Gastrointestinal Surgery

On this page
🗺️ The Alimentary Arsenal: Your Surgical Roadmap
The gastrointestinal tract spans 9 meters from mouth to anus, yet surgical pathology clusters in predictable anatomical hotspots. Understanding this distribution transforms random facts into systematic knowledge. The appendix sits at the McBurney point (one-third the distance from anterior superior iliac spine to umbilicus), the gastroesophageal junction lies at T10-T11, and the rectum begins at S3 where the taenia coli coalesce. Each region presents distinct pathology requiring tailored surgical approaches.
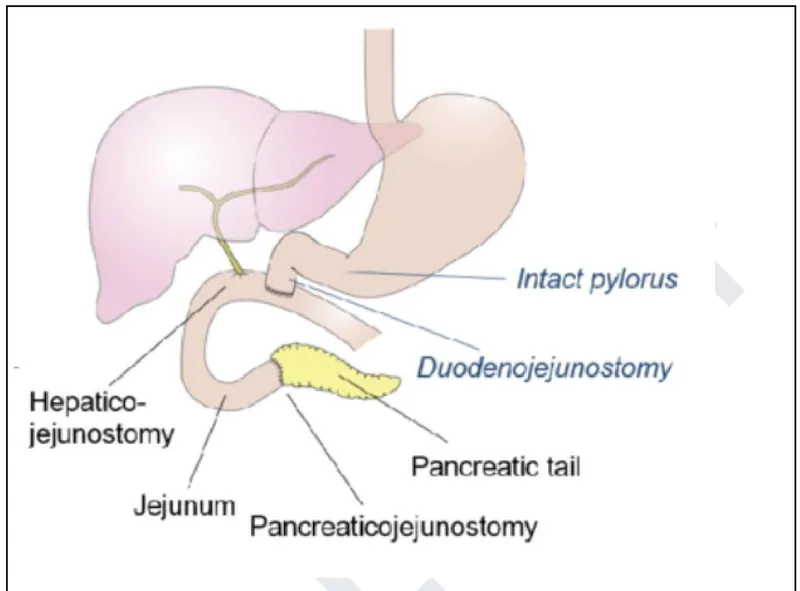
Anatomical Zones & Surgical Significance
-
Esophageal Territory (25 cm length)
- Upper third: striated muscle, cervical approach
- Middle third: mixed muscle, thoracotomy access
- Lower third: smooth muscle, abdominal approach
- Critical transition at 40 cm from incisors (GE junction)
- Blood supply: inferior thyroid (upper), bronchial (middle), left gastric (lower)
-
Gastroduodenal Zone
- Stomach capacity: 1500 mL distended
- Pylorus at L1 vertebral level
- Duodenal C-loop embraces pancreatic head
- 90% of peptic ulcers occur in first 3 cm of duodenum
- Gastric emptying half-time: 90-120 minutes for solids
-
Small Bowel Domain (6 meters)
- Jejunum: 2.5 meters, thick walls, prominent plicae
- Ileum: 3.5 meters, thinner walls, Peyer patches
- Blood supply: 15-18 arcades of superior mesenteric artery
- Ischemia threshold: <40 mmHg mesenteric pressure
- Absorptive surface: 200 m² with villi
-
Colonic Corridor
- Total length: 150 cm from cecum to rectum
- Cecal diameter: 9 cm (largest, most prone to perforation)
- Watershed zones: splenic flexure, rectosigmoid junction
- Arterial supply switches at splenic flexure (SMA → IMA)
- Rectal blood supply: superior, middle, inferior hemorrhoidal arteries
📌 Remember: LAW of LaPlace predicts perforation risk: Wall tension = (Pressure × Radius) / (2 × Wall thickness). The cecum perforates first in distal obstruction because it has the largest radius despite lower intraluminal pressure.

