IBD Overview - Fiery Bowel Blues
- Chronic, relapsing idiopathic inflammation of GIT.
- Two main types: Ulcerative Colitis (UC) & Crohn's Disease (CD).
- Epidemiology:
- Peak incidence: 15-30 years & 50-80 years (bimodal).
- Slight female predominance.
- Higher in developed nations.
- Risk factors:
- Genetics (e.g., NOD2/CARD15 for CD).
- Smoking (Worsens CD, Protects UC 📌).
- Diet (Western diet), NSAIDs.
- Altered gut microbiota.
⭐ Extraintestinal manifestations (EIMs) are common, occurring in up to 50% of IBD patients; arthritis is the most frequent EIM_._
Crohn's vs UC - The Great Divide
| Feature | Crohn's Disease (CD) | Ulcerative Colitis (UC) |
|---|---|---|
| Location | Mouth to anus; Skip lesions; Terminal ileum common | Rectum (always), continuous proximal spread; Colon only |
| Pathology | Transmural; Non-caseating granulomas (50-60%); Cobblestones, Creeping fat | Mucosal/Submucosal; Crypt abscesses, Pseudopolyps |
| Complications | Fistulae, Strictures, Abscesses; Perianal disease | Toxic megacolon, Hemorrhage; ↑ CRC risk (pancolitis) |
| Smoking | Worsens CD | Protective for UC |
⭐ Extraintestinal manifestations (EIMs) are common in IBD. Primary Sclerosing Cholangitis (PSC), a significant EIM, has a strong association with Ulcerative Colitis (approx. 70% of PSC patients have UC).
📌 Mnemonic:
- CD: "GRANny skips on COBBLESTONES from GUM to BUM, but SMOKING makes her FISTulae WORSE."
- UC: "ULCERS in the COLON are CONTINUOUS from the RECTUM, SMOKING is PROTECTIVE, but watch for CANCER."
Clinical & Diagnosis - Spotting the Signs
- Common Symptoms:
- Ulcerative Colitis (UC): Bloody diarrhea (hallmark), tenesmus, urgency, LLQ abdominal pain. Systemic symptoms less prominent.
- Crohn's Disease (CD): Abdominal pain (RLQ, colicky), weight loss, fatigue, diarrhea (often non-bloody). Perianal disease common.
- Key Extraintestinal Manifestations (EIMs): (~25-40% IBD patients) 📌 A PIE SAC
- Arthritis (peripheral/axial), Aphthous stomatitis
- Pyoderma gangrenosum
- Iritis/Uveitis
- Erythema nodosum
- Sclerosing cholangitis (PSC - UC, ↑cancer risk)
- Clubbing, Cholelithiasis (CD - ileal)
- Diagnostic Approach:
- Labs: CBC (anemia), ↑ESR/CRP, fecal calprotectin. p-ANCA (UC ~60%), ASCA (CD ~60%).
- Endoscopy + Biopsy (Definitive):
- UC: Continuous inflammation (rectum proximally), friability, pseudopolyps. Biopsy: cryptitis, crypt abscesses.
- CD: Skip lesions, aphthous/linear ulcers, cobblestoning, transmural. Biopsy: non-caseating granulomas (pathognomonic, ~30-50%).
- Imaging (CT/MR Enterography): Small bowel, transmural extent, complications (strictures, fistulae, abscesses).
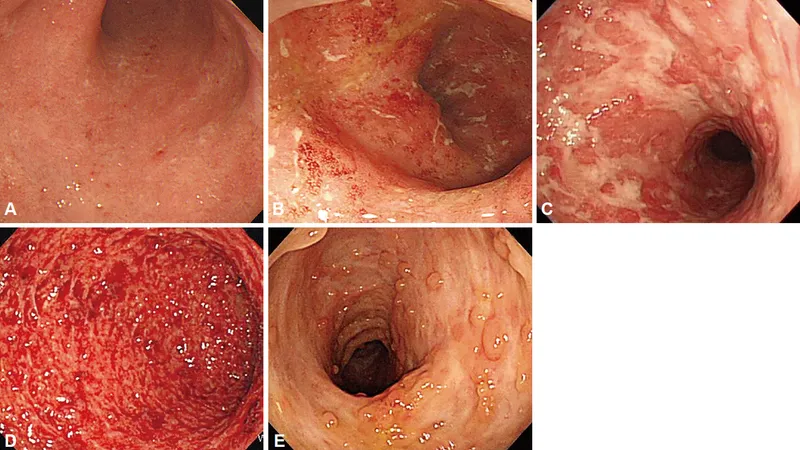
⭐ While crypt abscesses are characteristic of UC, they can also be seen in severe CD; non-caseating granulomas are specific to CD but only found in ~30-50% of biopsies.
Management - Taming the Flames
- Medical Therapy (Step-Up):
- Mild: 5-ASA (Mesalamine, Sulfasalazine) for UC; Budesonide for ileocolonic CD.
- Moderate Flares: Systemic Corticosteroids (Prednisolone $~1mg/kg$, max 40-60mg), taper on remission.
- Maintenance/Steroid-Sparing: Immunomodulators (Azathioprine, 6-MP, MTX). Monitor side effects.
- Severe/Refractory: Biologics (📌AIVU: Adalimumab, Infliximab, Vedolizumab, Ustekinumab).
⭐ Infliximab requires latent TB screening (reactivation risk).
- Surgical Therapy:
- Ulcerative Colitis (UC):
- Indications: Refractory, dysplasia/cancer, toxic megacolon ($>6cm$ dilation + toxicity), perforation, hemorrhage.
- Procedure: Total Proctocolectomy with IPAA (curative).
- Crohn's Disease (CD):
- Indications: Complications (strictures, fistulas, abscesses, obstruction), refractory disease.
- Procedures: Conservative resection, stricturoplasty. Not curative.
- Ulcerative Colitis (UC):
High‑Yield Points - ⚡ Biggest Takeaways
- Crohn's Disease: Characterized by transmural inflammation, skip lesions, fistulas, and strictures; smoking is a significant risk factor.
- Ulcerative Colitis: Features continuous mucosal inflammation typically starting in the rectum, with risk of toxic megacolon; smoking is paradoxically protective.
- Extraintestinal manifestations like arthritis, uveitis, and skin lesions are common in both.
- Surgical indications for Crohn's: Primarily for complications (e.g., stricture, fistula, abscess); bowel conservation (e.g., strictureplasty) is paramount.
- Surgical indications for UC: Includes medically refractory disease, dysplasia/cancer, or acute severe colitis; total proctocolectomy with IPAA is curative.
- Both IBD types carry an increased colorectal cancer risk, necessitating regular surveillance.
- Key serological markers: p-ANCA often positive in UC, ASCA often positive in Crohn's Disease.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

