Intro to IOM in Endocrine Surgery - Surgical Spyglass
- Definition: Real-time physiological assessment of nerve and gland function during endocrine surgery. Acts as a "Surgical Spyglass", offering crucial intraoperative insights.
- Primary Goals:
- Early identification of critical structures (e.g., recurrent laryngeal nerve (RLN), parathyroid glands).
- Continuous assessment of their functional integrity.
- Guide precise surgical dissection.
- Minimize risk of iatrogenic injury.
- Key Benefits:
- Reduced rates of permanent complications (e.g., vocal cord palsy, hypoparathyroidism).
- Improved preservation of endocrine function.
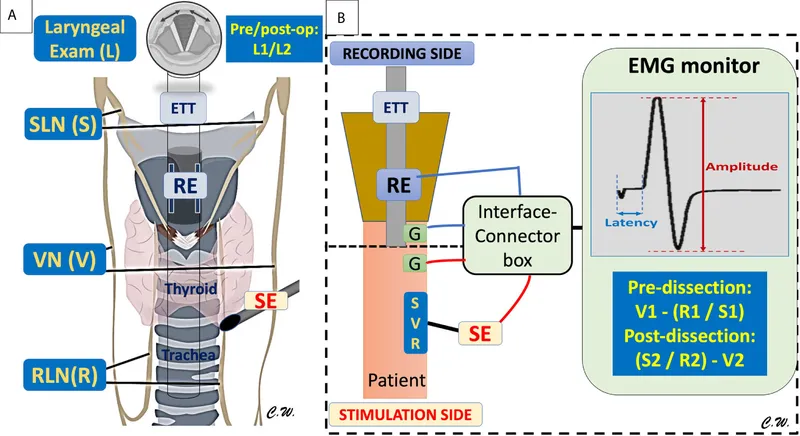
⭐ IOM, especially for RLN, is crucial in thyroid surgery to prevent voice changes and assess nerve integrity before closure.
IOM in Thyroid & Parathyroid Surgery - Neck Check Tech
- Nerve Integrity Monitoring (NIM): Safeguards RLN & EBSLN during surgery.
- EMG-based: Stimulates nerve, records vocal cord (thyroarytenoid) muscle response.
- Types: Intermittent (probe) vs. Continuous (vagus/RLN electrode).
- Signal: Amplitude (µV), Latency (ms).
- ⚠️ Loss of Signal (LOS): Amplitude < 100 µV or >50% drop from baseline.
- Aids nerve ID, predicts function, guides safe dissection.
- 📌 Nerves In Mind for RLN/EBSLN.
- Parathyroid Gland ID & Viability: Key to prevent post-op hypocalcemia.
- Autofluorescence (NIRAF):
- Parathyroids uniquely fluoresce (e.g., at approx. 820-830 nm) with NIR light (e.g., approx. 785 nm excitation).
- Helps distinguish from thyroid, fat, lymph nodes.
- 📌 Parathyroids Are Fluorescent.
- ICG Angiography: IV dye assesses parathyroid vascularity, predicting gland viability.
- Autofluorescence (NIRAF):
- Intraoperative PTH (ioPTH): For primary hyperparathyroidism (PHPT).
- Rapid PTH assay: Baseline, pre-excision, post-excision (5, 10, 20 min) samples.
- Confirms complete removal of hyperfunctioning parathyroid tissue.
⭐ Miami Criterion: >50% PTH drop from highest baseline/pre-excision at 10 min post-final gland excision predicts PHPT cure.
 oka
oka
IOM for Adrenal & Pancreatic Tumors - Hormone Hunt How-To
- Adrenal Tumors:
- Pheochromocytoma/PGL:
- Monitor: Arterial BP (A-line), CVP.
- Goal: Manage hypertensive crisis (tumor handling) & hypotension (post-vein ligation).
- Consider: Glucose (post-resection hypoglycemia).
- Conn's (Aldosteronoma):
- Monitor: Serum K⁺, BP.
- Goal: Confirm resection (↓Aldo, K⁺ normalization post-op).
- Cushing's (Cortisol Adenoma):
- Monitor: BP, glucose.
- Goal: Expect ↓cortisol post-op (guides steroid replacement).
- Pheochromocytoma/PGL:
- Pancreatic NETs (PNETs):
- Insulinoma:
- Monitor: Frequent intraoperative glucose (IOGM) q 5-15 min.
- Goal: Glucose ↑ by >25-50 mg/dL or to euglycemia within 30-60 min post-resection.
- 📌 "Sweet Success for Insulinoma = Sugar Soars!"
- No rise? Suspect residual/multicentric disease.
⭐ Rapid fall in intraoperative insulin levels (if assay available) is a more direct indicator of successful insulinoma resection.
- Gastrinoma:
- Goal: Confirm resection by ↓gastrin (usually post-op).
- Consider: Intraop secretin test (if available).
- Insulinoma:
Advanced Techniques & Limitations - Future Focus Finds
- Advanced:
- AI in IOM interpretation, Ultrafast PTH assays.
- NIR autofluorescence (parathyroid ID).
- ML for risk prediction.
- Limitations:
- Cost, access, data complexity.
- Standardization needs.
- Future Focus:
- Non-invasive sensors, multi-analyte platforms.
- Personalized IOM strategies.
⭐ Continuous intraoperative PTH (C-PTH) monitoring is crucial for assessing complete resection in primary hyperparathyroidism, aiming for a >50% drop from baseline.
High‑Yield Points - ⚡ Biggest Takeaways
- IOPTH in parathyroidectomy: >50% drop from baseline indicates successful resection.
- RLN monitoring: Standard for thyroid & parathyroid surgery; prevents vocal cord palsy.
- Insulinoma resection: Requires intraoperative glucose monitoring (CGM or frequent BG).
- Pheochromocytoma surgery: Prioritizes hemodynamic stability over intraop catecholamine levels.
- Frozen section: Crucial for confirming malignancy & identifying parathyroid tissue.
- Methylene blue: Aids parathyroid identification; may interfere with IOPTH assays.
- Intraoperative cortisol: Guides resection in Cushing's & cortisol-producing adrenal tumors.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