Regional Pathology Distribution
| Region | Common Pathology | Peak Age | Malignancy Risk | Surgical Urgency |
|---|---|---|---|---|
| Esophagus | GERD, achalasia, cancer | 50-70 yr | 15-20% Barrett's → CA | Elective (perforation: emergent) |
| Stomach | PUD, cancer, outlet obstruction | 40-60 yr | 10% ulcers malignant | Variable (perforation: emergent) |
| Small bowel | Obstruction, Crohn's, tumors | 30-50 yr | <5% neoplasms | 80% obstructions emergent |
| Appendix | Appendicitis | 10-30 yr | <1% carcinoid | 95% within 24 hours |
| Colon | Diverticulitis, cancer, IBD | 50-70 yr | 5% lifetime risk | 20% require urgent surgery |
| Rectum | Hemorrhoids, fissures, cancer | 40-60 yr | 40% colorectal CA here | Mostly elective |
⭐ Clinical Pearl: 80% of gastrointestinal emergencies involve either obstruction, perforation, or hemorrhage. Master these three presentations, and you command 90% of urgent surgical decision-making.
Embryological Foundations
-
Foregut derivatives (esophagus to second duodenum)
- Arterial supply: celiac trunk
- Vagal innervation: anterior and posterior trunks
- Pain referral: epigastric region
- Venous drainage: portal system
-
Midgut derivatives (third duodenum to proximal two-thirds transverse colon)
- Arterial supply: superior mesenteric artery
- Rotation: 270 degrees counterclockwise in utero
- Pain referral: periumbilical region
- Malrotation complications: volvulus risk
-
Hindgut derivatives (distal third transverse colon to anal canal)
- Arterial supply: inferior mesenteric artery
- Dual innervation: autonomic (proximal) + somatic (distal)
- Pain referral: suprapubic and perineal
- Venous drainage: portal + systemic (hemorrhoid zones)
💡 Master This: Embryological blood supply predicts surgical approach. Foregut lesions require celiac axis control, midgut pathology demands SMA assessment, and hindgut disease involves IMA ligation. This knowledge guides every oncologic resection and vascular emergency.
Connect these anatomical foundations through functional physiology to understand how structure enables surgical disease patterns.
🗺️ The Alimentary Arsenal: Your Surgical Roadmap
📚 The Inflammatory Cascade: From Irritation to Intervention
Gastrointestinal inflammation follows predictable molecular pathways that determine surgical timing. Understanding the progression from mucosal injury to transmural necrosis transforms reactive surgery into strategic intervention. The inflammatory cascade begins with epithelial barrier disruption, progresses through neutrophil infiltration within 2-4 hours, and culminates in tissue destruction by 12-24 hours without treatment.
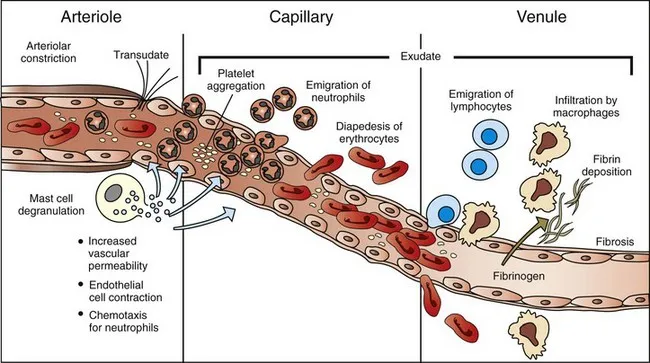
Inflammatory Progression Timeline
-
Phase 1: Mucosal Injury (0-2 hours)
- Epithelial tight junction breakdown
- Bacterial translocation begins at 2 hours
- Local cytokine release: IL-1, IL-6, TNF-α
- Prostaglandin synthesis increases 10-fold
- Reversible with conservative management
-
Phase 2: Neutrophil Invasion (2-8 hours)
- Leukocyte adhesion molecule expression
- Transmigration into submucosa
- Reactive oxygen species production
- Tissue edema increases 30-50%
- Window for antibiotic efficacy
-
Phase 3: Transmural Extension (8-24 hours)
- Full-thickness wall involvement
- Serosal inflammation visible
- Peritoneal irritation signs emerge
- Perforation risk increases 5-fold
- Surgical intervention often required
-
Phase 4: Necrosis & Perforation (>24 hours)
- Tissue infarction develops
- Free perforation in 15-30%
- Abscess formation in 40-60%
- Mortality increases 3-fold vs. early surgery
- Damage control surgery indicated
📌 Remember: SIRS criteria predict surgical timing: ≥2 of 4 (Temperature >38°C or <36°C, Heart rate >90, Respiratory rate >20, WBC >12,000 or <4,000) within 6 hours of symptom onset indicates 70% likelihood of requiring operative intervention.
