Hemorrhoids 101 - Piles Primer
- Definition: Symptomatic, engorged vascular cushions in the anal canal.
- Anal Cushions: Normal submucosal structures (left lateral, right anterior, right posterior). Contain AV shunts.
- Types (based on relation to Dentate Line):
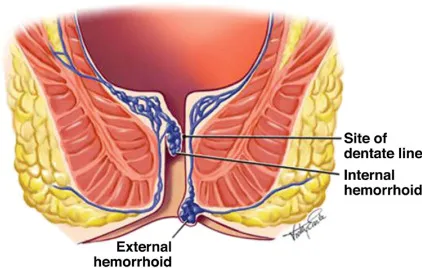
- Internal: Proximal to dentate line. Columnar epithelium. Visceral innervation (painless).
- Goligher's Classification:
- Grade I: Bleeding, no prolapse.
- Grade II: Prolapse on straining, reduces spontaneously.
- Grade III: Prolapse, requires manual reduction.
- Grade IV: Irreducible prolapse, may strangulate.
- Goligher's Classification:
- External: Distal to dentate line. Squamous epithelium. Somatic innervation (painful).
- Internal: Proximal to dentate line. Columnar epithelium. Visceral innervation (painless).
- Etiology: Straining, constipation, pregnancy, portal hypertension, prolonged sitting.
⭐ The primary locations of internal hemorrhoids are right anterior (11 o'clock), right posterior (7 o'clock), and left lateral (3 o'clock) in lithotomy position.
Etiology & Symptoms - Strain & Pain Story
-
Etiology (The "Strain" Factors):
- Chronic straining: constipation, diarrhea
- ↑ Intra-abdominal pressure: pregnancy, obesity, heavy lifting, chronic cough
- Prolonged sitting, low-fiber diet
- Age-related connective tissue degeneration
- Family predisposition
- 📌 Mnemonic: "PUSH" (Pregnancy/Pressure, Urge/straining, Sitting prolonged, Hard stools)
-
Symptoms (The "Pain & Bleed" Story):
- Painless rectal bleeding: Bright red blood on stool/tissue, or dripping. (Most common)
⭐ Internal hemorrhoids typically present with painless bleeding; pain suggests thrombosis (external/internal) or strangulation (prolapsed internal).
- Anal pain/discomfort: Especially if thrombosed or strangulated.
- Pruritus ani (itching)
- Perianal mass/lump (palpable)
- Mucous discharge
- Sensation of incomplete defecation
- Painless rectal bleeding: Bright red blood on stool/tissue, or dripping. (Most common)
Diagnosis & DDx - Anal Detective Work
-
Diagnosis:
- History: Painless bright red rectal bleeding (on tissue/stool), prolapse, discomfort, pruritus.
- Perianal Inspection: External hemorrhoids, prolapsed internal, skin tags, fissures.
- DRE: Assess tone, rule out mass. Internal hemorrhoids usually not palpable unless thrombosed.
- Anoscopy/Proctoscopy: Confirms diagnosis; visualizes & grades internal hemorrhoids.
-
Differential Diagnosis:
- Anal Fissure (severe pain with defecation)
- Colorectal Cancer (red flags: weight loss, altered bowel habits, older age)
- IBD (diarrhea, abdominal pain)
- Rectal Prolapse
⭐ Proctosigmoidoscopy/colonoscopy may be needed in patients >40 years or with red flags to exclude malignancy.
Management Matrix - Taming the Troubles
- Conservative (Grade I, uncomplicated II): 📌 Mnemonic: WASH
- Water (Sitz baths: warm, 15 min, TID)
- Analgesics/Topicals (anesthetics, steroids - short term, venotonics e.g., Daflon)
- Stool softeners & ↑Fluids
- High-fiber diet (25-35g/day), avoid straining.
- Office Procedures (Grade I-II refractory, select III):
- Rubber Band Ligation (RBL): Most common, effective.
- Sclerotherapy: Injection (e.g., 5% Phenol in oil).
- Infrared Coagulation (IRC).
- Surgical (Grade III refractory, Grade IV, complications e.g., thrombosis, strangulation):
- Conventional Hemorrhoidectomy:
- Milligan-Morgan (open): Leaves wounds open for secondary intention.
- Ferguson (closed): Primary wound closure.
- Stapled Hemorrhoidopexy (PPH/Longo): For circumferential prolapse. Reduces pain, faster recovery.
- Doppler-guided Hemorrhoidal Artery Ligation (HAL) +/- Recto-Anal Repair (RAR).
- Conventional Hemorrhoidectomy:
- Acute Thrombosed External Hemorrhoid:
- Conservative: Pain relief, sitz baths, stool softeners.
- Excision if severe pain & within 48-72 hours of onset.
⭐ Milligan-Morgan hemorrhoidectomy is an open technique leaving wounds for secondary intention healing, while Ferguson is a closed technique with primary wound closure anastamosis of rectal mucosa to anodermis .
High‑Yield Points - ⚡ Biggest Takeaways
- Internal hemorrhoids are typically painless with bright red bleeding; external hemorrhoids are painful.
- Grading (I-IV) of internal hemorrhoids is key for selecting appropriate management.
- Conservative treatment (high-fiber diet, sitz baths) is first-line for early grades.
- Rubber band ligation is a common, effective OPD procedure for Grade II and III internal hemorrhoids.
- Surgical hemorrhoidectomy (e.g., Milligan-Morgan) is reserved for Grade III/IV or complicated cases.
- Acute thrombosed external hemorrhoid presents as a painful perianal lump; consider excision if presenting within 72 hours.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

