Thyroiditis Basics - Gland Under Siege
- Inflammation of thyroid gland; diverse causes (autoimmune, infectious, drug-induced).
- Key Presentations:
- Painful (e.g., Subacute Granulomatous, Acute Suppurative).
- Painless (e.g., Hashimoto's, Subacute Lymphocytic, Riedel's).
- Thyroid Function: Can cycle through thyrotoxicosis (preformed hormone release), hypothyroidism, then euthyroidism.
- ESR/CRP: Often ↑, especially in painful forms.
- Radioactive Iodine Uptake (RAIU): Typically ↓ due to glandular damage or TSH suppression.
⭐ In most forms of thyroiditis causing thyrotoxicosis, RAIU is characteristically low, distinguishing it from Graves' disease (where RAIU is high).
Hashimoto's - Autoimmune Havoc
- Most common cause of hypothyroidism in iodine-sufficient areas; an autoimmune disorder.
- Key Antibodies: Anti-Thyroid Peroxidase (Anti-TPO), Anti-Thyroglobulin (Anti-Tg).
- Pathology:
- Diffuse lymphocytic infiltration with germinal center formation.
- Hurthle cell (Askanazy cell) metaplasia: follicular cells become enlarged, with abundant eosinophilic, granular cytoplasm.
- Clinical Course:
- May present initially with transient hyperthyroidism (Hashitoxicosis).
- Progresses to hypothyroidism; goiter is typically firm, rubbery, and non-tender.
- Associated with other autoimmune diseases (e.g., Type 1 DM, pernicious anemia).
- Increased risk of B-cell non-Hodgkin lymphoma (MALToma) of the thyroid.
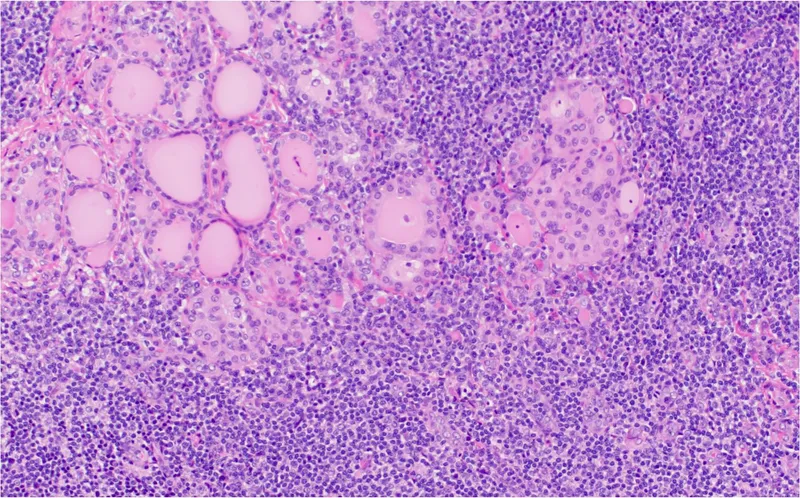
⭐ Hurthle cells (Askanazy cells), representing oxyphilic metaplasia of follicular epithelial cells, are a characteristic histological feature but not pathognomonic alone for Hashimoto's thyroiditis; they are also seen in other thyroid conditions like follicular neoplasms or goiter. However, in the context of diffuse lymphocytic infiltrate, they strongly suggest Hashimoto's disease and are frequently tested upon for their association with this condition in exams like NEET PG.
Subacute Squad - Painful & Quiet Phases
1. Subacute Granulomatous (De Quervain's) Thyroiditis:
- Painful, tender goiter; often post-viral (URI). Fever, malaise.
- Key: ↑ESR (often >50, classically >100 mm/hr). Pain radiates to jaw/ear.
- ↓RAIU (Radioactive Iodine Uptake). FNA: Granulomas, multinucleated giant cells.
- Tx: NSAIDs/Aspirin. Severe: Prednisone (e.g., 40mg/day).
2. Subacute Lymphocytic (Silent/Painless) Thyroiditis:
- Painless, non-tender, small/moderate goiter. Autoimmune etiology.
- Variant: Postpartum thyroiditis (occurs 1-12 months post-delivery).
- Anti-TPO Ab often (+). ↓RAIU (during thyrotoxic phase).
- Tx: Symptomatic (β-blockers for thyrotoxicosis); Levothyroxine if hypothyroid phase prolonged/symptomatic.