Pathophysiological Mechanisms by Organ
-
Appendiceal Inflammation
- Luminal obstruction in 60-80% (fecalith, lymphoid hyperplasia)
- Intraluminal pressure rises from 10 mmHg to 60 mmHg
- Venous congestion at 20 mmHg → arterial compromise at 40 mmHg
- Perforation occurs when wall tension exceeds 80 mmHg
- Time to perforation: 24-36 hours from symptom onset
- Pediatric perforation rate: 30-40% (thinner wall, delayed diagnosis)
-
Diverticular Inflammation
- Microperforation of diverticulum in 90% of cases
- Pericolic fat inflammation contains 70% of episodes
- Free perforation in 1-2% (Hinchey stage IV)
- Abscess formation in 15-20% (Hinchey stage II-III)
- Recurrence after first episode: 25% within 5 years
- Immunosuppression increases perforation risk 4-fold
-
Inflammatory Bowel Disease
- Crohn's: transmural inflammation, skip lesions
- Ulcerative colitis: mucosal/submucosal, continuous
- Toxic megacolon: colon diameter >6 cm with systemic toxicity
- Perforation risk in toxic megacolon: 15-20%
- Free perforation mortality: 30-50% if delayed >24 hours
- Fistula formation in Crohn's: 30-40% over lifetime

⭐ Clinical Pearl: The "golden 24 hours" principle applies across GI inflammation. Appendicitis perforation increases from 10% at 24 hours to 50% at 48 hours. Diverticulitis managed conservatively has 80% success if started within 24 hours versus 40% after 48 hours.
Inflammatory Markers & Surgical Decision Points
| Marker | Normal | Mild Inflammation | Moderate | Severe (Surgery Likely) | Peak Time |
|---|---|---|---|---|---|
| WBC count | 4-11 K/μL | 11-15 K/μL | 15-20 K/μL | >20 K/μL | 12-24 hr |
| CRP | <10 mg/L | 10-50 mg/L | 50-150 mg/L | >150 mg/L | 24-48 hr |
| Procalcitonin | <0.5 ng/mL | 0.5-2 ng/mL | 2-10 ng/mL | >10 ng/mL | 6-12 hr |
| Lactate | <2 mmol/L | 2-4 mmol/L | 4-6 mmol/L | >6 mmol/L | 2-6 hr |
| Neutrophil % | 40-70% | 70-80% | 80-90% | >90% | 6-12 hr |
💡 Master This: Serial inflammatory markers predict surgical need better than single values. CRP doubling within 24 hours or procalcitonin >2 ng/mL at presentation indicates 85% likelihood of failed conservative management in diverticulitis. Lactate >4 mmol/L suggests ischemia requiring urgent exploration.
Antibiotic Penetration & Timing
-
Tissue penetration varies by antibiotic class
- Fluoroquinolones: 80-100% tissue concentration
- Metronidazole: 90-100% anaerobic coverage
- Carbapenems: 60-80% tissue levels
- Aminoglycosides: 30-50% penetration (poor in abscess)
- Cephalosporins: 50-70% with adequate perfusion
-
Critical timing thresholds
- Antibiotics within 1 hour: 90% efficacy for uncomplicated cases
- Delayed >6 hours: efficacy drops to 60%
- After 24 hours: <40% response in complicated disease
- Abscess >3 cm: antibiotics alone fail in 80%
- Perforation present: antibiotics adjunctive only
⚠️ Warning: Never delay surgery for antibiotic trial when free perforation is suspected. Mortality increases 15% for every 6-hour delay beyond diagnosis. The "sun should never set" on free intra-abdominal contamination.
Connect these inflammatory mechanisms through pattern recognition frameworks to identify surgical candidates early.
📚 The Inflammatory Cascade: From Irritation to Intervention
🔬 Pattern Recognition Mastery: The Diagnostic Framework
Surgical gastrointestinal disease presents with overlapping symptoms requiring systematic discrimination. Master the "pain-perforation-peritonitis" triad, and you identify 95% of surgical emergencies. Abdominal pain location predicts pathology with 75-85% accuracy, but migration patterns and associated symptoms refine diagnosis to >90% certainty.
