Anorectal Anatomy & Physiology - Foundation First
- Anal Canal: Length: Anatomical ~4 cm, surgical 2-3 cm.
- Dentate (Pectinate) Line: Embryological division (endoderm/ectoderm). Columnar above, squamous below.
- Hilton's Line: Intersphincteric groove.
- Sphincters:
- Internal (IAS): Involuntary, smooth muscle, main resting tone.
- External (EAS): Voluntary, striated muscle, pudendal nerve (S2-S4), squeeze.
- Blood Supply:
- Above Dentate: Superior Rectal Artery (IMA); portal drainage.
- Below Dentate: Inferior Rectal Artery (Internal Pudendal); systemic drainage.
- Nerve Supply:
- Above Dentate: Autonomic (dull pain/pressure).
- Below Dentate: Somatic (Inferior Rectal N. - sharp pain).
- Lymphatics: 📌 "Above Internal, Below Groin"
- Above Dentate: Internal iliac nodes.
- Below Dentate: Superficial inguinal nodes.

⭐ The dentate line dictates epithelium, neurovascular supply, lymphatic drainage, and thus pathology (e.g., internal vs. external hemorrhoids, pain perception).
Hemorrhoids & Anal Fissure - Painful Problems
Hemorrhoids: Dilated submucosal vascular cushions.
- Types: Internal (above dentate line), External (below dentate line).
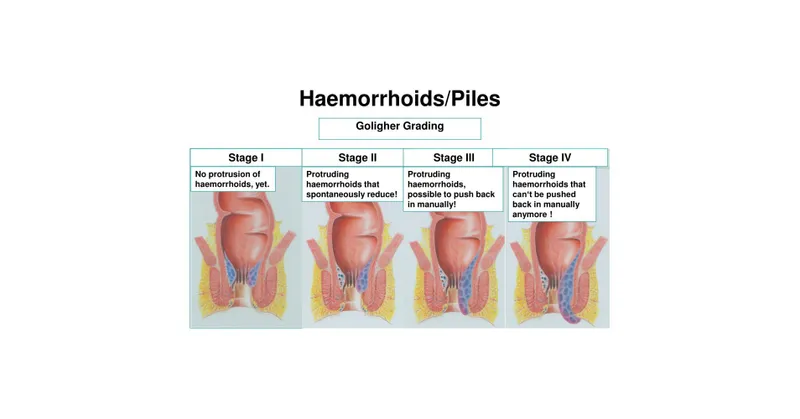
- Goligher's Classification (Internal):
- Grade I: Bleeds, no prolapse.
- Grade II: Prolapses, reduces spontaneously.
- Grade III: Prolapses, requires manual reduction.
- Grade IV: Irreducible prolapse.
- Clinical Features: Painless bleeding (internal), pain (external, thrombosed internal), pruritus, prolapse.
- Management:
- Conservative: High-fiber diet, sitz baths, adequate fluids.
- Medical: Stool softeners, topical anesthetics/steroids.
- Non-operative (Grades I-III): Rubber band ligation (RBL), Sclerotherapy, Infrared coagulation (IRC).
- Surgical (Grades III-IV, failed non-op): Hemorrhoidectomy (Milligan-Morgan - open; Ferguson - closed), Stapled hemorrhoidopexy.
Anal Fissure: Linear tear/ulcer in anoderm, distal to dentate line.
- Types: Acute (<6 weeks), Chronic (>6 weeks; often with sentinel pile, hypertrophied anal papilla).
- Etiology: Hypertonic Internal Anal Sphincter (IAS), trauma from hard stools.
- Typical Location: Posterior midline (most common). Anterior midline (more common in females).

