Anorectal Abscess & Fistula - Genesis & Germs
- Anorectal Abscess: Acute infection in spaces around the anus/rectum.
- Fistula-in-ano: Chronic abnormal tract connecting the anal canal to perianal skin.
- Genesis (Cryptoglandular Hypothesis):
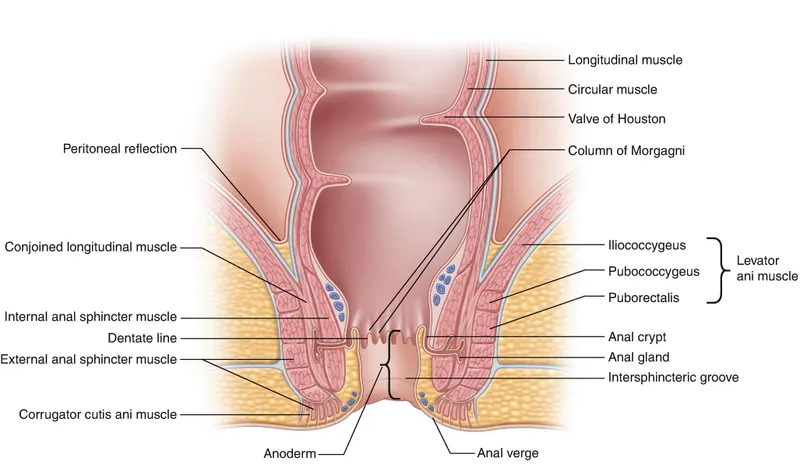
- Infection originates in anal glands (Hermann's glands) in the intersphincteric space.
- These glands drain into anal crypts (of Morgagni).
- Duct obstruction → stasis → bacterial infection → abscess.
- Abscess may drain spontaneously or require surgery, potentially forming a fistula.
- Causative Organisms (Polymicrobial):
- Escherichia coli (most common aerobe)
- Bacteroides fragilis (common anaerobe)
- Staphylococcus aureus
- Enterococcus spp.
- Streptococcus spp.
⭐ The cryptoglandular theory is the most accepted etiology for common, non-specific anorectal abscesses and fistulas.
Anorectal Abscess & Fistula - Mapping the Maze
Anorectal Abscesses: Origin: Cryptoglandular infection.
- Types & Features:
Type Location Key Feature Perianal Subcutaneous Most common (60%), fluctuant Ischiorectal Ischiorectal fossa Large, tender Intersphincteric Intersphincteric Deep pain, difficult Dx Supralevator Above levator ani Sepsis, deep pain
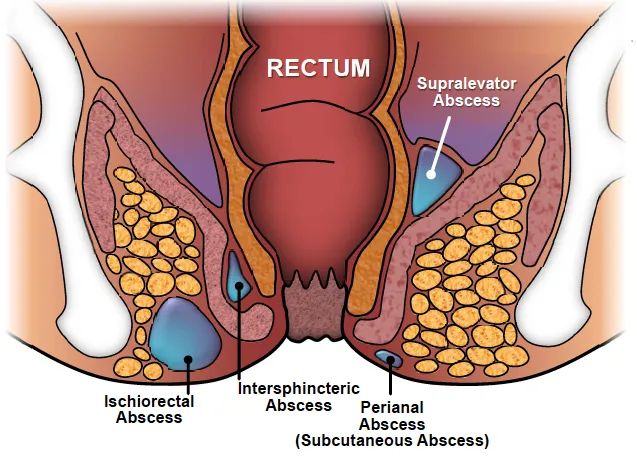
Fistula-in-Ano: Chronic sequela of abscess.
- Parks Classification:
Type Pathway Frequency Intersphincteric Intersphincteric ~70% Transsphincteric Crosses ext. sphincter ~25% Suprasphincteric Over puborectalis ~5% Extrasphincteric Outside sphincters <1%
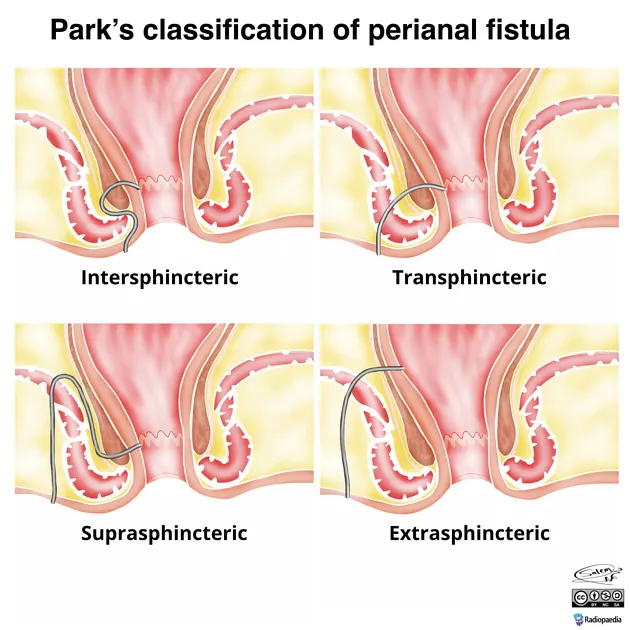
- Goodsall's Rule: Predicts internal opening.