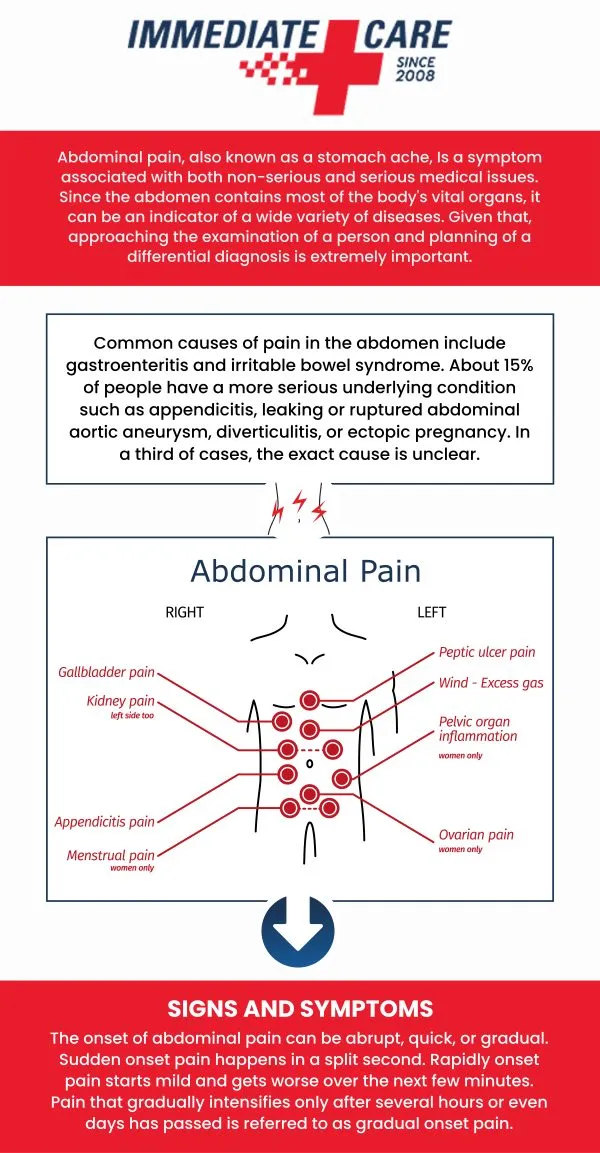
Pain Pattern Analysis
-
Right Lower Quadrant Pain
- Appendicitis: periumbilical → RLQ migration in 60-80%
- Time to migration: 6-12 hours (classic presentation)
- Anorexia present in 80%, vomiting in 60%
- Fever typically low-grade (<38.5°C) early
- Rovsing sign: 60% sensitive, 80% specific
- Psoas sign: positive in 40% retrocecal appendicitis
- Obturator sign: positive in 30% pelvic appendicitis
-
Left Lower Quadrant Pain
- Diverticulitis: "left-sided appendicitis" in 70%
- Age typically >50 years (vs. appendicitis <40 years)
- Fever higher (>38.5°C) in 50%
- Palpable mass in 20% (phlegmon/abscess)
- Urinary symptoms in 30% (bladder irritation)
- Prior episodes in 40% of presentations
-
Epigastric Pain
- Peptic ulcer: burning, meal-related in 70%
- Perforated ulcer: sudden, severe, board-like rigidity
- Free air under diaphragm in 75% of perforations
- Gastric outlet obstruction: postprandial vomiting
- Succussion splash positive after >4 hours fasting
-
Diffuse Abdominal Pain
- Intestinal obstruction: colicky, crescendo pattern
- Pain-free intervals early, constant in strangulation
- Vomiting: early in proximal, late in distal obstruction
- Bowel sounds: hyperactive early, absent late
- Tympany on percussion in 90% of cases
📌 Remember: PQRST pain assessment - Provocation (what worsens?), Quality (sharp vs. dull), Radiation (where spreads?), Severity (1-10 scale), Timing (sudden vs. gradual). Document all five elements for every acute abdomen.
