Intro to MEN - Genetic Dominoes
- 📌 MEN: Multiple Endocrine Neoplasia.
- Group of disorders causing tumors in multiple endocrine glands; typically Autosomal Dominant inheritance.
- Key genes involved: MEN1 (encoding menin), RET (proto-oncogene).
- Characterized by high penetrance but variable expressivity among affected individuals.
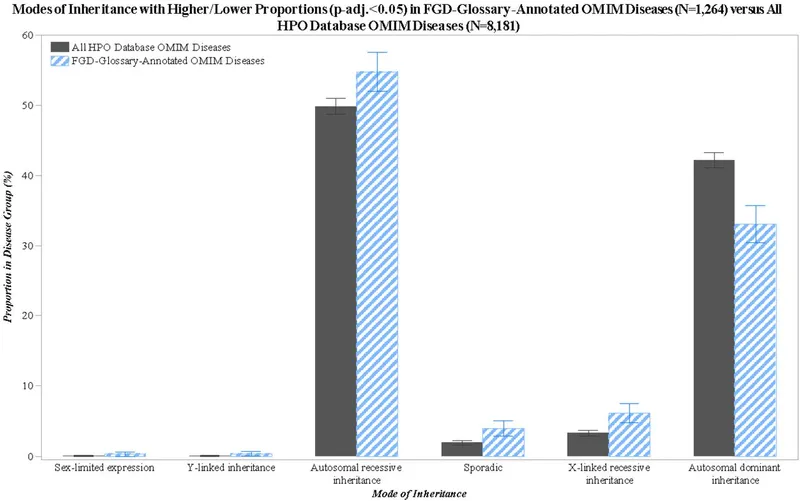
⭐ Most MEN syndromes are inherited in an autosomal dominant fashion, affecting multiple glands over a patient's lifetime.
MEN 1 (Wermer's) - 3 'P' Party
Autosomal dominant, MEN1 gene mutation (encodes menin). 📌 Mnemonic: 3 'P's.
| Affected 'P' Organ | Tumors & Features | Frequency (%) |
|---|---|---|
| Parathyroid | Hyperplasia/Adenoma → Primary Hyperparathyroidism (↑Ca²⁺, "stones, bones, groans"). Most common & earliest. | >90 |
| Pancreas (NETs) | Gastrinoma (ZES: ulcers, diarrhea), Insulinoma (hypoglycemia), VIPoma, Glucagonoma. | 30-70 |
| Pituitary | Prolactinoma (most common: galactorrhea, amenorrhea), GH-oma (acromegaly), ACTH-oma (Cushing's disease). | 10-60 |

⭐ Primary hyperparathyroidism: most common (>90%) & earliest MEN1 sign, often by age 20-25 years.
MEN 2A (Sipple's) - Thyroid's Tough Trio
- Genetic Basis: Autosomal dominant, RET proto-oncogene mutation (gain-of-function).
- Components (📌 Mnemonic: MPP):
- Medullary Thyroid Carcinoma (MTC): ~100% penetrance. Calcitonin is tumor marker.
- Pheochromocytoma: ~50%, often bilateral. Screen with plasma/urine metanephrines.
- Parathyroid Hyperplasia/Adenoma: ~20-30%, leading to hyperparathyroidism.

- Screening & Management Flowchart:
⭐ Prophylactic thyroidectomy is recommended in childhood (often before age 5 years, depending on specific RET codon mutation) for individuals with RET mutations associated with MEN2A to prevent MTC development or treat it at its earliest stage. Consider screening for pheochromocytoma before any surgery due to anesthesia risks.
MEN 2B - MTC's Mean Cousin
- Autosomal Dominant, RET proto-oncogene (codon 918).
- 📌 MPM: Medullary thyroid ca, Pheochromocytoma, Mucosal neuromas/Marfanoid habitus.
- NO hyperparathyroidism (key difference from MEN 2A).
| Feature | MEN 2B | MEN 2A (Comparison) |
|---|---|---|
| MTC | Aggressive, early onset. Prophylactic thyroidectomy by 1 year. | Less aggressive (by 5-6 yrs). |
| Pheochromocytoma | Yes (often bilateral) | Yes (often bilateral) |
| Distinct | Mucosal neuromas (lips, tongue), Marfanoid habitus, Intestinal ganglioneuromatosis. | (Cutaneous Lichen Amyloidosis, Hirschsprung's) |

MEN Dx & Mx - Code MEN Unravelled
- Diagnosis:
- Clinical suspicion (family history, specific tumor clusters).
- Biochemical screening: ↑Hormone levels (e.g., Ca, PTH, gastrin, calcitonin, metanephrines).
- Genetic testing: MEN1 gene, RET proto-oncogene analysis.
- Imaging: CT, MRI, USG, MIBG/DOTA-PET to localize tumors.
- Management:
- Surgical: Total thyroidectomy (MTC), parathyroidectomy, adrenalectomy (pheochromocytoma: pre-op α then β blockade CRITICAL).
- Lifelong surveillance protocols tailored to syndrome/gene.
⭐ Genetic testing is crucial for identifying at-risk family members and guiding prophylactic interventions.
High‑Yield Points - ⚡ Biggest Takeaways
- MEN 1 (Wermer's syndrome): 3 P's - Parathyroid (most common), Pancreatic (e.g., gastrinoma), Pituitary. MEN1 gene.
- MEN 2A (Sipple's syndrome): Medullary Thyroid Carcinoma (MTC), Pheochromocytoma, Parathyroid hyperplasia. RET proto-oncogene.
- MEN 2B: MTC (aggressive), Pheochromocytoma, Mucosal neuromas/Marfanoid habitus. RET proto-oncogene (distinct mutation).
- MTC is a universal feature of MEN2 syndromes; prophylactic thyroidectomy is often indicated.
- Primary Hyperparathyroidism is the earliest and most frequent manifestation of MEN1.
- Pheochromocytomas in MEN syndromes are frequently bilateral and can be extra-adrenal.
- Genetic screening for MEN1/RET mutations in affected individuals and at-risk family members is crucial for early detection and management.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

