Congenital Anomalies - Quirks & Twists
⭐ Meckel's diverticulum, the most common GI congenital anomaly, typically presents with painless rectal bleeding in children due to ectopic gastric mucosa.
- Meckel's Diverticulum: True diverticulum (all gut layers).
- 📌 Rule of 2s: 2% population, 2 feet from ileocecal valve, 2 inches long, 2% symptomatic, 2 common ectopic tissues (gastric, pancreatic).
- Complications: Bleeding (commonest), intussusception (lead point), diverticulitis, volvulus, perforation.
- Malrotation & Volvulus:
- Abnormal midgut rotation; Ladd's bands may cause duodenal obstruction.
- Midgut volvulus: Neonatal bilious emesis. Surgical emergency!
- Intestinal Atresia/Stenosis:
- Duodenal: "Double bubble" sign on X-ray; strong association with Trisomy 21.
- Jejunoileal: Caused by in-utero vascular accidents (e.g., SMA branch occlusion). "Apple peel" or "Christmas tree" deformity.

Inflammatory Conditions - Battles & Bugs
- Crohn's Disease (CD)
- Skip lesions, cobblestone mucosa, string sign (barium)
- Complications: fistulas, strictures, abscesses
- ASCA positive
- EIMs: arthritis, uveitis, erythema nodosum
⭐ Crohn's disease is characterized by transmural inflammation, non-caseating granulomas, and can affect any part of the GIT from mouth to anus, most commonly the terminal ileum.
- Intestinal Tuberculosis (TB)
- Ileocecal commonest; transverse ulcers
- Caseating granulomas
- Complications: strictures, obstruction, perforation

- Typhoid (Enteric) Fever
- Salmonella typhi; Peyer's patch hypertrophy (terminal ileum)
- Longitudinal ulcers
- Complications: perforation, hemorrhage (2nd-3rd week)
- Other Infections
- Yersiniosis: mimics appendicitis, terminal ileitis
- Whipple's Disease: T. whipplei; PAS+ macrophages, malabsorption, steatorrhea
Obstruction & Vascular Issues - Blockades & Bummers
- Small Bowel Obstruction (SBO)
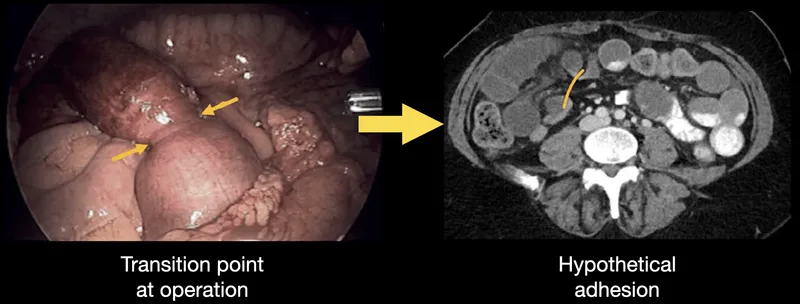
- Etiology: Adhesions (most common), hernias, tumors. 📌 "ABC": Adhesions, Bulges (hernias), Cancer.
- Clinical (4 cardinal signs): Colicky pain, vomiting (bilious→faeculent), distension, obstipation.
- Diagnosis: X-ray (dilated loops >3cm, air-fluid levels). CT confirms, shows cause/complications.
- Management: NPO, IV fluids, NG tube. Surgery for strangulation, closed-loop, or no resolution.
⭐ Adhesions from previous surgery are the leading cause of small bowel obstruction in adults, while hernias are the second most common.
- Acute Mesenteric Ischemia (AMI)
- Types: Arterial (embolus/thrombus), venous, NOMI.
- Classic: Severe pain "out of proportion" to exam. ↑Lactate, metabolic acidosis.
- Diagnosis: CT Angiography (CTA) is key.
- Treatment: Urgent surgery (revascularization/resection of non-viable bowel). High mortality.
Small Bowel Neoplasms & SBS - Tumors & Takeouts
- Neoplasms: Often vague symptoms (pain, bleeding, obstruction).
- Benign: Adenoma, Leiomyoma, Lipoma.
- Malignant: AdenoCa (MC, duod/jej), Carcinoid (ileum), Lymphoma (ileum, celiac assoc.), GIST (c-KIT+).
⭐ Carcinoid tumors are the most common endocrine tumors of the GI tract, often arising in the ileum and appendix; hepatic metastases are required for carcinoid syndrome.
- Carcinoid Syndrome (if liver mets): Flushing, diarrhea, bronchospasm. Dx: ↑ 5-HIAA.
- Short Bowel Syndrome (SBS):
- Malabsorption if < 200 cm SB remaining.
- Etiology: Crohn's, volvulus, ischemia, massive resection.
- Complications: Malnutrition, dehydration, electrolyte imbalance, gallstones, oxalate renal stones.
- Mgmt: Diet (high calorie/protein, low fat), TPN, octreotide.
High‑Yield Points - ⚡ Biggest Takeaways
- Meckel's diverticulum: Rule of 2s, most common congenital GI anomaly, ectopic gastric mucosa.
- Crohn's disease: Transmural inflammation, skip lesions, cobblestoning, non-caseating granulomas.
- Intussusception: Commonest cause of infant intestinal obstruction, currant jelly stool, target sign (USG).
- Small Bowel Obstruction (SBO): Adhesions (post-op) are leading cause in adults; hernias second.
- Carcinoid tumors: Most common in appendix; carcinoid syndrome with liver metastasis (flushing, diarrhea).
- Celiac disease: Gluten sensitivity causing villous atrophy; anti-TTG antibodies positive_._
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