Physical Examination Hierarchy
-
Inspection findings (perform first, before palpation)
- Distension: suggests obstruction or ileus
- Visible peristalsis: proximal obstruction in thin patients
- Surgical scars: adhesive obstruction in 60-75%
- Hernias: 10-15% of obstructions (examine all orifices)
- Ecchymosis: Grey Turner (flank) or Cullen (periumbilical) suggests hemorrhage
-
Auscultation patterns (perform before palpation to avoid artifact)
- Normal: 5-35 sounds/minute
- Hyperactive: >35/min suggests early obstruction
- High-pitched/tinkling: mechanical obstruction pathognomonic
- Absent sounds: ileus or late obstruction after >6 hours
- Succussion splash: gastric outlet obstruction
-
Percussion significance
- Tympany: gas-filled loops in obstruction
- Shifting dullness: ascites (>500 mL detectable)
- Loss of liver dullness: pneumoperitoneum in 30% of perforations
- Rebound tenderness: peritoneal irritation (test gently)
-
Palpation sequence (perform last to avoid guarding)
- Start away from pain to gain patient trust
- Voluntary guarding: patient can relax on command
- Involuntary guarding: rigid, cannot relax (peritonitis)
- Rebound tenderness: peritoneal inflammation
- Murphy sign: inspiratory arrest in cholecystitis (85% sensitive)
- Rovsing sign: RLQ pain with LLQ palpation (appendicitis)
⭐ Clinical Pearl: Carnett test distinguishes visceral from abdominal wall pain with 85% accuracy. Have patient tense abdominal muscles (lift head/legs). Pain that increases is abdominal wall origin; pain that decreases is visceral origin.
Scoring Systems for Surgical Decision
-
Alvarado Score for Appendicitis (max 10 points)
- Migration of pain: 1 point
- Anorexia: 1 point
- Nausea/vomiting: 1 point
- RLQ tenderness: 2 points
- Rebound pain: 1 point
- Fever >37.3°C: 1 point
- Leukocytosis >10,000: 2 points
- Left shift >75% neutrophils: 1 point
- Score ≥7: 85% sensitivity for appendicitis
- Score ≤4: <10% likelihood, safe discharge
- Score 5-6: 50% risk, imaging recommended
-
Hinchey Classification for Diverticulitis
- Stage I: pericolic abscess (CT drainage + antibiotics)
- Stage II: pelvic abscess (drainage + delayed surgery)
- Stage III: purulent peritonitis (surgery within 6-12 hours)
- Stage IV: fecal peritonitis (emergency surgery, mortality 30-40%)
- Stages I-II: 80% success with conservative management
- Stages III-IV: surgery mandatory, delay increases mortality 10%/6 hours
| Clinical Feature | Appendicitis | Diverticulitis | Perforated Ulcer | Small Bowel Obstruction |
|---|---|---|---|---|
| Typical age | 10-30 yr | >50 yr | 40-60 yr | Any (prior surgery) |
| Pain onset | Gradual 6-12 hr | Gradual 12-24 hr | Sudden <1 hr | Gradual/crescendo |
| Pain location | Periumbilical→RLQ | LLQ | Epigastric→diffuse | Periumbilical/diffuse |
| Fever | Low <38.5°C | Moderate >38.5°C | Variable | Low/absent early |
| WBC | 12-15 K/μL | 15-20 K/μL | 15-25 K/μL | 10-15 K/μL |
| Key imaging | CT: fat stranding | CT: wall thickening | XR: free air 75% | XR: air-fluid levels |
💡 Master This: The "see-think-do" algorithm for acute abdomen: See peritoneal signs → Think perforation/ischemia → Do immediate imaging and surgical consultation. Never delay surgery for "just one more test" when peritonitis is evident. Clinical examination trumps imaging when findings are unequivocal.
Connect these recognition patterns through differential diagnosis frameworks to distinguish similar presentations systematically.
🔬 Pattern Recognition Mastery: The Diagnostic Framework
🏥 The Differential Matrix: Systematic Discrimination
Overlapping presentations in gastrointestinal surgery demand structured comparison. The key discriminators are age, onset timing, pain character, and imaging findings. Master these four parameters, and you achieve >90% diagnostic accuracy before entering the operating room.
