Hemostasis Essentials - Clotting Crew Call
- Hemostasis: Physiological process halting blood loss post-injury.
- Key Stages:
- Vascular Spasm: Initial vasoconstriction reduces blood flow.
- Primary Hemostasis (Platelet Plug Formation):
- Adhesion: Platelets bind exposed collagen via vWF-GpIb.
- Activation: Shape change; release of ADP, TXA2 (potent vasoconstrictor & platelet activator).
- Aggregation: GpIIb/IIIa binds fibrinogen, linking platelets.
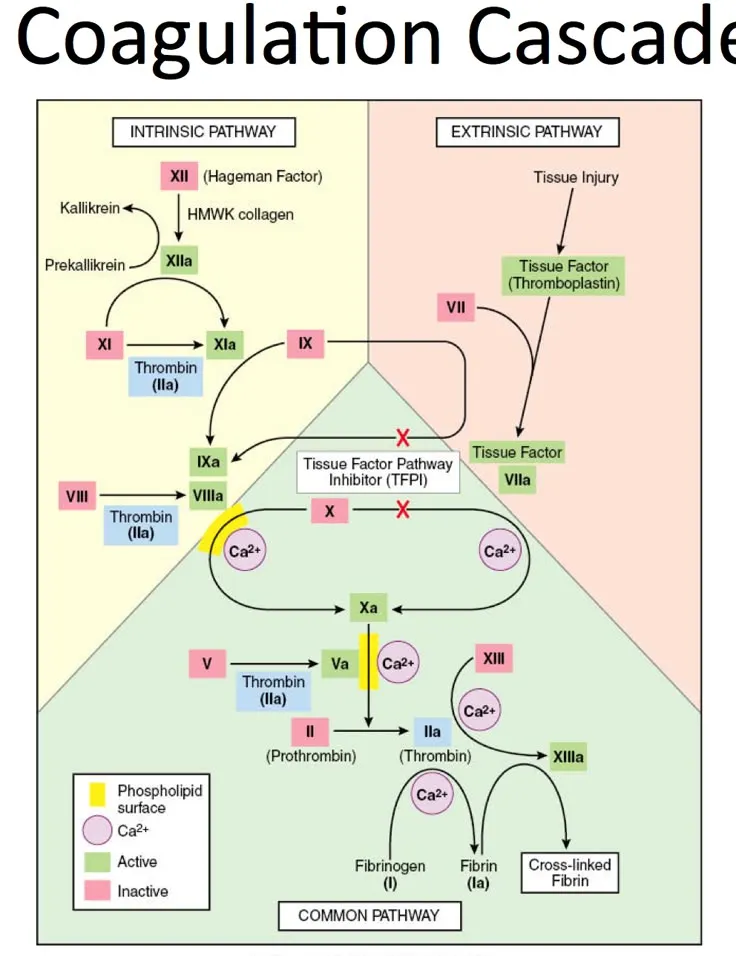
- Secondary Hemostasis (Coagulation Cascade): Enzymatic cascade forming fibrin clot.
- Fibrinolysis: Clot dissolution by plasmin.
- Simplified Coagulation Pathways:
⭐ Vitamin K is crucial for factors II, VII, IX, X (📌 Mnemonic: 1972) & anticoagulant proteins C, S.
Bleeding & Clotting Chaos - When Systems Fail
Disorders of hemostasis: excessive bleeding or thrombosis. Key conditions:
| Disorder | Defect | PT | aPTT | BT | Platelets | Clinical Features / Notes |
|---|---|---|---|---|---|---|
| Hemophilia A | FVIII def. | N | ↑ | N | N | Hemarthrosis, deep muscle hematomas; X-linked recessive |
| Hemophilia B | FIX def. | N | ↑ | N | N | Like Hemophilia A; X-linked recessive |
| vWD | vWF def./abnormality | N | N/↑ | ↑ | N | Mucocutaneous bleed (epistaxis); AD; 📌 Most common inherited |
| ITP | Anti-platelet Abs (GPIIb/IIIa) | N | N | ↑ | ↓↓↓ | Isolated ↓platelets; petechiae, purpura; often post-viral |
| TTP | ADAMTS13 def./autoAb | N | N | ↑ | ↓↓↓ | FAT RN: Fever, MAHA, ↓Platelets, Renal, Neuro sx |
| DIC | Consumptive coagulopathy | ↑ | ↑ | ↑ | ↓ | Bleeding + Thrombosis; ↑D-dimer, ↓Fibrinogen; schistocytes |
- Thrombophilias (Hypercoagulable States):
- Factor V Leiden: Most common inherited (APC resistance).
- Antiphospholipid Syndrome (APS): Acquired; arterial/venous thrombosis, recurrent fetal loss.
