Epidemiology & Risk Factors - Cancer's Coordinates
- Incidence: 3rd most common cancer worldwide (men), 2nd (women).
- Age: Peak incidence >50 years; rising in younger adults.
- Geography: Higher in developed countries (Western diet/lifestyle).
- **Risk Factors (Modifiable):
- Diet: ↓Fiber, ↑Red/processed meat, ↑Fat.
- Lifestyle: Obesity, physical inactivity, smoking, alcohol.
- **Risk Factors (Non-Modifiable):
- Personal history: Adenomatous polyps, IBD (UC > Crohn's).
- Family history: CRC or adenomatous polyps in 1st-degree relative.
- Hereditary syndromes: FAP, Lynch syndrome (HNPCC).
⭐ Lynch syndrome accounts for 2-4% of all CRCs; associated with multiple extracolonic cancers (endometrial, ovarian, gastric).
Pathogenesis & Polyps - From Polyp to Problem
- CRC develops via adenoma-carcinoma sequence (commonest) or serrated pathway.
- Key Genetic Pathways:
- Chromosomal Instability (CIN) Pathway (~85%):
- Sequential APC (gatekeeper), KRAS, TP53 mutations.
- Linked to FAP.
- Microsatellite Instability (MSI) Pathway (~15%):
- Defective DNA Mismatch Repair (dMMR) genes (e.g., MLH1, MSH2).
- Linked to Lynch Syndrome (HNPCC).
- Often right-sided, mucinous.
- Chromosomal Instability (CIN) Pathway (~85%):
- Polyps as Precursors:
- Adenomatous (Neoplastic):
- Tubular: Most common (~75%), lowest malignant risk.
- Villous: Highest malignant risk (~40%).
- Tubulovillous: Intermediate.
- Serrated:
- Hyperplastic: Small, benign, usually left-sided.
- Sessile Serrated Adenoma/Polyp (SSA/P): Premalignant, right-sided, BRAF mutation.
- Adenomatous (Neoplastic):
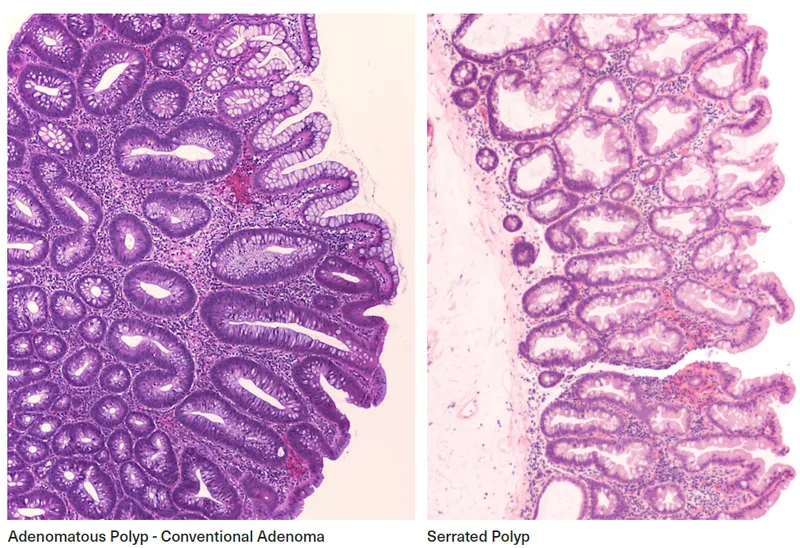
⭐ Villous adenomas exhibit the highest malignant potential among adenomatous polyps, approaching 40%.
Clinical Features & Diagnosis - Detecting Danger
- Often asymptomatic; symptoms depend on tumor location:
- Right-sided: Occult bleeding → iron deficiency anemia, fatigue, vague abdominal pain.
- Left-sided: Altered bowel habits (constipation/diarrhea), visible rectal bleeding (hematochezia), tenesmus, obstructive symptoms.
- General: Unexplained weight loss, anorexia.
- ⚠️ Alarm symptoms: Persistent change in bowel habit (>6 wks), PR bleeding, unexplained weight loss, iron deficiency anemia (especially in males/post-menopausal females), palpable abdominal mass.
- Diagnosis:
- History, Physical Exam (incl. Digital Rectal Exam - DRE).
