Graves': Pathophysiology - Antibody Mayhem
- Autoimmune: Type II hypersensitivity.
- Key Antibody: TSH Receptor Antibody (TRAb).
- Primarily Thyroid Stimulating Immunoglobulins (TSI).
- Mimics TSH, activates TSH receptor (TSHR).
- Mechanism:
- TRAb binds TSHR → ↑ intracellular cAMP.
- Stimulates thyroid hormone (T3, T4) synthesis & secretion.
- Promotes thyroid follicular cell growth/proliferation → goiter.
- Feedback Loop: ↑ T3/T4 → ↓ pituitary TSH.
- Genetic Links: HLA-DR3, CTLA-4.
- Triggers: Stress, infection, smoking, iodine.
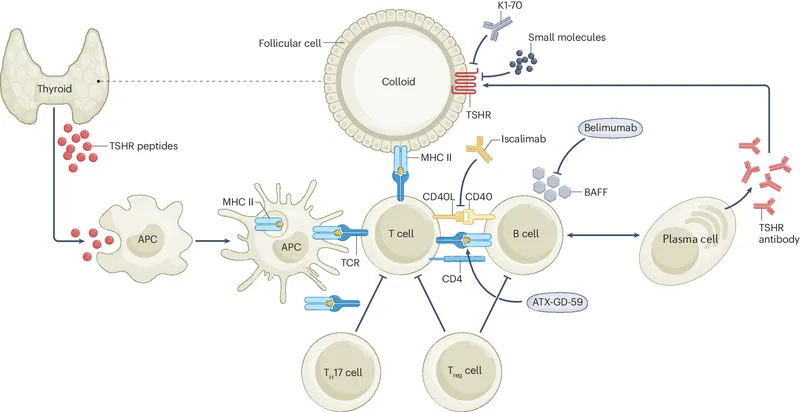
⭐ TRAb can be stimulating, blocking, or neutral. In Graves', stimulating antibodies (TSI) predominate, causing hyperthyroidism.
Graves': Clinical Features - Eye‑Popping Signs
- General Hyperthyroidism: Weight loss, palpitations, heat intolerance, tremor.
- Graves' Ophthalmopathy (GO) / Thyroid Eye Disease (TED): Specific autoimmune manifestation.
- Proptosis (exophthalmos): Forward protrusion of eyeballs.
- Lid retraction (Dalrymple's sign): Causes a "staring" appearance.
- Lid lag (von Graefe's sign): Upper eyelid lags behind globe on downward gaze.
- Diplopia (double vision), periorbital edema, chemosis (conjunctival edema).
- Optic neuropathy (in severe cases): Can lead to vision loss.
- Specific Extrathyroidal Manifestations:
- Pretibial myxedema (Graves' dermopathy): Localized, infiltrative dermopathy; waxy, discolored induration of the skin ("orange peel" or peau d'orange appearance), typically on anterior shins.
- Thyroid acropachy: Rare; digital clubbing, soft tissue swelling of hands and feet, periosteal new bone formation.
- Goiter: Diffuse, usually firm, and may have a vascular bruit.
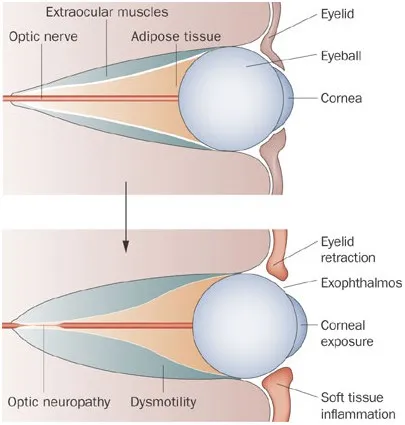
⭐ Lid retraction is the most common and often earliest sign of Graves' ophthalmopathy; it can occur even when the patient is euthyroid or hypothyroid after treatment for Graves' hyperthyroidism.
