Adrenal Cortex Anatomy & Tumor Intro - Gland Overview
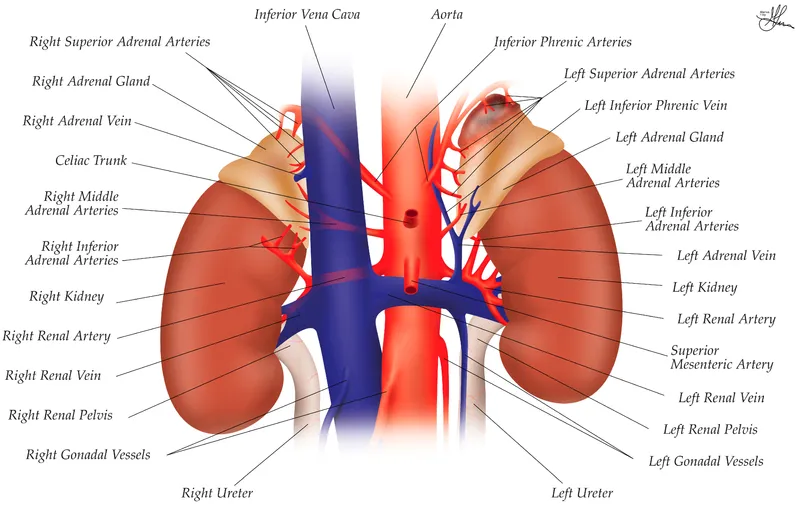
- Location: Bilateral, retroperitoneal, superomedial to kidneys.
- Arterial Supply: Superior, middle, & inferior adrenal arteries.
- Venous Drainage:
⭐ Left adrenal vein → left renal vein; Right adrenal vein → Inferior Vena Cava (IVC).
- Cortex Layers & Hormones (Outer to Inner): 📌 GFR Mnemonic
- Zona Glomerulosa: Mineralocorticoids (Aldosterone) → Salt
- Zona Fasciculata: Glucocorticoids (Cortisol) → Sugar
- Zona Reticularis: Androgens (DHEA) → Sex
- Adrenal Tumors Overview:
- Benign (e.g., adenoma) vs. Malignant (e.g., carcinoma).
- Functional (hormone-secreting) vs. Non-functional.
Functional Tumors (Cushing's, Conn's) - Hormone Havoc
Adrenal cortex overproduction: Cortisol (Cushing's) or Aldosterone (Conn's).
| Syndrome | Key Features | Screening Tests | Confirmatory Tests |
|---|---|---|---|
| Cushing's | Central obesity, moon facies, purple striae, HTN, hyperglycemia, weakness | LDDST (1mg): Cortisol >1.8 µg/dL; ↑24hr UFC; ↑Late-night salivary cortisol | HDDST (8mg); CRH stimulation test |
| Conn's | HTN (resistant), hypokalemia (not always), metabolic alkalosis, fatigue | ARR >20-30 (PAC/PRA); PAC >15 ng/dL; Suppressed PRA | Saline infusion; Oral Na+ load; Fludrocortisone supp. |
| 📌 Conn's: Think CONNecting HTN and Low K+ (Potassium). |
Diagnostic Algorithm (Conn's Syndrome):
⭐ Most common cause of endogenous Cushing's syndrome is Cushing's disease (pituitary adenoma), not primary adrenal tumors.
Management: Unilateral adenoma: Surgery. Bilateral hyperplasia/non-surgical: Medical (e.g., spironolactone for Conn's, ketoconazole for Cushing's).
Adrenocortical Carcinoma (ACC) - Malignant Mayhem
- Rare, aggressive; often >4-6 cm. Bimodal age: <5 yrs, 40s-50s.
- Presentation:
- Functional (~60%): Cushing's, virilization.
- Non-functional (~40%): Abd pain/mass.
- Diagnosis:
- CT/MRI: Large (>4-6 cm), irregular, heterogeneous, necrosis, calcification, invasion; >10 HU (non-contrast).
- Weiss Score: Histopathology; ≥3 criteria (mitoses, necrosis, invasion) = ACC.
- Staging: ENSAT System.
ENSAT Stage Description Stage I Tumor ≤5 cm, confined to adrenal Stage II Tumor >5 cm, confined to adrenal Stage III Local invasion (nodes, vein, adjacent organs) Stage IV Distant metastases - Management:
- Surgery: Radical adrenalectomy (local).
- Adjuvant: Mitotane (high risk).
- Metastatic: Mitotane, chemo.
- Prognosis: Poor; 5-yr survival 15-40%.
⭐ Mitotane is an adrenolytic agent used as adjuvant therapy in ACC and for metastatic disease.
Adrenal Incidentalomas - Surprise Masses
- Adrenal mass >1 cm discovered incidentally. Prevalence: ~5%.
- Essential Workup:
- Exclude functionality:
- Pheochromocytoma: Plasma free metanephrines or 24-hr urinary metanephrines/catecholamines.
- Cushing's syndrome: 1mg Dexamethasone Suppression Test (DST); overnight or low-dose.
- Primary aldosteronism (if hypertensive/hypokalemic): Aldosterone-Renin Ratio (ARR).
- Assess malignant potential (Non-Contrast CT):
- Benign features: Size <4 cm, smooth margins, homogenous, Hounsfield Units (HU) ≤10.
- Suspicious/Malignant: Size >4-6 cm, irregular, heterogeneous, HU >10, growth on follow-up.
- Exclude functionality:
- Management Algorithm:
⭐ Majority (70-80%) of adrenal incidentalomas are benign, non-hypersecreting adenomas.
High‑Yield Points - ⚡ Biggest Takeaways
- Conn's syndrome (primary hyperaldosteronism): adenoma causing hypertension, hypokalemia. ↑Aldo:Renin ratio.
- Cushing's syndrome (cortisol excess): adenoma/carcinoma causing central obesity, striae. Dexamethasone suppression test.
- Adrenocortical carcinoma (ACC): Aggressive, often functional, typically >6 cm. Weiss criteria for malignancy.
- Incidentalomas: Require hormonal workup. Resect if functional, malignant features, or >4-6 cm.
- Laparoscopic adrenalectomy: Standard for most benign functional tumors and smaller ACCs (<6cm).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

