Pheo Basics - Adrenal Overdrive
- Rare catecholamine-secreting neuroendocrine tumor.
- Arises from chromaffin cells of the sympatho-adrenal system.
- Origin:
- Adrenal medulla (~80-85% of pheochromocytomas).
- Extra-adrenal paraganglia (~15-20%, termed paragangliomas); commonest is organ of Zuckerkandl.
- 📌 Rule of 10s (classic, but some figures vary with modern genetics):
- 10% bilateral adrenal
- 10% extra-adrenal
- 10% malignant
- 10% pediatric
- 10% familial (now known to be higher, up to 30-40% with genetic testing)
- 10% asymptomatic (often an incidentaloma)
⭐ Pheochromocytomas are a classic cause of surgically correctable hypertension.
Symptom Storm - Pressure Cooker
- Classic Triad (PHE): 📌
- Palpitations
- Headache (often throbbing)
- Episodic sweating (diaphoresis)
- Hypertension: Often paroxysmal (sudden attacks), can be sustained.
- Systolic BP can exceed 200-300 mmHg.
- Diastolic BP can exceed 130-180 mmHg.
- Other symptoms: Anxiety, tremors, pallor, chest/abdominal pain, nausea, vomiting, fatigue, weight loss.
- Triggers: Can be spontaneous or precipitated by stress, anesthesia, surgery, certain foods (tyramine-rich), or medications (e.g., beta-blockers without alpha-blockade, MAOIs).
⭐ Catecholamine Cardiomyopathy: Reversible left ventricular dysfunction can occur due to excessive catecholamine stimulation, mimicking dilated cardiomyopathy or Takotsubo cardiomyopathy (stress-induced).
Detective Work - Finding Pheo
- Biochemical Confirmation First: Crucial before imaging.
-
Key Diagnostic Tests:
Test Sensitivity Specificity Key Point Plasma free metanephrines (PFM) >95% ~85-89% Highest sensitivity; preferred test Urinary fractionated metanephrines ~90-97% ~90-95% Confirmatory; good alternative 24-hr Urinary VMA Lower (~60%) Lower (~90%) Less sensitive/specific -
Diagnostic Threshold: Levels >2-3 times upper limit of normal (ULN).
-
📌 Mnemonic: "Rule of 10s for Pheo, but test with Plasma Metanephrines".
-
- Imaging (Post-Biochemical Confirmation):
- Anatomical: CT abdomen/pelvis (initial); MRI (children, pregnancy, contrast allergy).
- Functional: ¹²³I-MIBG scintigraphy; ⁶⁸Ga-DOTATATE PET/CT (metastatic/extra-adrenal disease).
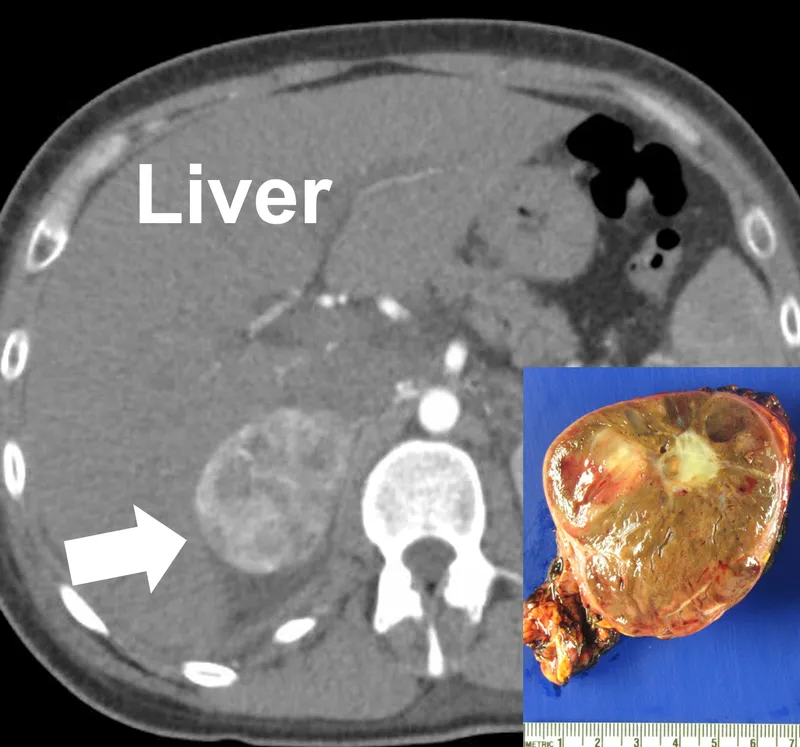
⭐ Plasma free metanephrines (PFM) are the most sensitive initial biochemical test for pheochromocytoma and paraganglioma.
Taming the Tumor - Surgical Gameplan
Pre-operative Goals: Achieve BP <130/80 mmHg (seated), SBP >90 mmHg (standing) & restore plasma volume.
- Surgical Resection: Definitive treatment, aiming for complete tumor removal.
- Approach: Laparoscopic adrenalectomy is gold standard. Open surgery for large (>6-8 cm), invasive, or multiple tumors.
- Intra-operative Care:
- Vigilant arterial BP monitoring is crucial.
- Manage hypertensive crises (e.g., IV nitroprusside, phentolamine).
- Treat hypotension post-adrenal vein ligation (aggressive fluids, vasopressors).
⭐ The "no-touch" isolation technique for the adrenal vein is crucial during surgery to minimize tumor manipulation and prevent massive catecholamine release.
Family Ties & Oddballs - Beyond Typical
| Syndrome | Gene | Key Features |
|---|---|---|
| MEN2A/B | RET | MTC; PTH hyperplasia (2A); Neuromas (2B) |
| VHL | VHL | Hemangioblastomas, RCC, pancreatic cysts |
| NF1 | NF1 | Neurofibromas, Café-au-lait spots, Lisch nodules |
| SDHx | SDHB/D | Paragangliomas; SDHB: ↑malignancy risk |
High‑Yield Points - ⚡ Biggest Takeaways
- Classic Triad: Episodic headache, sweating, tachycardia.
- Diagnosis: ↑ plasma free metanephrines or ↑ 24-hr urinary fractionated metanephrines & catecholamines.
- Pre-op: α-blockade (e.g., phenoxybenzamine) first, then β-blockade if needed (prevents crisis).
- Rule of 10s: 10% bilateral, extra-adrenal, malignant, pediatric, familial (some now higher).
- Most common extra-adrenal tumor site: Organ of Zuckerkandl.
- Key Associations: MEN 2A/2B, VHL, NF1.
- Treatment: Surgical resection after medical stabilization_._
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