Graves': Diagnosis - Spotting the Storm
- Initial Tests:
- ↓ TSH (often < 0.01 mIU/L)
- ↑ Free T4 (FT4) & ↑ Free T3 (FT3)
- Confirmatory Test:
- TSH Receptor Antibodies (TRAb): Positive (diagnostic)
- Thyroid Stimulating Immunoglobulins (TSI) is a type of TRAb.
- TSH Receptor Antibodies (TRAb): Positive (diagnostic)
- Radioactive Iodine Uptake (RAIU) Scan:
- Shows diffuse, increased uptake.
- Helps differentiate from other hyperthyroid causes.
⭐ TRAb positivity is the most specific laboratory finding for Graves' disease, present in >90% of cases.
Graves': Management - Scalpel & Solutions
Medical Options (Context):
- Antithyroid Drugs (ATDs): Methimazole (MMI preferred), PTU (1st trimester pregnancy/thyroid storm).
- Radioiodine (RAI): CI: pregnancy, severe GO, malignancy suspicion.
- Beta-blockers: Symptomatic control.
Surgical Indications:
- Large goiter (>80g), compressive symptoms.
- Malignancy suspected/confirmed.
- ATD failure/intolerance; RAI contraindicated/refused.
- Moderate-severe active Graves' Orbitopathy (GO).
- Pregnancy planned <6 months / Rapid biochemical control needed.
Pre-operative Preparation:
- Achieve euthyroidism: ATDs.
- Lugol’s Iodine or SSKI: 7-14 days pre-op (↓ vascularity). 📌 "Lugol's Lugs down vascularity".
- Beta-blockers for symptom control.
Surgical Procedures:
- Total Thyroidectomy (TT): Preferred, lowest recurrence.
- Near-Total Thyroidectomy (NTT): Small remnant.
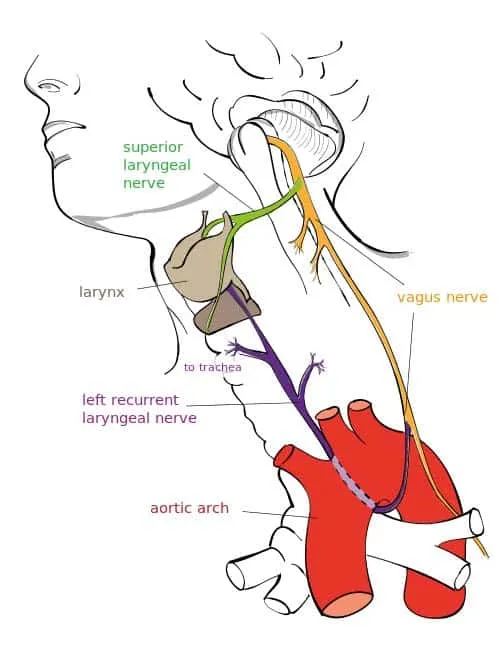
Key Complications:
- RLN injury: Hoarseness.
- Hypoparathyroidism: Hypocalcemia.
- EBSLN injury: Voice fatigue, ↓ high pitch.
- Hemorrhage, Hematoma.
⭐ > Total thyroidectomy is preferred for Graves': lowest recurrence, good safety with experience.
High‑Yield Points - ⚡ Biggest Takeaways
- Graves' disease: Autoimmune; TSH receptor antibodies (TRAb) cause hyperthyroidism, the most common etiology.
- Specific signs: Exophthalmos, pretibial myxedema, thyroid acropachy, plus diffuse goiter.
- Diagnosis: ↓TSH, ↑FT4/FT3, +TRAb; diffuse ↑Radioiodine Uptake (RAIU).
- Surgery: Total/Near-total thyroidectomy for large goiter, ophthalmopathy, or failed medical/RAI therapy.
- Pre-op: Euthyroidism with antithyroid drugs, then Lugol’s iodine to decrease gland vascularity.
- Major risks: Recurrent laryngeal nerve injury (hoarseness), hypoparathyroidism (hypocalcemia).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

