Stoma Fundamentals - What's the Hole Story?
- Stoma: Artificial opening connecting an internal organ to the body surface.
- Ostomy: Surgical procedure to create a stoma.
- Common Indications: Cancer (colorectal), IBD (Crohn's, UC), trauma, obstruction, fecal diversion.
- Types & Classification:
- Common: Ileostomy, Colostomy. Others: Gastrostomy, Jejunostomy.
- Configuration: End, Loop, Double-barrel.
- Duration: Temporary, Permanent.
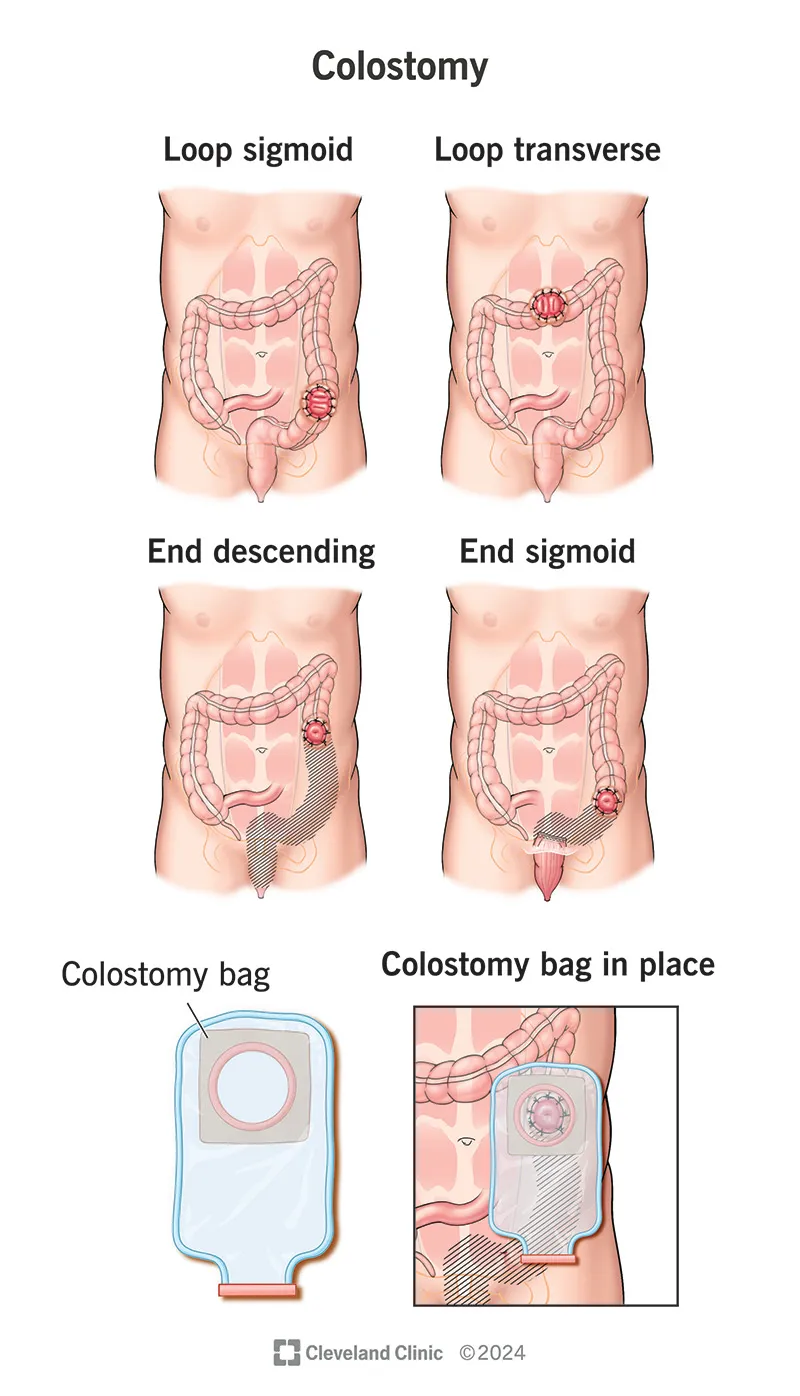
| Feature | Ileostomy | Colostomy |
|---|---|---|
| Location | Usually RIF | Usually LIF, Transverse colon |
| Effluent | Liquid, continuous, enzyme-rich | Semi-solid to formed, intermittent |
| Protrusion | Spouted (2-3 cm) | Flush or <1 cm |
| Complications | High output, dehydration, skin excoriation | Obstruction, prolapse, parastomal hernia |
Stoma Creation - Site & Snip
- Pre-operative Siting (📌 VISIBLE Mnemonic):
- Visible: To patient for self-care.
- Incision-away: From surgical incision, scars.
- Rectus-traversing: Through rectus abdominis muscle.
- Skin-crease free: Away from folds, umbilicus.
- Bony-prominence free: Avoid iliac crest.
- Level surface: For good appliance seal.
- Easy access: For stoma care.
- Site on apex of infra-umbilical fat fold.
