NETs Overview - The Hormone Rebels
- Definition: Heterogeneous neoplasms from neuroendocrine cells (historically APUDomas) within the Diffuse Neuroendocrine System (DNES).
- Key Feature: Can synthesize and secrete various hormones/amines, causing diverse syndromes (functional) or be silent (non-functional).
- Common Sites:
- Gastroenteropancreatic (GEP) tract (most common): Small intestine (ileum), rectum, pancreas, appendix.
- Lungs (bronchial carcinoids).
- WHO Classification (GEP-NETs): Graded by proliferation.
- NET G1: Mitoses <2/10 HPF & Ki-67 index ≤2%
- NET G2: Mitoses 2-20/10 HPF & Ki-67 index 3-20%
- NEC G3 (Carcinoma): Mitoses >20/10 HPF & Ki-67 index >20%

⭐ Small intestine (especially ileum) is the most common site for GEP-NETs., where they are often multifocal and associated with carcinoid syndrome if liver metastases are present
Symptoms & Diagnosis - Spotting the Signals
- Symptoms:
- Non-functioning: Often silent; vague pain, mass effect.
- Functioning: Hormone excess syndromes.
- Carcinoid: Flushing, diarrhea, bronchospasm. 📌 (Serotonin-mediated)
- Insulinoma: Hypoglycemia (Whipple's triad).
- Gastrinoma (ZES): Peptic ulcers, diarrhea.
- Diagnosis:
- Biochemical Markers:
- General: ↑Chromogranin A (CgA) - most sensitive. Neuron-Specific Enolase (NSE).
- Specific: Urine 5-HIAA (carcinoid); serum insulin, gastrin, glucagon.
- Imaging:
- Anatomical: CT, MRI, Endoscopic Ultrasound (EUS).
- Functional (Receptor-based): 68Ga-DOTATATE PET/CT (gold standard for GEP-NETs), Octreoscan (111In-pentetreotide SRS).
- Biochemical Markers:
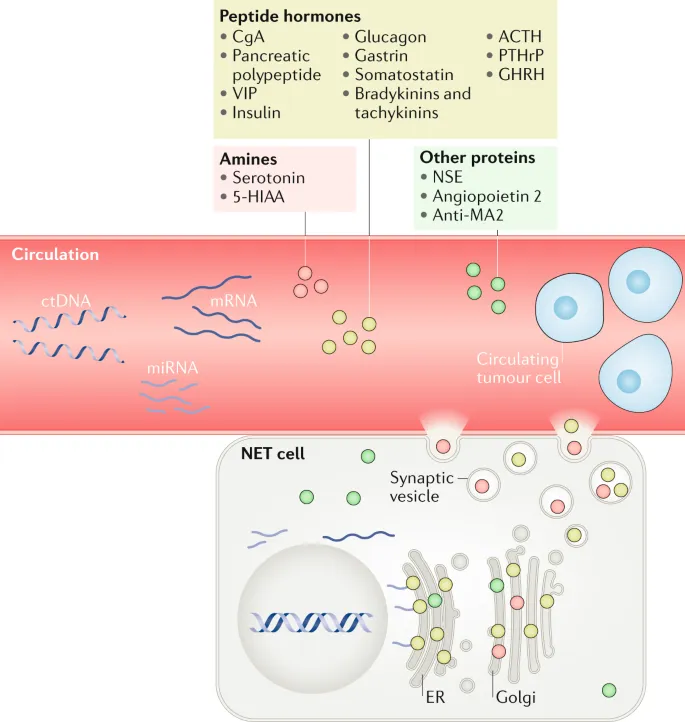
⭐ Carcinoid syndrome (flushing, diarrhea) typically manifests only after liver metastasis, as hepatic first-pass metabolism inactivates hormones from primary GI NETs.
Key Syndromes - The Hormone Havoc
| Syndrome | Hormone(s) | Key Symptoms | Diagnosis | MEN1 Assoc. |
|---|---|---|---|---|
| Insulinoma | Insulin | Whipple's triad (hypoglycemia, neuroglycopenia, glucose relief) | 72hr fast; ↑Insulin, ↑C-peptide, ↑Proinsulin with ↓glucose; CT/MRI/EUS | ~5-10% |
| Gastrinoma (ZES) | Gastrin | Peptic ulcers (multiple, refractory), diarrhea, GERD, abdominal pain | ↑Fasting gastrin (>1000 pg/mL + pH <2); Secretin stimulation test; SRS, EUS | ~20-25% |
| Carcinoid Syndrome | Serotonin, etc. | Flushing, diarrhea, bronchospasm, R-sided heart valve lesions (📌 FDR-Heart: Flushing, Diarrhea, R-Heart) | ↑24hr urinary 5-HIAA; ↑Chromogranin A; Octreotide scan (SRS) | Rare |
⭐ Carcinoid syndrome typically manifests only after liver metastases, as hormones from GI carcinoids are inactivated by the first-pass effect in the liver.
Treatment Strategies - Taming the Tumors
- Localized Disease: Surgical resection offers curative potential. Adjuvant therapy based on risk.
- Metastatic/Unresectable Well-Differentiated (WD-NETs):
- Somatostatin Analogs (SSAs): Octreotide, Lanreotide for carcinoid syndrome control & antiproliferative effects (PROMID, CLARINET studies).
- Peptide Receptor Radionuclide Therapy (PRRT): $^{177}$Lu-DOTATATE for SSTR+ tumors after SSA progression (NETTER-1 trial).
- Targeted Therapy: Everolimus (mTORi), Sunitinib (TKI) for progressive pancreatic NETs (pNETs)/GI-NETs.
- Poorly Differentiated Neuroendocrine Carcinomas (PD-NECs) / High-Grade: Systemic chemotherapy (e.g., Cisplatin + Etoposide) is standard.
⭐ Octreotide/Lanreotide (SSAs) are first-line for symptomatic and antiproliferative therapy in unresectable/metastatic low-intermediate grade GEP-NETs.
High‑Yield Points - ⚡ Biggest Takeaways
- Carcinoid syndrome (flushing, diarrhea) often indicates liver metastases from midgut NETs.
- Chromogranin A (CgA) is the most sensitive general marker for NETs.
- Octreotide scan (SRS) is crucial for localization and staging.
- MEN 1 association: Pancreatic NETs (gastrinoma, insulinoma), parathyroid, pituitary.
- Insulinomas present with Whipple's triad; surgical enucleation is often curative.
- Gastrinomas (ZES) cause severe peptic ulcers; locate in Passaro's triangle.
- Surgical resection is the mainstay for curative intent in localized disease_
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