- Clinical Features: Severe tearing pain during/after defecation, bright red blood per rectum (BRBPR).
- Management:
- Conservative: Sitz baths, stool softeners, high-fiber diet.
- Medical: Topical 0.2% Glyceryl Trinitrate (GTN) ointment, topical 2% Diltiazem cream.
- Surgical (Chronic, failed medical): Lateral Internal Sphincterotomy (LIS) - Gold Standard.
⭐ The most common site for an anal fissure is the posterior midline.
Anorectal Abscess & Fistula - Deep Dive Drains
Anorectal Abscess: Localized pus collection.
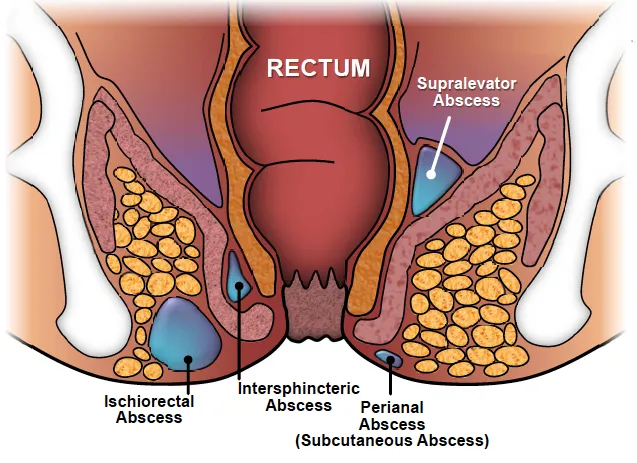
- Types: Perianal (most common,
60%), Ischiorectal (20%), Intersphincteric (5%), Supralevator (4%).- Clinical: Acute pain, swelling, fluctuance, fever.
- Microbiology: Polymicrobial (E. coli, Bacteroides spp.).
- Management: Prompt Incision & Drainage (I&D). Antibiotics if cellulitis/systemic signs/immunocompromised.
Fistula-in-ano: Chronic abnormal tract between anal canal epithelium and perianal skin.
- Etiology: Cryptoglandular (most common); Crohn's, TB, malignancy.
- Goodsall's Rule: Predicts tract path.
- Anterior external opening: Straight radial tract.
- Posterior external opening: Curved tract to posterior midline.
- Exception: Anterior opening >3 cm from anal verge may curve posteriorly. ⭐> Goodsall's rule helps predict the track of a fistula-in-ano based on the external opening's location relative to the transverse anal line.
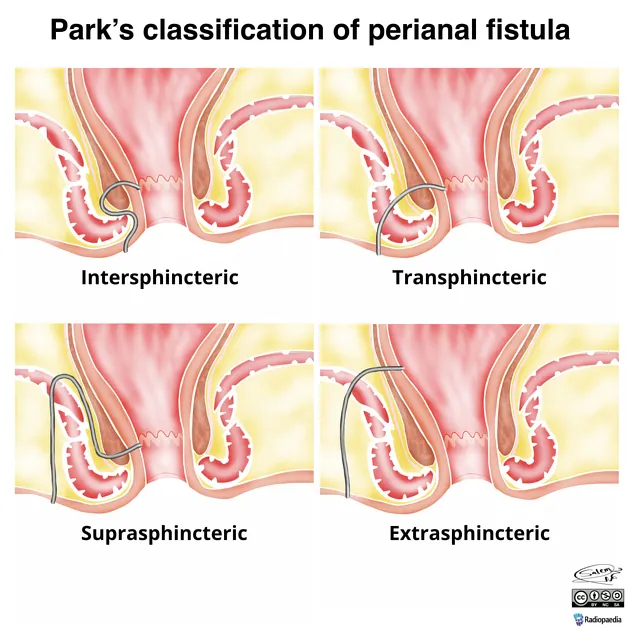
- Parks' Classification: (📌 Mnemonic: "ITSE" - In The Sphincter Eventually)
Type Description Frequency Intersphincteric Between internal & external sphincters ~70% Transsphincteric Crosses both sphincters ~25% Suprasphincteric Tract passes above puborectalis muscle ~5% Extrasphincteric Tract passes outside sphincter complex ~1%
-
Investigations: MRI (gold standard for complex/recurrent), EUA (Examination Under Anesthesia).
-
Management Principles: Eradicate sepsis, heal tract, preserve sphincter function, prevent recurrence.
- Options: FistuLOTOMY (lay open), FistuLECTOMY (excision), Seton, LIFT, VAAFT, Advancement Flaps. Choice depends on tract complexity & sphincter integrity.
Other Anorectal Conditions - Beyond the Basics
- Pilonidal Sinus: Natal cleft hair follicle blockage. Features: pain, swelling, discharge. Management: hygiene, I&D (abscess), excision (e.g., Karydakis).

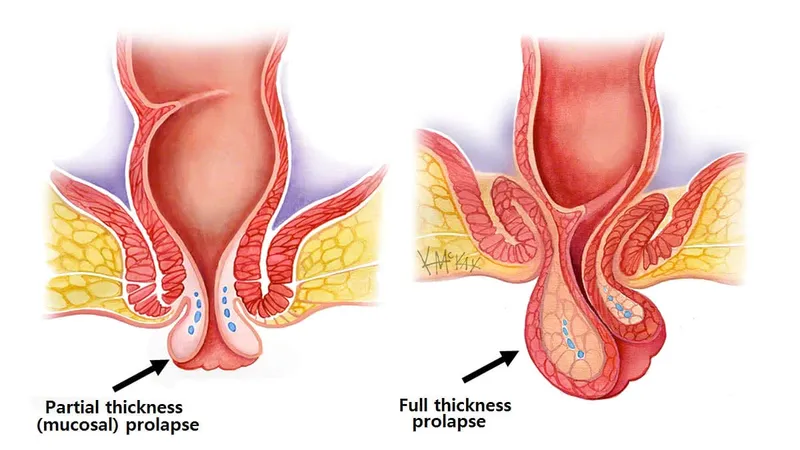
- Rectal Prolapse: Types: Mucosal, Full-thickness (Procidentia). Features: concentric mucosal folds, mass, incontinence. Differentiate: hemorrhoids (radial folds). Management: conservative; surgical (e.g., Delorme, rectopexy).
- Pruritus Ani: Common causes: idiopathic, poor hygiene, infections (fungal, pinworm), skin conditions (eczema). Investigation: clinical. Management: address cause, hygiene, topical steroids (short-term).
- Anal Canal Tumors: Types: Squamous Cell Carcinoma (SCC - most common, HPV-related), adenocarcinoma, melanoma. Features: bleeding, pain, mass. Staging: TNM (brief). Management: SCC (Nigro protocol: chemoradiation), others (surgery).
⭐ Squamous cell carcinoma is the most common anal canal malignancy, often HPV-linked.
High‑Yield Points - ⚡ Biggest Takeaways
- Internal hemorrhoids: painless bleeding, above dentate line; Grade IV irreducible.
- Anal fissure: posterior midline most common; lateral suggests Crohn's/TB. Sentinel pile is key.
- Perianal abscess is most frequent; supralevator abscess is deep and often missed.
- Fistula-in-ano: Goodsall's rule predicts internal opening; Seton for complex types.
- Pilonidal sinus: Acquired, midline pits in natal cleft, common in hirsute individuals.
- Anal canal cancer: Squamous Cell Carcinoma (SCC) is most common, strongly HPV-associated.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