- Anterior: straight track.
- Posterior: curved to posterior midline.
- Exception: Anterior >3cm from verge may curve.

⭐ Perianal abscess is the most common type of anorectal abscess.
Anorectal Abscess & Fistula - Signs & Scrutiny
- Symptoms:
- Abscess: Acute throbbing pain, localized swelling, erythema, fever.
- Fistula: Chronic purulent/serosanguinous discharge, recurrent abscess, external opening, pruritus ani.
- Examination:
- Inspection: External opening, induration, inflammation.
- Palpation: Tenderness, fluctuance (abscess), tract (fistula).
- DRE: Pain may limit (abscess); identify internal opening (fistula).
- Probing: Gentle; often under anaesthesia (EUA) to trace tract.
- Investigations:
- Anoscopy/Proctoscopy: Visualize internal opening.
- Complex/Recurrent Fistulas:
- Endoanal Ultrasound (EAUS/ERUS): Sphincter integrity, tract relation.
- MRI Pelvis: Gold standard; delineates entire tract, extensions, abscesses.
⭐ MRI is the gold standard investigation for complex or recurrent fistula-in-ano.
- Diagnostic Algorithm:
oka
Anorectal Abscess & Fistula - Fixing the Flow
- Abscess Management: Prompt Incision & Drainage (I&D) is mainstay; cruciate or radial incisions close to anal verge. Antibiotics: only if significant cellulitis, systemic signs (fever, ↑WBC), immunocompromised, or prosthetic heart valves.
- Fistula Surgery Principles:
- Eradicate tract, prevent recurrence.
- Preserve anal sphincter function & continence.
- Identify primary (internal) opening. 📌 Goodsall's Rule aids this.
- Surgical Options (Fistula):
- Simple/Low: Fistulotomy/Fistulectomy.
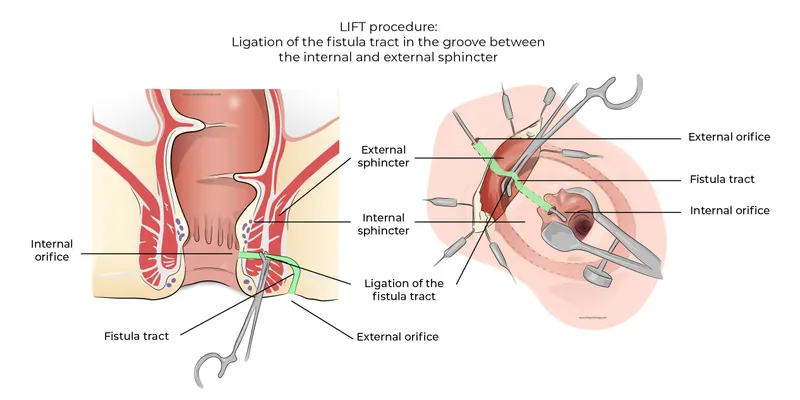
- High/Complex: Seton (draining/cutting), LIFT (Ligation of Intersphincteric Fistula Tract), VAAFT, Advancement flap, Fibrin glue/plug, FiLaC (Fistula laser closure).
⭐ The primary goal of fistula surgery is to cure the fistula while preserving continence.
 anorrectal
anorrectal
High‑Yield Points - ⚡ Biggest Takeaways
- Cryptoglandular infection in the intersphincteric space is the primary cause.
- Perianal abscess is most common; supralevator abscesses can be deep and insidious.
- Goodsall's rule predicts fistula tracks: anterior openings = straight paths, posterior = curved paths.
- Intersphincteric fistulas are the most frequent type.
- MRI is gold standard imaging for complex or recurrent fistulas.
- Abscesses require prompt incision and drainage; fistulas often need fistulotomy or seton.
- Consider Crohn's disease with multiple, recurrent, or complex fistulas.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

