ERAS Core Concepts - Recovery Revolution
- Goal: Attenuate surgical stress response, hasten functional recovery, ↓ complications.
- Approach: Multimodal, evidence-based, standardized perioperative care pathway.
- Focus: Optimizing patient's physiological & functional status pre, intra & post-op.
- Key Outcomes:
- ↓ Length of hospital stay (LOS)
- ↓ Post-operative morbidity (e.g., infections)
- ↑ Patient satisfaction & quality of life
- Faster return to daily activities
⭐ ERAS protocols significantly reduce the incidence and duration of post-operative ileus, a common complication after colorectal surgery.
Pre-operative ERAS - Priming the Patient
- Patient education & counselling: Crucial for compliance.
- Nutritional screening & optimisation: Correct malnutrition (e.g., Albumin >3 g/dL).
- Smoking & alcohol cessation: Stop ≥4 weeks prior.
- Anaemia correction: Target Hb >10-12 g/dL.
- No prolonged fasting: Solids 6h, clear fluids up to 2h pre-op.
- Carbohydrate loading: e.g., 800ml night before, 400ml 2h pre-op (maltodextrin).
⭐ Oral carbohydrate loading (e.g., maltodextrin drink) reduces post-operative insulin resistance and improves patient comfort.
- Selective bowel preparation: No routine Mechanical Bowel Prep (MBP) for most colonic surgery; consider for low anterior resections.
- Thromboprophylaxis: Risk-stratified (e.g., LMWH).
- Antimicrobial prophylaxis: Administer <60 mins before incision.
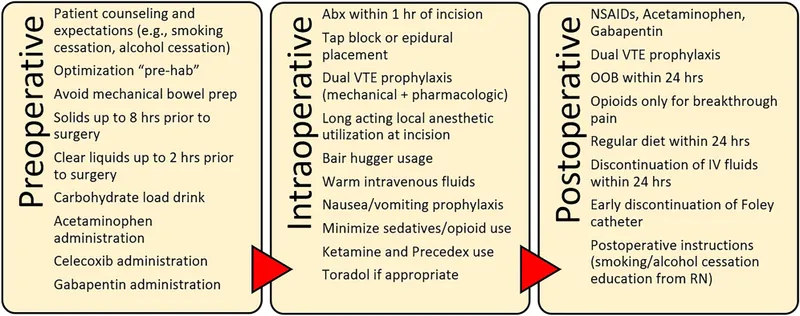
Intra-operative ERAS - Surgical Symphony
- Goal: Minimize surgical stress, optimize physiology.
- Anesthesia: Thoracic epidural analgesia (T6-T11) or transversus abdominis plane (TAP) block. Avoid long-acting opioids.
- Surgical Technique: Laparoscopic/robotic approach preferred (↓pain, ↓ileus, ↓LOS).
- Transverse incisions if open.
- Avoid routine drains/nasogastric tubes (NGT).
- Fluid Management: Goal-directed fluid therapy (GDFT); avoid overload. Target euvolemia.
- Restrictive intraoperative fluids (e.g., < 3L crystalloid).
- Normothermia: Maintain core temperature > 36°C (warming devices).

⭐ High-Yield Fact: Routine use of drains and NGTs is discouraged in ERAS protocols for colorectal surgery as they can increase discomfort and delay recovery without proven benefit in uncomplicated cases.
Post-operative ERAS - Mobilize & Nourish
- Mobilization:
- Out of Bed (OOB): Day of surgery (POD 0) or POD 1.
- Ambulate: Target 2 hrs on POD 0, 6 hrs by POD 1.
- Benefits: ↓VTE, ↓ileus, ↓pulmonary complications.
- Nutrition:
- Oral Intake: Clear liquids within hours; regular diet by POD 1-2.
- No routine Nasogastric Tube (NGT).
- Gum chewing: 3 times/day. 📌 Stimulates gut!
- IV fluids: Stop once oral intake adequate (target POD 1).
- Catheters & Analgesia:
- Urinary catheter: Remove POD 1 (within 24 hrs).
- Analgesia: Multimodal, opioid-sparing.
⭐ Early oral feeding (within 24 hours) after colorectal surgery does not increase anastomotic leak rates and reduces length of hospital stay.

ERAS Benefits & Barriers - Winning Formula
- Benefits:
- ↓ Length of Stay (LOS), ↓ complications (e.g., ileus, SSI).
- ↓ Readmission rates, ↑ patient satisfaction.
- Faster recovery & return to normal activities, overall cost savings.
- Barriers:
- Resistance to change from traditional practices.
- Lack of multidisciplinary team (MDT) coordination.
- Patient non-compliance or complex comorbidities.
- Insufficient resources, education, or standardized protocols.
- Winning Formula:
- Multimodal approach: pre-operative, intra-operative, post-operative.
- Proactive patient education and engagement.
- Dedicated MDT with clear communication channels.
- Continuous audit, feedback, and protocol refinement.
⭐ ERAS protocols are proven to significantly reduce postoperative ileus, a key factor in prolonged hospital stays.
High‑Yield Points - ⚡ Biggest Takeaways
- ERAS is a multimodal perioperative care pathway designed to accelerate recovery after colorectal surgery.
- Emphasizes preoperative patient education, carbohydrate loading, and no prolonged fasting.
- Intraoperative goals include minimally invasive techniques, goal-directed fluid therapy, and maintaining normothermia.
- Postoperative pillars are early oral feeding, early ambulation, and multimodal opioid-sparing analgesia.
- Avoids routine NG tubes and abdominal drains to promote early gut function and mobility.
- Core aims: reduced hospital stay, fewer postoperative complications, and faster return to normal function.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