Triphasic Clinical Course (Both types):
⭐ De Quervain's thyroiditis: Key features are severe neck pain, fever, and markedly elevated ESR (often >100 mm/hr). RAIU is characteristically low during the thyrotoxic phase due to follicular cell damage and suppressed TSH an TSH-mediated iodine uptake, not due to primary hyperfunction of the gland itself like in Graves' disease.
Rarer Rebels - Woody & Fiery
- Riedel's Thyroiditis (Woody):
- Invasive fibrous tissue; "rock-hard", fixed, painless goiter.
- Compressive symptoms (dysphagia, dyspnea, hoarseness). Hypothyroidism common.
- Associated with IgG4-related disease / multifocal fibrosclerosis.
- Dx: Open biopsy (fibrosis). Rx: Corticosteroids, Tamoxifen, surgery for obstruction.
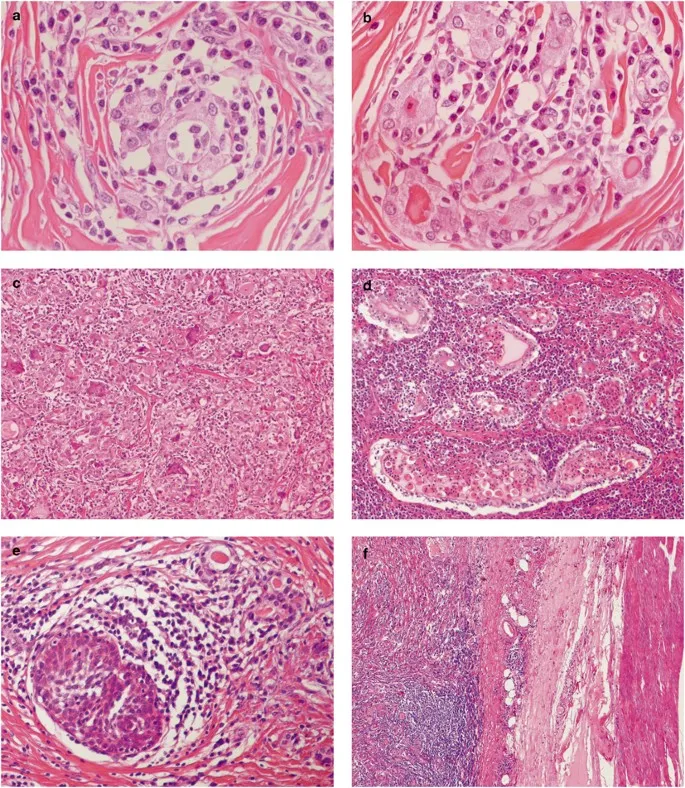
- Acute (Suppurative) Thyroiditis (Fiery):
- Bacterial infection (Staph aureus, Strep pyogenes); often via pyriform sinus fistula (children).
- Sudden severe neck pain, fever, chills; tender, erythematous, warm goiter.
- Usually euthyroid; ↑WBC, ↑ESR, ↑CRP.
- Dx: FNA (pus for culture). Rx: IV antibiotics, drainage of abscess.
⭐ Riedel's thyroiditis can mimic anaplastic carcinoma due to its hard, fixed nature and local invasion.
Thyroiditis Playbook - Unravel & Treat
- Key Differentiators: Pain, ESR, RAIU, Antibodies.
- General Tx: Symptomatic relief; specific therapy based on type.
| Type | Pain | ESR | RAIU | Key |
|---|---|---|---|---|
| Subacute | Yes | ↑↑↑ | ↓ | Viral prodrome |
| Hashimoto | No | N/↑ | Var | Anti-TPO |
| Silent/PP | No | N | ↓ | Transient |
| Riedel's | No | ↑ | ↓ | Fibrosis |
High‑Yield Points - ⚡ Biggest Takeaways
- De Quervain's thyroiditis: Painful, post-viral, ↑ESR, transient hyperthyroidism, low RAIU.
- Hashimoto's thyroiditis: Most common hypothyroidism cause, anti-TPO/Tg Ab, Hurthle cells, ↑lymphoma risk.
- Riedel's thyroiditis: "Woody" or rock-hard thyroid, painless, fibrotic, IgG4-related, compressive symptoms.
- Silent/Painless thyroiditis: Transient thyrotoxicosis then hypothyroidism, low RAIU; often postpartum.
- Acute (Suppurative) thyroiditis: Bacterial, painful, fever, ↑WBC; typically euthyroid.
- RAIU: Low in De Quervain's & Silent (thyrotoxic phase); contrasts Graves' (high).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