- Labs: CBC (anemia), LFTs. Carcinoembryonic Antigen (CEA) for prognosis & recurrence monitoring (not screening).
- Colonoscopy: Gold standard for diagnosis & biopsy.
- Imaging for staging:
- CT (Chest/Abdomen/Pelvis) for TNM staging.
- MRI Pelvis: Essential for rectal cancer local staging (esp. mesorectal fascia).
- Endorectal Ultrasound (ERUS): T-staging in early rectal cancers.
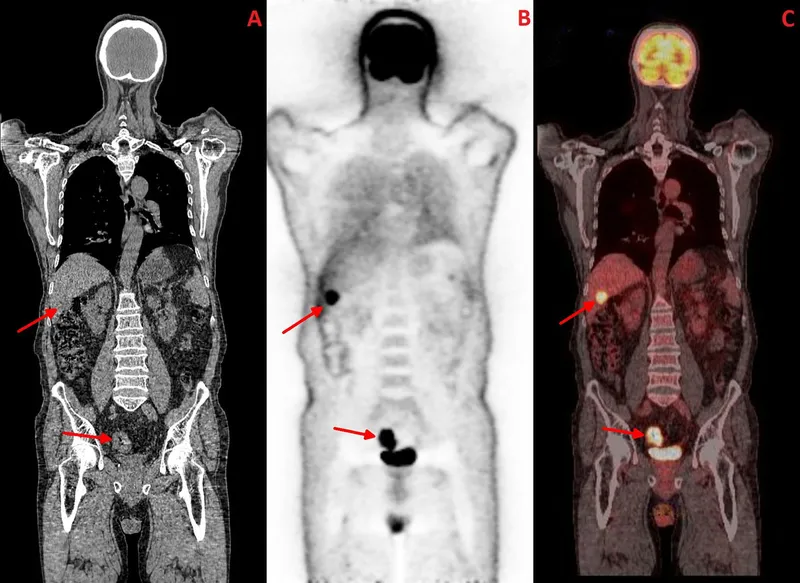
⭐ Carcinoembryonic Antigen (CEA) levels >5 ng/mL pre-operatively are associated with a worse prognosis in colorectal cancer patients and can indicate residual disease if elevated post-operatively.
Staging & Management - Battle Blueprint
- Staging Workup:
- Colonoscopy + Biopsy (diagnostic)
- CT Chest/Abdomen/Pelvis (metastasis screen)
- MRI Pelvis (essential for rectal cancer: T-stage, N-stage, Circumferential Resection Margin - CRM)
- CEA (baseline & prognostic/monitoring marker)
- TNM Staging (AJCC): Core to treatment planning.
- Colon Cancer Management:
- Primary Treatment: Segmental colectomy + adequate lymphadenectomy (aim for ≥12 nodes).
- Adjuvant Chemotherapy: For all Stage III and high-risk Stage II (e.g., T4, perforation, poor differentiation).
- Rectal Cancer Management:
- Early (e.g., cT1N0 low-risk): Local excision (TEMS/TAMIS) or Total Mesorectal Excision (TME).
- Locally Advanced (cT3/T4 or N+): Neoadjuvant Chemoradiotherapy (NCRT) → TME → Adjuvant Chemotherapy.
- Very low tumors may require Abdominoperineal Resection (APR).
- Metastatic Disease (Stage IV):
- Palliative chemotherapy +/- targeted agents (based on KRAS, NRAS, BRAF, MSI status).
- Surgery for resectable metastases (liver, lung) in select cases.

⭐ For rectal cancer, achieving a clear Circumferential Resection Margin (CRM > 1mm) on pathology post-TME is a critical determinant of local recurrence and survival; pre-operative MRI helps predict CRM involvement.
High‑Yield Points - ⚡ Biggest Takeaways
- FAP (APC gene) & Lynch syndrome (MMR genes) are major hereditary risks.
- Right-sided lesions: anemia, occult blood. Left-sided: altered bowel habits, obstruction.
- Colonoscopy is gold standard for screening & diagnosis.
- CEA is for prognosis & recurrence monitoring, not screening.
- Liver is the most common site for distant metastasis.
- Rectosigmoid junction is the most frequent location.
- Surgical resection is the primary curative treatment for localized disease.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

