treat: Fluids, blood, stop loss.
- Septic: Infection + dysregulated host response. Treat: Fluids, antibiotics, vasopressors.
- Cardiogenic: Pump failure (e.g., MI). Treat: Inotropes, address cause.
- Neurogenic: Sympathetic tone loss (spinal injury). Treat: Vasopressors, atropine.
- SIRS, Sepsis, Septic Shock:
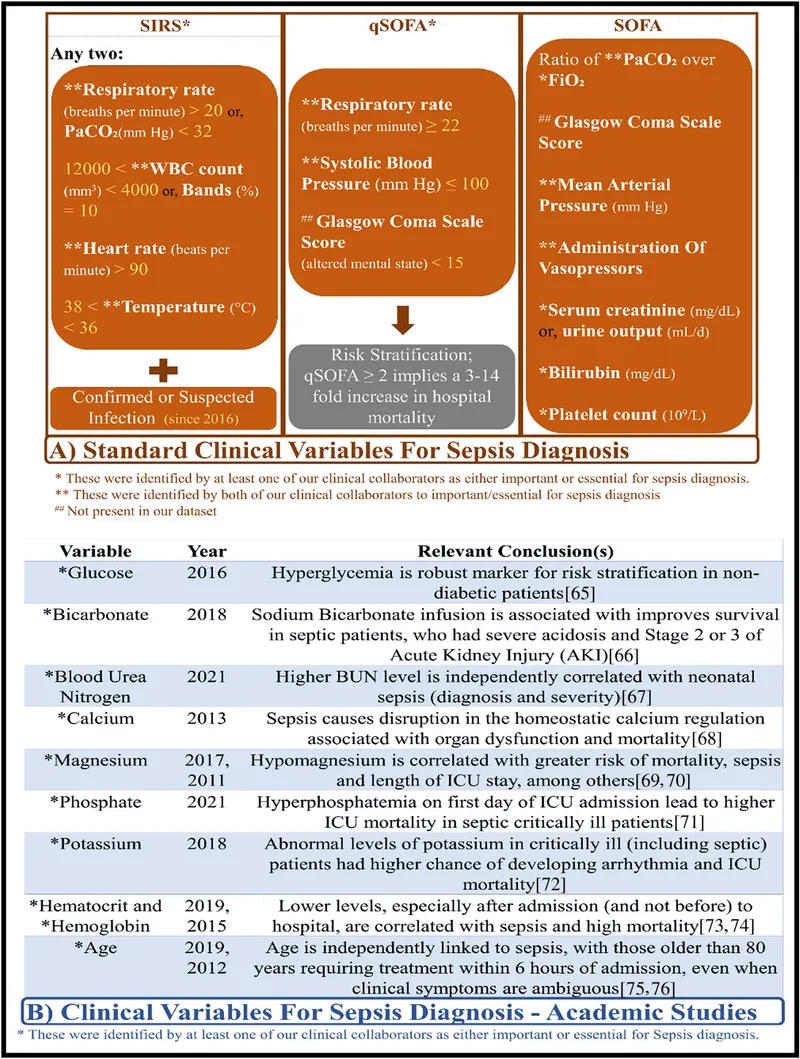
- SIRS: ≥2: Temp >38°C/<36°C; HR >90/min; RR >20/min or PaCO₂ <32mmHg; WBC >12,000/mm³/<4,000/mm³ or >10% bands.
- Sepsis: SIRS + suspected/confirmed infection.
- Septic Shock: Sepsis + hypotension despite fluids, requiring vasopressors & lactate >2 mmol/L.
⭐ Key components of qSOFA score (≥2 points suggests higher risk of poor outcome with sepsis): Respiratory Rate ≥22/min, Altered Mentation (GCS <15), Systolic Blood Pressure ≤100 mmHg.
High‑Yield Points - ⚡ Biggest Takeaways
- Staphylococcus aureus is the most common cause of Surgical Site Infections (SSI).
- Post-op fever causes (5 W's): Atelectasis (Day 1-2), UTI (Day 3-5), SSI (Day 5-7), DVT/PE (Day 7+), Drug fever.
- Wound dehiscence is fascial separation; evisceration involves visceral protrusion.
- DVT prophylaxis is critical in major surgeries to prevent pulmonary embolism.
- Anastomotic leaks in GI surgery present with sepsis and require prompt management.
- Malignant hyperthermia, triggered by anesthetics, is treated with dantrolene.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more