Age-Based Probability Stratification
-
Pediatric (<18 years): 70% appendicitis dominance
- Appendicitis: 60-70% of acute abdomen
- Intussusception: peak 6-36 months, "currant jelly" stools
- Meckel diverticulum: 2% population, symptomatic in 4%
- Malrotation with volvulus: 75% present <1 year
- Perforated viscus rare unless trauma
-
Young Adult (18-40 years): inflammatory predominance
- Appendicitis: 40-50% of surgical abdomen
- IBD complications: peak onset 15-35 years
- Small bowel obstruction: adhesions if prior surgery
- Perforated ulcer: <5% (H. pylori declining)
- Diverticulitis: <5% (but more aggressive when present)
-
Middle Age (40-60 years): transitional pathology
- Diverticulitis: 30-40% of LLQ pain
- Colorectal cancer: incidence rises 50-fold vs. age 20
- Peptic ulcer disease: peak incidence
- Biliary disease: gallstones in 20-30%
- Small bowel obstruction: adhesions 60%, hernia 20%
-
Elderly (>60 years): vascular and neoplastic risk
- Mesenteric ischemia: mortality 60-80% if delayed
- Colorectal cancer: 70% of all cases
- Diverticulitis: 50% prevalence by age 70
- Incarcerated hernia: mortality 10% if strangulated
- Volvulus: sigmoid 80%, cecal 20%
📌 Remember: "VINDICATE" mnemonic for differential diagnosis - Vascular, Infectious, Neoplastic, Degenerative, Inflammatory, Congenital, Autoimmune, Traumatic, Endocrine/metabolic. Apply systematically to every acute abdomen.
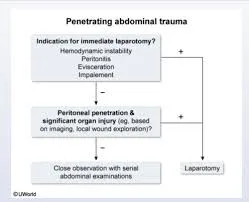
Onset Timing as Diagnostic Discriminator
-
Sudden onset (<1 hour to peak pain): catastrophic events
- Perforated viscus: "worst pain of life" in 80%
- Mesenteric ischemia: "pain out of proportion" to exam
- Ruptured aneurysm: shock in 60% at presentation
- Ovarian torsion: severe unilateral pain (women)
- Ectopic pregnancy rupture: positive β-hCG, shock
- Immediate imaging and surgical consultation mandatory
-
Rapid onset (1-6 hours): acute inflammation/obstruction
- Appendicitis: progressive over 6-12 hours
- Cholecystitis: postprandial, RUQ radiation
- Ureteral colic: colicky, flank-to-groin radiation
- Incarcerated hernia: visible/palpable bulge
- Small bowel obstruction: colicky, vomiting
-
Gradual onset (>12 hours): indolent processes
- Diverticulitis: days of discomfort before presentation
- Inflammatory bowel disease: chronic-on-acute
- Gastric outlet obstruction: weeks of symptoms
- Early appendicitis: vague periumbilical discomfort
- Partial obstruction: intermittent symptoms
⭐ Clinical Pearl: "Pain out of proportion to physical findings" is the hallmark of mesenteric ischemia in 75% of cases. Suspect in patients >60 years with atrial fibrillation, recent MI, or peripheral vascular disease. Lactate >3 mmol/L has 90% sensitivity but only 40% specificity-normal lactate does not exclude early ischemia.
Imaging Characteristics: The Radiological Roadmap
| Diagnosis | Plain Film Findings | CT Findings | Sensitivity | Specificity | Gold Standard |
|---|---|---|---|---|---|
| Appendicitis | Nonspecific 90% | Fat stranding, appendix >6 mm | 95% | 94% | CT with IV contrast |
| Diverticulitis | Nonspecific 80% | Wall thickening >4 mm, pericolic fat | 98% | 95% | CT abdomen/pelvis |
| Perforated ulcer | Free air 75% | Pneumoperitoneum, oral contrast leak | 90% | 95% | CT with oral contrast |
| Small bowel obstruction | Air-fluid levels 80% | Transition point, caliber change | 90% | 85% | CT enterography |
| Mesenteric ischemia | Nonspecific 95% | Bowel wall thickening, pneumatosis | 85% | 92% | CT angiography |
| Volvulus | Coffee bean sign | Whirl sign, closed loop | 75% | 90% | CT abdomen/pelvis |
-
CT Abdomen/Pelvis with IV Contrast: 95% diagnostic workhorse
- Sensitivity >90% for most surgical pathology
- Oral contrast not routinely needed (delays care 2-4 hours)
- IV contrast essential for vascular assessment
- Contraindications: Cr >1.5 mg/dL (relative), allergy
- Radiation: 10-15 mSv (equivalent to 500 chest X-rays)
-
Ultrasound: 85% sensitivity for appendicitis (operator-dependent)
- First-line in children and pregnancy
- Appendix >6 mm diameter = abnormal
- Target sign: inflamed appendix in cross-section
- Free fluid suggests perforation
- Negative study does not exclude appendicitis
-
MRI: emerging role (90% sensitivity, no radiation)
- Pregnancy: safe alternative to CT
- IBD assessment: fistula mapping
- Rectal cancer: local staging
- Limitations: cost, availability, time (45-60 min)
💡 Master This: The "CT everything" approach is not appropriate. Use clinical scoring first: Alvarado ≥7 for appendicitis proceeds directly to surgery in many centers without imaging. CT is for equivocal cases (score 5-6) where diagnosis changes management. Avoid radiation in young patients when clinical diagnosis is clear.
