Intro & Patho - Gut Pouch Primer
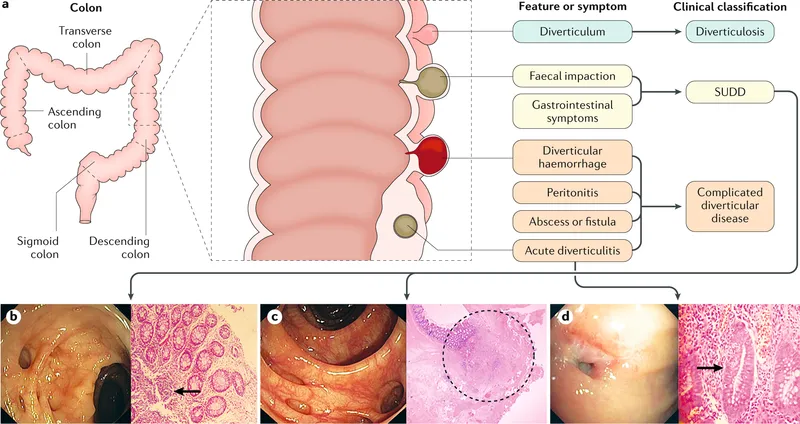
- Diverticulosis: Presence of asymptomatic outpouchings (diverticula).
- Diverticulitis: Inflammation/infection of diverticula.
- Type: Mostly false diverticula (mucosa & submucosa herniate through muscularis propria).
- Pathogenesis:
- Low fiber diet → ↓ stool bulk → ↑ intraluminal pressure.
- Herniation at weak points in colon wall (often where vasa recta penetrate).
- 📌 Mnemonic: Low Fiber, High Pressure → Pouches!

⭐ Sigmoid colon is the most common site (~95%) for diverticular disease due to highest pressure.
Clinical & Diagnosis - Spotting the Sacs
-
Asymptomatic Diverticulosis: Most common form. Sacs (diverticula) present, but no inflammation. Often an incidental finding.
-
Acute Diverticulitis: Inflammation/infection of diverticula.
- Symptoms: LLQ pain (classic, sigmoid colon most affected), fever, nausea, vomiting, altered bowel habits (constipation/diarrhea).
- Signs: LLQ tenderness, localized guarding; a palpable mass may indicate phlegmon or abscess.
-
Diagnostic Pathway:
⭐ CT scan is the gold standard and investigation of choice for suspected acute diverticulitis. It confirms the diagnosis and identifies complications.
-
Important Considerations:
- Laboratory tests: Leukocytosis (↑WBC), elevated C-reactive protein (↑CRP) are common.
- ⚠️ Avoid colonoscopy in the acute phase due to the risk of perforation. Plan 6-8 weeks after resolution to rule out underlying malignancy.
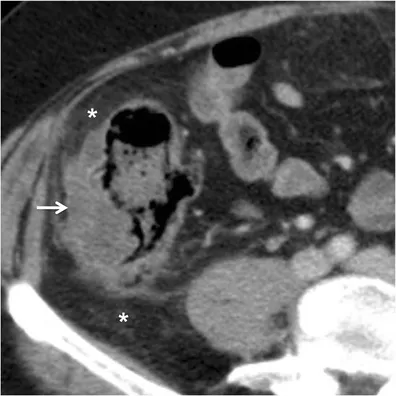
Management - Pouch Patrol Plan
- Uncomplicated Diverticulitis:
- Outpatient: Clear liquid diet, oral broad-spectrum antibiotics (e.g., Ciprofloxacin + Metronidazole or Amoxicillin-clavulanate) for 7-10 days.
- Inpatient (if severe symptoms, comorbidities, immunosuppression, or failed outpatient): NPO, IV fluids, IV antibiotics.
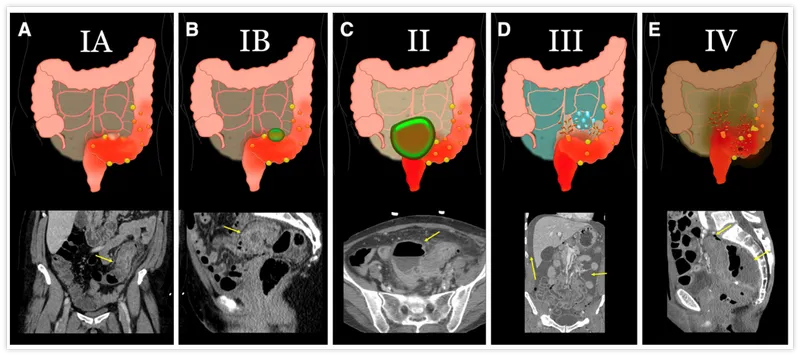
- Complicated Diverticulitis: Management guided by Hinchey Classification.
