Intro & Risks - Gland Gone Wild
- Most common endocrine malignancy; incidence ↑, especially in women.
- Major Types:
- Papillary (MC,
80-85%), Follicular (10-15%), Medullary (~3-5%), Anaplastic (<2%, worst prognosis). - 📌 Poor Fat Mice Always (Papillary, Follicular, Medullary, Anaplastic).
- Papillary (MC,
- Key Risk Factors:
- Radiation exposure: Childhood/adolescent head & neck (e.g., for lymphoma). Dose-dependent.
- Family Hx/Genetic Syndromes:
- Medullary: MEN2A/2B (RET proto-oncogene), Familial Medullary Thyroid Cancer (FMTC).
- Papillary: Familial Adenomatous Polyposis (FAP), Gardner syndrome, Cowden syndrome (PTEN gene).
- Iodine deficiency: ↑ risk for Follicular cancer.
- Chronic TSH stimulation (e.g., Hashimoto's thyroiditis - controversial for papillary; established link to thyroid lymphoma).
⭐ Thyroid cancer is the most common endocrine malignancy. Papillary thyroid cancer (PTC) is its most prevalent subtype, often with an excellent prognosis if detected early and managed appropriately.
Classification & Path - Rogues' Gallery
- Papillary Carcinoma (PTC): ~80-85%.
- Path: Orphan Annie eye nuclei (intranuclear inclusions, grooves), psammoma bodies.
- Spread: Lymphatic. Prognosis: Excellent.
- Variants: Follicular, Tall cell (worse prognosis).
⭐ Papillary thyroid cancer: most common type, psammoma bodies, excellent prognosis.
- Follicular Carcinoma (FTC): ~10-15%.
- Path: Capsular/vascular invasion essential for diagnosis (FNAC cannot diagnose).
- Spread: Hematogenous (bone, lung). 📌 "Follicular Follows Vessels."
- Hürthle cell variant: more aggressive.
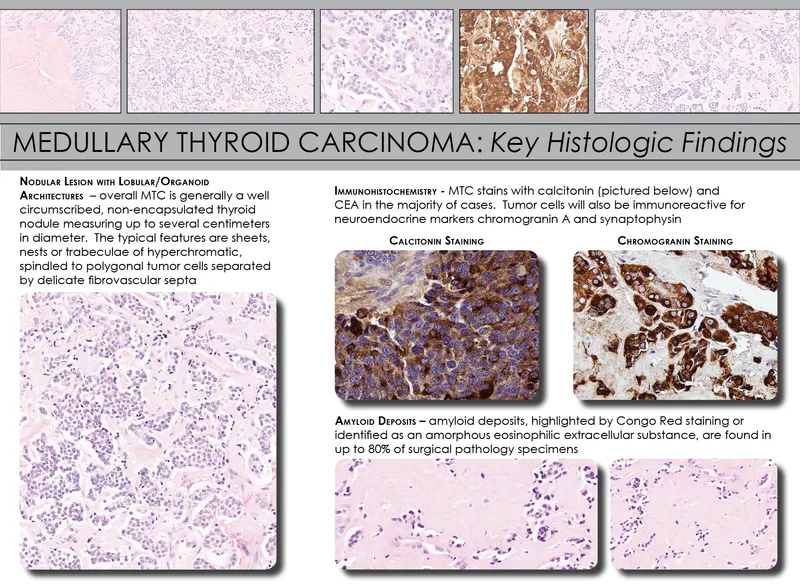
- Medullary Carcinoma (MTC): ~3-5%.
- Origin: Parafollicular C-cells. Secretes calcitonin.
- Path: Amyloid stroma (Congo red positive).
- Associations: MEN 2A/2B (RET mutation).
- Anaplastic Carcinoma (ATC): <1-2%.
- Undifferentiated, highly aggressive. Often elderly.
- Prognosis: Dismal, rapidly fatal.
- Lymphoma: Rare. Often arises in Hashimoto's thyroiditis.
Diagnosis & Staging - Detective Work
- Clinical Evaluation: Neck swelling, hoarseness, dysphagia. Family Hx (Medullary Ca).
- Thyroid Function Tests (TFTs): Usually euthyroid. TSH (suppressed in hot nodule, ↑ in Hashimoto's).