Laboratory Discrimination
-
White Blood Cell Count: 75% sensitive, 60% specific
- <10,000/μL: does not exclude appendicitis (30% normal WBC)
- >15,000/μL: suggests complicated disease
- >20,000/μL: perforation or ischemia likely
- Left shift >75% neutrophils: bacterial infection
- Bandemia >10%: severe infection
-
C-Reactive Protein: 80% sensitive after 12 hours
- <10 mg/L: appendicitis unlikely after 12 hours
- >50 mg/L: complicated appendicitis or diverticulitis
- >150 mg/L: abscess or perforation probable
- Peaks at 24-48 hours (delayed marker)
-
Lactate: 90% sensitive for ischemia when >3 mmol/L
- >2 mmol/L: concerning in acute abdomen
- >4 mmol/L: ischemia until proven otherwise
- >6 mmol/L: mortality 50%, urgent exploration
- Serial measurements: rising = deterioration
-
Lipase: 95% sensitive for pancreatitis
- >3× upper limit: pancreatitis (but not surgical)
- Rule out non-surgical acute abdomen
- Can be elevated in bowel obstruction (2× normal)
⚠️ Warning: Never use laboratory values alone to exclude surgical pathology. 10-30% of appendicitis patients have normal WBC and normal CRP at presentation. Clinical assessment and imaging trump labs when discordant.
Connect these discrimination frameworks through treatment algorithms to optimize surgical timing and approach selection.
🏥 The Differential Matrix: Systematic Discrimination
🔍 Surgical Decision Architecture: Timing and Technique
Operative timing separates good outcomes from catastrophic complications. The decision matrix balances urgency (minutes to hours), emergency (hours to 24 hours), and elective (days to weeks) categories. Understanding physiological reserve and disease progression determines the optimal intervention window.
Urgency Classification Framework
-
Immediate Surgery (<1 hour): life-threatening conditions
- Free perforation with peritonitis
- Mesenteric ischemia with peritoneal signs
- Massive GI hemorrhage with shock (MAP <65 mmHg)
- Ruptured abdominal aortic aneurysm
- Mortality increases 15-20% per hour of delay
- Resuscitation concurrent with surgical prep
-
Urgent Surgery (1-6 hours): stabilize then operate
- Appendicitis with localized peritonitis
- Diverticulitis Hinchey III-IV
- Small bowel obstruction with strangulation signs
- Contained perforation with abscess
- Time for adequate resuscitation and imaging
-
Emergency Surgery (6-24 hours): optimized preparation
- Uncomplicated appendicitis
- Small bowel obstruction without ischemia
- Large bowel obstruction (if cecum >9 cm)
- Bleeding ulcer after failed endoscopic control
- Window for medical optimization and bowel prep
-
Elective Surgery (>24 hours to weeks): planned intervention
- Colorectal cancer without obstruction
- IBD after medical therapy failure
- Recurrent diverticulitis (>2 episodes)
- Gastric outlet obstruction (after decompression)
- Full preoperative workup and optimization
📌 Remember: "Resuscitate, Image, Operate" sequence for urgent cases. "Operate, Resuscitate, Image" for immediate cases (don't delay for CT when peritonitis is obvious). The decision to skip imaging requires senior surgeon judgment and clear peritoneal signs.