- Protein C/S, Antithrombin III deficiencies.
⭐ FFP replaces all clotting factors; Cryoprecipitate: rich in Fibrinogen, FVIII, vWF, FXIII.
Hemostasis Meds & Moves - Drug & Scalpel Fixes
Pharmacological:
- Anticoagulants:
Drug MOA Monitor Reversal UFH Potentiates ATIII aPTT Protamine (1mg/100U) Warfarin Vit K antag PT/INR (2-3) Vit K, PCC, FFP DOACs Direct Th/Xa inhib (Specific) Idaru (Dabi), Andex (Xa inh) - Procoagulants:
- Tranexamic Acid (TXA): Antifibrinolytic (1g IV).
- DDAVP: ↑vWF, FVIII.
- Blood: FFP, Cryo, Plts.
⭐ FFP replaces all clotting factors; dose 10-15 mL/kg. Cryoprecipitate: Fibrinogen, FVIII, FXIII, vWF.
Surgical & Topical:
- Mechanical: Pressure, ligature, tourniquet.
- Thermal: Cautery, Argon Plasma Coagulation (APC).
- Topical: Gelfoam, Surgicel, Thrombin. 📌 Surgicel Slowly resorbed.
Anticoagulation Reversal Algorithm:
Blood Transfusion Basics - Life‑Saving Liquids
-
Indications: Symptomatic anemia, Hb < 7 g/dL (or < 8 g/dL if cardiac hx), active bleeding, coagulopathy.
-
Blood Products Table:
Product Content Key Indication Volume/Effect (Typical) Storage Temp PRBC RBCs ↑O₂ capacity ~300mL; 1U ↑Hb 1g/dL 2-6°C Platelets Platelets Bleeding, Plt < 10-20k ~50mL(RDP); 1U RDP ↑Plt 5-10k 20-24°C (agitate) FFP All factors Coagulopathy (INR > 1.5) ~250mL; 10-15mL/kg ≤ -18°C Cryoprecipitate Fibrinogen, FVIII, vWF Fibrinogen < 100mg/dL ~15mL/U; 10U ↑Fib 50-70mg/dL ≤ -18°C -
Massive Transfusion Protocol (MTP): >10 units PRBC/24h. Ratio 1:1:1 (PRBC:FFP:Platelets).
-
Acute Transfusion Reaction Management:
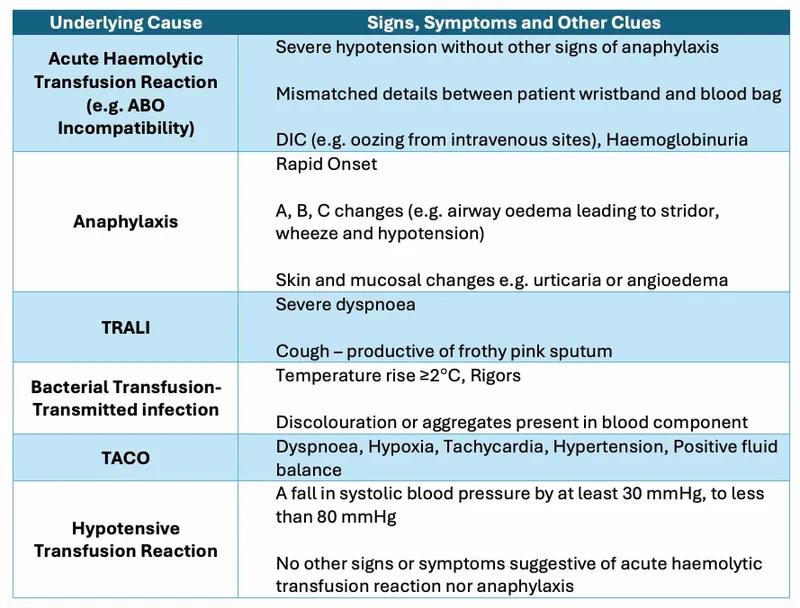
⭐ ABO incompatibility (clerical error) is the leading cause of fatal transfusion reactions.
High‑Yield Points - ⚡ Biggest Takeaways
- Primary hemostasis: Platelet plug formation (adhesion, activation, aggregation).
- Secondary hemostasis: Coagulation cascade activation leads to a stable fibrin clot.
- Vitamin K dependent factors include II, VII, IX, X, Protein C & S.
- FFP replaces all clotting factors; Cryoprecipitate for fibrinogen, Factor VIII, vWF, Factor XIII.
- Massive transfusion protocol (MTP) aims for 1:1:1 ratio of PRBC:FFP:Platelets.
- Febrile non-hemolytic is the most common transfusion reaction; monitor for TRALI and TACO.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more