Epidemiology & Risk Factors - Cancer's Spread & Seeds
- Incidence: Globally common; rising in India. Peak age >50 yrs. M>F.
- Modifiable Risks:
- Diet: ↓Fiber, ↑Red/processed meat.
- Lifestyle: Obesity, smoking, alcohol, physical inactivity.
- Non-Modifiable Risks:
- Family Hx: CRC/polyps (1st degree: ~2x risk).
- Genetic: FAP, Lynch syndrome (HNPCC).
- IBD: Ulcerative Colitis (UC) > Crohn's Disease (CD).
- Personal Hx: Adenomatous polyps.
⭐ Most common inherited CRC: Lynch syndrome (HNPCC), due to mismatch repair (MMR) gene defects.
Pathology & Genetics - Malignant Makeover
- Histology: Adenocarcinoma (>90-95%).
- Variants: Mucinous, Signet-ring cell (poor prognosis), Medullary (MSI-H, better prognosis).
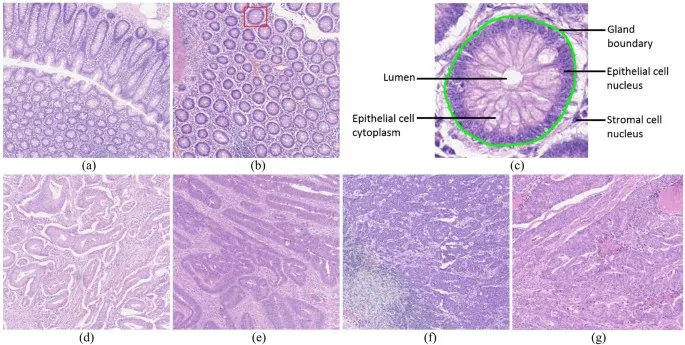
- Variants: Mucinous, Signet-ring cell (poor prognosis), Medullary (MSI-H, better prognosis).
- Key Genetic Pathways:
- Chromosomal Instability (CIN) (~80-85%): APC (early) → KRAS → TP53 (late). FAP-associated. (📌 AK-53: APC, KRAS, p53)
- Microsatellite Instability (MSI) (~15-20%): Defective DNA Mismatch Repair (dMMR) genes (MLH1, MSH2, MSH6, PMS2). MSI-H. Lynch Syndrome. Right-sided, mucinous, lymphocytic infiltrate.
- Serrated Pathway: BRAF mutations, CIMP.
⭐ Lynch Syndrome (HNPCC) accounts for 2-5% of all CRCs and is due to germline mutations in MMR genes.
Clinical Features & Diagnosis - Symptoms & Sleuthing
- Common Symptoms: Altered bowel habits (constipation/diarrhea), rectal bleeding (hematochezia/melena), abdominal pain/mass, unexplained weight loss, iron-deficiency anemia.
- Right-sided (ascending colon): Often insidious; anemia (occult blood loss), fatigue, vague abdominal pain. Mass palpable late.
- Left-sided (descending/sigmoid): Change in bowel habit (pencil stools), colicky pain, overt bleeding, obstructive symptoms.
- Rectal: Rectal bleeding (often bright red), tenesmus, urgency, feeling of incomplete evacuation.
- Diagnostic Approach (Sleuthing):
- Digital Rectal Exam (DRE): Essential for low rectal lesions.
- Fecal Occult Blood Test (FOBT) / Fecal Immunochemical Test (FIT).
- Labs: CBC (for anemia), LFTs, Carcinoembryonic Antigen (CEA) - baseline for prognosis & recurrence monitoring.
⭐ Unexplained iron deficiency anemia in an adult (especially male or postmenopausal female) warrants investigation for colorectal cancer.
- Colonoscopy: Gold standard for diagnosis; allows visualization & biopsy.
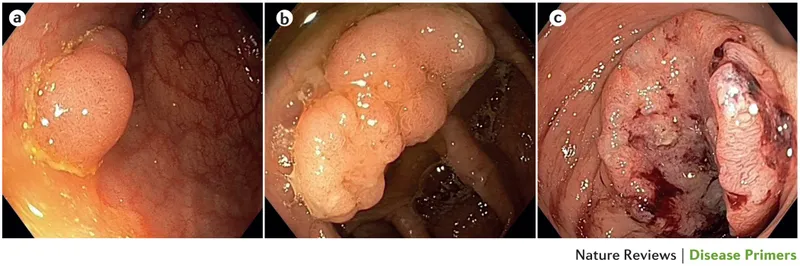
Staging & Management - Levels & Lifelines
- Staging (TNM):
- T: T1-T4 tumor depth.
- N: N0-N2 lymph nodes.
- M: M0 (no metastasis), M1 (yes).
- Workup: CT C/A/P, Pelvic MRI (rectal), CEA.
- Management:
- Colon Cancer:
- Non-metastatic: Surgery (e.g., hemicolectomy). Adjuvant chemo (FOLFOX) for Stage III/high-risk Stage II.
- Rectal Cancer:
- Early (T1-2N0 low risk): Surgery.
- Locally Advanced (T3/4 or N+): Neoadjuvant Chemoradiotherapy (NCRT) → Total Mesorectal Excision (TME) surgery (APR/LAR) → Adjuvant chemo.
⭐ TME surgery post-NCRT for locally advanced rectal cancer is standard, ↓ local recurrence.
- Metastatic (Stage IV): Palliative chemo ± targeted Rx (anti-EGFR/VEGF) ± surgery.
- Colon Cancer:
Screening & Prevention - Early Watch & Ward
- Average Risk (Age >45-50):
- Annual FOBT/FIT.
- Sigmoidoscopy q5 yrs.
- Colonoscopy q10 yrs (Gold Standard).
- High-Risk (earlier/frequent):
- Family Hx CRC/adenoma.
- IBD (UC/Crohn's >8-10 yrs).
- FAP (scope from 10-12 yrs), Lynch (scope from 20-25 yrs).
- Prevention:
- Diet: ↑Fiber, ↓Red meat.
- Lifestyle: Exercise, healthy weight, no smoking/alcohol.
- Aspirin (select high-risk).

⭐ Lynch syndrome (HNPCC): most common inherited CRC, from mismatch repair gene defects.
High‑Yield Points - ⚡ Biggest Takeaways
- CEA is for prognosis and recurrence monitoring, not screening.
- Lynch syndrome (HNPCC): Most common hereditary CRC, due to DNA mismatch repair gene defects.
- Right-sided cancers often present with iron-deficiency anemia and occult bleeding.
- Left-sided cancers typically cause altered bowel habits, tenesmus, and obstruction.
- Liver is the most common site of distant metastasis from colorectal cancer.
- FAP (APC gene mutation): Near 100% cancer risk; prophylactic colectomy is standard.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