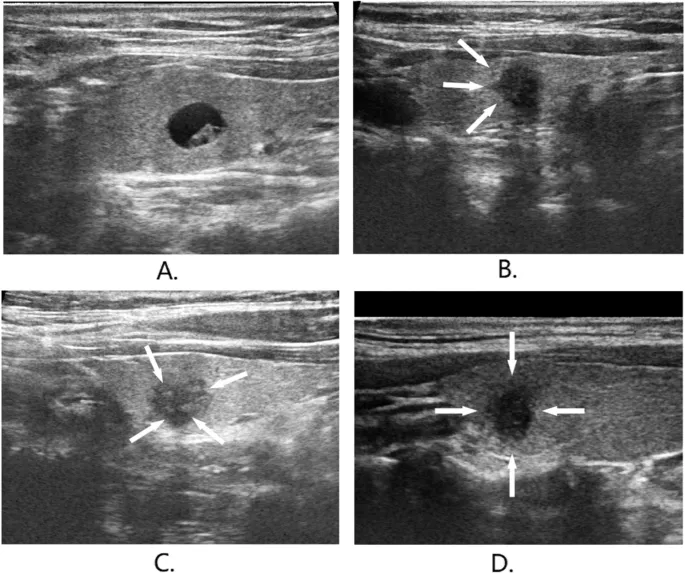
- Ultrasound (USG) Neck: Initial imaging. High-risk features: solid, hypoechoic, microcalcifications, irregular margins, taller-than-wide, extrathyroidal extension, suspicious lymph nodes.
- Fine Needle Aspiration Cytology (FNAC):
⭐ Fine Needle Aspiration Cytology (FNAC) is the gold standard investigation for a thyroid nodule.
- Bethesda System for Reporting Thyroid Cytopathology (BSRTC) guides management.
- Staging (AJCC 8th Ed): TNM. Age is key for Differentiated Thyroid Cancer (DTC).
- Papillary/Follicular: Age <55 yrs (Stage I/II). Age ≥55 yrs (Stage I-IV).
- Medullary: Calcitonin/CEA levels for prognosis & follow-up.
- Anaplastic: All Stage IV (universally poor prognosis).
Management & Follow-up - Battle Plan
- Primary Treatment
- Surgery: Total Thyroidectomy (TT) ± Central/Lateral Neck Dissection. Lobectomy for select low-risk (e.g., unifocal papillary microcarcinoma $<$1cm, no ETE/mets).
- Adjuvant Therapy (Risk-Stratified)
- Radioactive Iodine (RAI; I-131): Post-TT for remnant ablation/adjuvant. Dose: 30-150 mCi.
- TSH Suppression: Levothyroxine. Goal: TSH $<$0.1 mU/L (high-risk), 0.1-0.5 mU/L (low/intermediate-risk).
⭐ TSH suppression therapy is crucial post-thyroidectomy for differentiated thyroid cancer (DTC) to reduce recurrence.
- Advanced/Recurrent Disease
- EBRT: Unresectable, mets (bone, brain).
- TKIs (Lenvatinib, Sorafenib): RAI-refractory DTC.
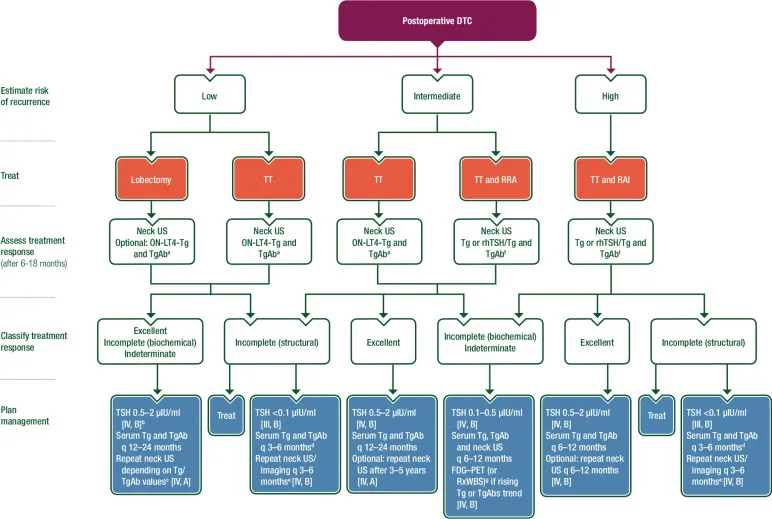
- Follow-up (Dynamic Risk Assessment)
- Serum Tg, Anti-TgAb, TSH (q 6-12 months).
- Neck Ultrasound (q 6-12 months).
- Further imaging (CT, MRI, PET) as indicated.
High‑Yield Points - ⚡ Biggest Takeaways
- Papillary Thyroid Carcinoma (PTC): Most common, excellent prognosis, psammoma bodies, lymphatic spread.
- Follicular Carcinoma: Hematogenous spread (bone, lungs); FNAC cannot diagnose invasion (histology needed).
- Medullary Carcinoma: From C-cells, produces calcitonin, linked to MEN2 (RET oncogene), amyloid stroma.
- Anaplastic Carcinoma: Elderly patients, worst prognosis, rapidly aggressive and often fatal.
- FNAC is the best initial diagnostic test for evaluating suspicious thyroid nodules.
- Differentiated cancers (PTC, Follicular): Treat with total thyroidectomy, radioiodine ablation, TSH suppression.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