- Hinchey Stage I (Pericolic/mesenteric abscess):
- Small abscess (<4cm): IV antibiotics.
- Large abscess (≥4cm): Percutaneous drainage + IV antibiotics.
- Hinchey Stage II (Walled-off pelvic/distant intra-abdominal abscess): Percutaneous drainage + IV antibiotics.
- Hinchey Stage III (Generalized purulent peritonitis): Emergency surgery - Resection and primary anastomosis (R&A) if stable, or Hartmann's procedure.
- Hinchey Stage IV (Generalized fecal peritonitis): Emergency surgery - Hartmann's procedure.
- Hinchey Stage I (Pericolic/mesenteric abscess):
⭐ Elective sigmoid colectomy is typically considered after one episode of complicated diverticulitis or recurrent uncomplicated episodes, especially in young or immunocompromised patients.
📌 Pouch Patrol Plan: Pain relief, Outpatient/Inpatient decision, Uncomplicated vs. Complicated, Conservative (antibiotics, drainage) vs. Surgical, Hinchey guides surgery type (Hartmann's).
Complications & Prevention - Diverticula Danger Zones
- Key Complications (📌 APFS-B Mnemonic):
- Abscess: Pericolic or pelvic; managed based on size & Hinchey stage.
- Perforation: Free (generalized peritonitis) or contained. Hinchey III/IV often need surgery.
- Fistula: Colovesical most common (male > female); presents with pneumaturia, fecaluria.
- Stricture: Due to chronic inflammation, may cause large bowel obstruction symptoms.
- Bleeding: Acute, painless, massive lower GI bleed; often from right-sided diverticula.
- Prevention:
- High-fiber diet (target 20-35g/day).
- Adequate hydration & regular physical activity.
⭐ While diverticulitis (inflammation) is more common in the sigmoid colon (left side), significant diverticular bleeding is more frequently associated with right-sided colonic diverticula due to wider necks and exposure to shearing forces of fecal content across the vasa recta entry point into the diverticulum dome. This is a key distinction for diagnosis and management of lower GI hemorrhage versus acute abdomen scenarios related to diverticular disease. The bleeding is typically arterial and can be life-threatening, often requiring colonoscopic intervention, angiography with embolization, or rarely, surgical resection. In contrast, left-sided diverticulitis complications like abscess or perforation are managed based on severity (e.g., Hinchey classification), often involving antibiotics, percutaneous drainage, or surgery. Understanding this anatomical predilection for complications is crucial for clinical decision-making in patients presenting with symptoms related to diverticular disease, guiding investigations and therapeutic approaches effectively. For instance, a patient with massive painless rectal bleeding might have a right-sided diverticular source, prompting a different diagnostic and therapeutic pathway than a patient with left lower quadrant pain and fever, suggestive of sigmoid diverticulitis. This distinction is frequently tested in postgraduate medical entrance exams, emphasizing its clinical importance. The pathophysiology also differs: bleeding occurs from erosion of an artery at the dome or neck of a diverticulum, whereas inflammation and perforation are due to micro- or macro-perforation at the apex of a diverticulum, often related to increased intraluminal pressure and inspissated stool. Prevention strategies, such as a high-fiber diet, aim to reduce intraluminal pressure and improve colonic transit, thereby minimizing the risk of both inflammatory complications and potentially reducing factors that could lead to bleeding, although the direct impact on bleeding prevention is less established than for diverticulitis. The management of complications also varies significantly: bleeding may require endoscopic hemostasis or embolization, while abscesses might be drained percutaneously, and perforations or fistulas often necessitate surgical intervention. Therefore, recognizing the specific complication and its typical anatomical location is paramount for effective patient care and is a core concept in colorectal surgery training and examinations. The colovesical fistula, the most common type, classically presents with pneumaturia (air in urine) and fecaluria (stool in urine), and is a significant cause of morbidity, often requiring surgical repair. Strictures, resulting from chronic inflammation and fibrosis, can lead to symptoms of bowel obstruction and may also require surgical resection if severe. Each complication has its own set of diagnostic criteria and management algorithms, which are essential knowledge for a surgical trainee. The Hinchey classification is specifically used for grading the severity of perforated diverticulitis, guiding treatment decisions from conservative management to emergency surgery. Stage I involves a pericolic abscess, Stage II a pelvic, intra-abdominal, or retroperitoneal abscess, Stage III generalized purulent peritonitis, and Stage IV generalized fecal peritonitis. This classification is fundamental in the surgical approach to complicated diverticulitis. For prevention, a diet rich in fiber (fruits, vegetables, whole grains) is the cornerstone, aiming to increase stool bulk, reduce colonic transit time, and lower intraluminal pressure. This is thought to prevent the formation of new diverticula and reduce the risk of complications in existing ones. Adequate fluid intake and regular physical activity are also recommended as part of a healthy lifestyle that may contribute to colonic health. The emphasis on these preventive measures is high in patient counseling and public health messaging regarding diverticular disease. The contrast between left-sided inflammatory complications and right-sided bleeding sources is a recurring theme in surgical literature and examinations, highlighting