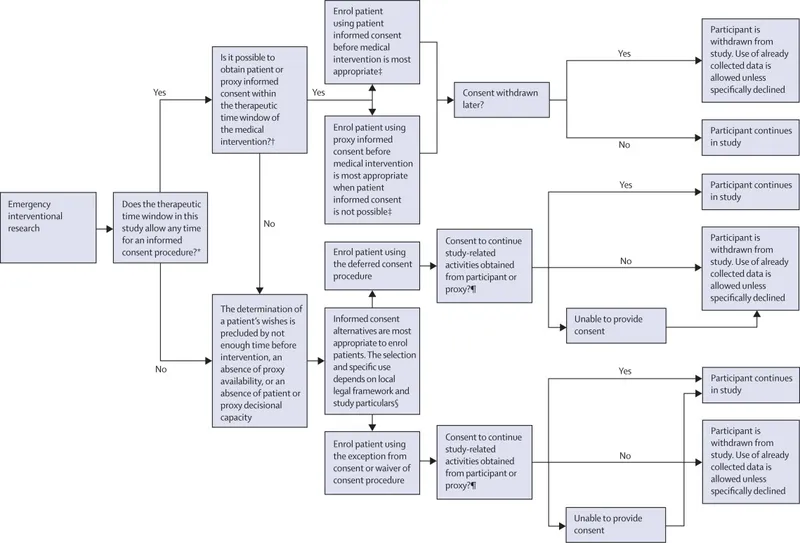
Operative Approach Selection
-
Open Laparotomy Indications: 40% of acute abdomen
- Hemodynamic instability requiring rapid control
- Diffuse peritonitis with unclear source
- Prior multiple abdominal surgeries (adhesions)
- Need for damage control surgery
- Surgeon comfort and experience
- Conversion rate from laparoscopy: 5-15%
-
Laparoscopic Approach Advantages: 60% feasible
- Diagnostic accuracy 95% for acute abdomen
- Shorter hospital stay (2-3 days vs. 5-7 days)
- Less postoperative pain (30-50% reduction)
- Faster return to normal activity (2 weeks vs. 4-6 weeks)
- Lower wound infection rate (5% vs. 15%)
- Comparable outcomes for appendicitis, cholecystitis
-
Damage Control Surgery Principles: <10% of cases
- Abbreviated laparotomy for physiological exhaustion
- Control hemorrhage and contamination only
- Temporary closure (vacuum-assisted or towel clip)
- ICU resuscitation for 24-48 hours
- Planned re-laparotomy for definitive repair
- Indications: pH <7.2, temperature <34°C, coagulopathy
Resection Principles by Organ
-
Appendectomy Technique: 95% complete excision
- Laparoscopic preferred in non-perforated (<24 hours)
- Open approach for perforated with abscess
- Mesoappendix division with energy device
- Base ligation with endoloop or stapler
- Stump inversion not routinely needed
- Drain placement only if abscess present
-
Colonic Resection Margins: oncologic vs. inflammatory
- Cancer: 5 cm margins, high vascular ligation
- Diverticulitis: resect to proximal rectum (avoid sigmoid remnant)
- Ischemia: resect to viable tissue (good bleeding, peristalsis)
- Crohn's: minimal margins (disease recurs regardless)
- Anastomosis: tension-free, well-perfused, >3 cm from tumor
-
Small Bowel Resection Considerations
- Preserve maximum length (need 100 cm for nutrition)
- Resect nonviable segments generously
- Ileocecal valve: preserve if possible (slows transit)
- Stricturoplasty for Crohn's (preserve length)
- Anastomosis: hand-sewn or stapled equivalent outcomes
| Procedure | Operative Time | Hospital Stay | Complication Rate | Mortality | Return to Work |
|---|---|---|---|---|---|
| Laparoscopic appendectomy | 45-60 min | 1-2 days | 5-10% | <0.5% | 1-2 weeks |
| Open appendectomy | 30-45 min | 2-3 days | 10-15% | <1% | 2-3 weeks |
| Sigmoid colectomy (lap) | 120-180 min | 3-5 days | 15-20% | ** |
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app




