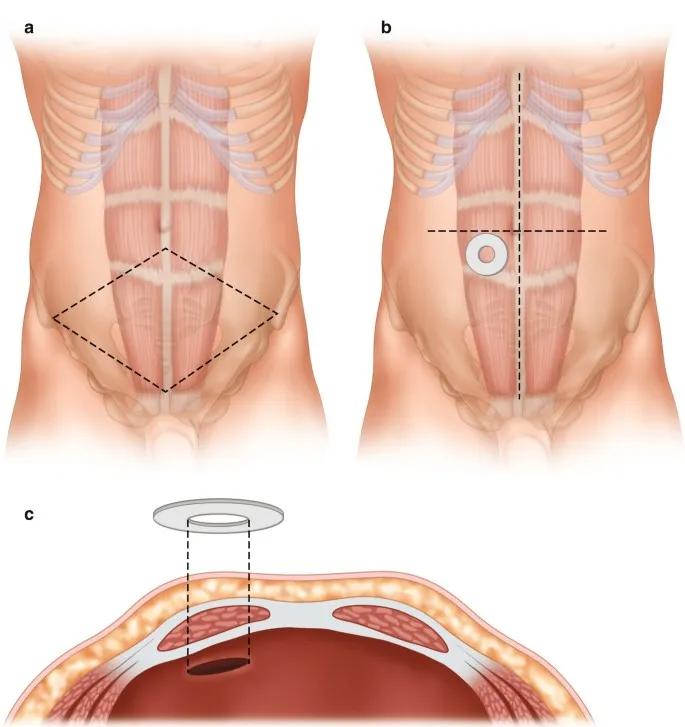
- Surgical Steps:
- Trephine: Skin disc excised (match bowel diameter, often 2-3 cm); abdominal wall layers incised.
- Bowel mobilization: Tension-free exteriorization.
- Maturation:
- End (e.g., Brooke ileostomy): Everted, sutured to skin.
- Loop: Opened, edges sutured to skin; rod optional.
⭐ Passing the stoma through the rectus abdominis muscle significantly reduces parastomal hernia risk.
Stoma Complications - When Holes Go Haywire
📌 Mnemonic for early complications: 'RASH IN M.E.' (Retraction, Abscess, Sepsis, Hemorrhage, Ischemia, Necrosis, Mucocutaneous separation, Edema).
| Type | Complications & Key Features/Management Hints |
|---|---|
| Early | Ischemia/Necrosis (dusky/black; urgent revision if deep), Retraction (may need revision), Mucocutaneous separation (local care/revision), Hemorrhage (local pressure; explore if severe), Infection (antibiotics, drainage). High output state (>1.5-2L/day; fluids, loperamide), Edema (usually self-limiting). |
| Late | Stenosis (dilation/revision), Prolapse (manual reduction/revision), Parastomal hernia (most common; support belt/repair), Dermatitis (skin barrier, topical agents), Fistula (conservative/surgical), Obstruction (investigate cause). Gallstones (↑ risk post-ileostomy), Psychological issues. |
⭐ Parastomal hernia is the most common late complication of stomas.
Living with a Stoma - Pouch & Practicalities
-
Stoma Appliances:
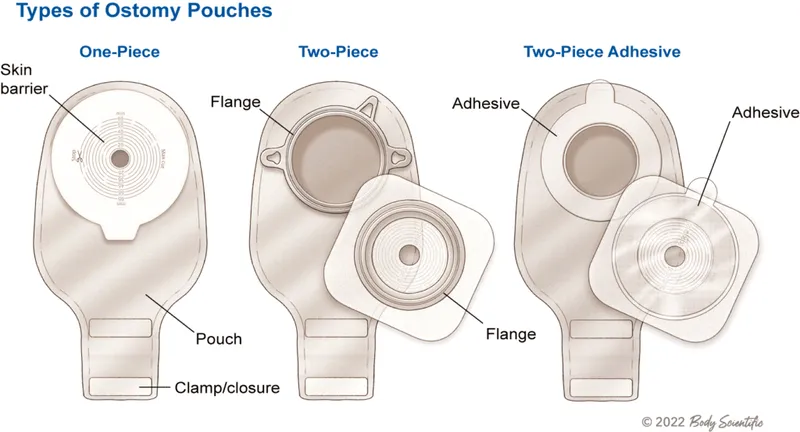
- Types: One-piece or two-piece systems.
- Bags: Drainable (ileostomy/high-output) vs. closed (colostomy).
- Convexity inserts for flush/retracted stomas.
-
Skin Care:
- Barrier creams/powders protect peristomal skin.
- Proper pouch fit prevents leakage.
-
Dietary Considerations:
Feature Ileostomy Colostomy Initial Diet Low-residue Fewer restrictions Hydration/Salt Crucial; output 500-800 ml/day (adapted) Important Blockage Risk Higher; Avoid 📌 COPS (Corn, Coconut, Orange pith, Popcorn, Peas, Pineapple, Skins, Seeds, Stringy veg) Lower Gas/Odor Manageable Manage gas/odor -
Monitoring & Support:
- Check electrolytes, Vit B12 (terminal ileostomy).
- Psychosocial support essential.
⭐ Patients with terminal ileostomies often require lifelong Vitamin B12 supplementation.
High‑Yield Points - ⚡ Biggest Takeaways
- Ileostomy: liquid, enzyme-rich output, continuous; skin protection crucial.
- Colostomy output: varies by site: ascending (liquid), transverse (semi-formed), sigmoid (formed).
- Loop stomas: usually temporary, two openings. End stomas can be permanent.
- Complications: prolapse, retraction, stenosis, parastomal hernia, dermatitis.
- High-output stomas (>1.5L/day): risk dehydration, electrolyte imbalance (K+, Mg++ loss).
- Brooke ileostomy: everted mucosa forms spout, minimizing skin contact.
- Hartmann's procedure: results in end colostomy and rectal stump.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