the different pathophysiological mechanisms at play in different parts of the colon. This understanding helps in localizing the problem and choosing appropriate diagnostic modalities, such as CT scan for suspected diverticulitis or colonoscopy/angiography for bleeding. The management of acute diverticular bleeding often starts with resuscitation and localization of the bleeding site, followed by endoscopic therapy (e.g., clipping, thermal coagulation, epinephrine injection). If endoscopy fails or is not feasible, angiography with embolization can be attempted. Surgery is reserved for refractory bleeding or hemodynamic instability. For complicated diverticulitis, the approach depends on the Hinchey stage and the patient's clinical condition, ranging from antibiotics and bowel rest for mild cases to percutaneous drainage of abscesses and surgical resection with or without stoma for severe perforations or fistulas. The choice of surgical procedure (e.g., Hartmann's procedure vs. primary anastomosis) is also a critical decision point based on the intraoperative findings and patient stability. These diverse management strategies underscore the complexity of diverticular disease and its complications, making it a significant topic in colorectal surgery. The long-term management after an episode of complicated diverticulitis may involve elective sigmoid colectomy to prevent recurrence, especially in young patients or after multiple episodes. The decision for elective surgery is individualized, considering the patient's age, comorbidities, severity of the initial episode, and lifestyle. Prevention remains key, and dietary advice is a crucial component of post-discharge care. The role of prophylactic antibiotics or other medications in preventing recurrence is still debated and not routinely recommended. Therefore, a thorough understanding of the spectrum of diverticular disease, from asymptomatic diverticulosis to life-threatening complications, is essential for medical postgraduates. This includes knowledge of epidemiology, pathophysiology, clinical presentation, diagnostic workup, classification systems like Hinchey, and the various medical and surgical treatment options, as well as preventive strategies. The distinction between right-sided bleeding and left-sided inflammation is a particularly high-yield point for examinations. Furthermore, the increasing incidence of diverticular disease in younger populations and in Westernized societies makes it a growing public health concern, emphasizing the need for effective prevention and management strategies. The economic burden of managing complicated diverticular disease is also substantial, further highlighting the importance of preventive measures like dietary modification. The nuances of managing specific complications, such as the timing of surgery for fistulas or the indications for elective resection after an episode of diverticulitis, are common topics in surgical training and examinations. The development of minimally invasive surgical techniques has also influenced the management of complicated diverticular disease, offering potential benefits in terms of recovery and morbidity for selected patients. However, the fundamental principles of managing infection, controlling sepsis, and restoring intestinal continuity remain central to the surgical treatment of these conditions. The interplay between medical and surgical management is also crucial, with many patients requiring a multidisciplinary approach involving gastroenterologists, radiologists, and surgeons. This collaborative approach ensures optimal patient outcomes and is a hallmark of modern surgical practice. The long-term consequences of diverticular disease, including recurrent diverticulitis, chronic abdominal pain, and the need for multiple interventions, can significantly impact a patient's quality of life, underscoring the importance of effective initial management and secondary prevention. The understanding of these aspects is vital for any physician dealing with patients with gastrointestinal disorders. The specific details of surgical techniques, such as the extent of resection, the decision to perform a primary anastomosis or a stoma, and the management of intraoperative complications, are beyond the scope of a rapid revision note but form the core of surgical training in this area. However, awareness of these options and their indications is expected at the postgraduate level. The role of newer diagnostic and therapeutic modalities, such as advanced endoscopic techniques for bleeding control or novel pharmacological agents for preventing diverticulitis, is an evolving area of research and may become more prominent in future guidelines. For now, the established principles of diagnosis, classification, and management remain the foundation of clinical practice. The emphasis on high-fiber diet for prevention is a consistent recommendation across various guidelines and is a simple yet effective measure that can be promoted at all levels of healthcare. The complications of diverticular disease can be severe and life-threatening, making their prompt recognition and appropriate management critical. The
High‑Yield Points - ⚡ Biggest Takeaways
- Sigmoid colon: Most common site due to high intraluminal pressure.
- Colonic diverticula are typically false diverticula (mucosa & submucosa herniation).
- Key risk factors: Low-fiber diet, aging, obesity.
- Diverticulosis: Often asymptomatic or painless hematochezia.
- Acute diverticulitis: LLQ pain, fever; CT scan is gold standard for diagnosis.
- Hinchey classification guides management of perforated diverticulitis.
- Colovesical fistula: Most common fistula complication.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

