SLNB Fundamentals - Node Navigator
- Definition: The first lymph node(s) to receive lymphatic drainage from a primary tumor.
- Purpose: Accurately stages the axilla in early breast cancer; guides decisions on Axillary Lymph Node Dissection (ALND) and adjuvant therapy.
- Technique: Dual method (blue dye + technetium-99m sulfur colloid) is preferred for localization.
- Injected peritumorally or subareolarly.
- Identified using a gamma probe and/or visually (blue dye).
- Key Benefit: Avoids routine ALND morbidity (e.g., lymphedema, pain) if SLN is negative.
⭐ For clinically node-negative (cN0) early breast cancer, SLNB is the standard axillary staging procedure.
The SLNB Procedure - Tracer Tactics
- Tracers Used:
- Dual technique (Gold Standard):
- Blue Dye: Isosulfan Blue (1%) or Methylene Blue. Injected intraoperatively.
- Radiocolloid: Technetium-99m ($^{ ext{99m}}$Tc) sulfur colloid / albumin nanocolloid. Injected preoperatively (2-20 hrs).
- Indocyanine Green (ICG): Emerging near-infrared fluorescent dye.
- Dual technique (Gold Standard):
- Injection Techniques & Volume:
- Sites: Peritumoral, intradermal (overlying tumor), subareolar (Sappey’s plexus).
- Volume: Blue dye ~1 mL; Radiocolloid ~0.2-0.5 mL.
- Intraoperative Identification:
- Gamma probe: Detects radiotracer ("hot" node).
- Visual: Blue dye stains lymphatics/nodes ("blue" node).
- Any "hot" or "blue" node is an SLN. Typically 1-4 SLNs removed.
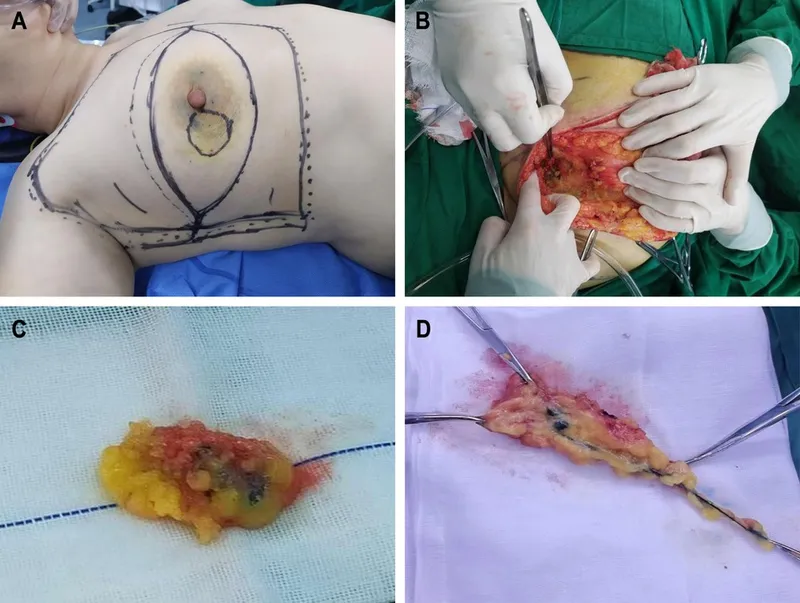
⭐ The dual technique (blue dye + radiocolloid) maximizes SLN identification rates (approaching 98%) with a false negative rate around 5-10%.
Results & Ramifications - Axillary Answers
-
SLNB Results:
- Positive:
- Macrometastasis (> 2 mm)
- Micrometastasis (0.2-2 mm)
- ITCs (≤ 0.2 mm): AJCC N0(i+), often node-negative management.
- Negative: No ALND. FNR target < 5-10%.
- Positive:
-
Management based on SLNB:
- Key Trials:
- ACOSOG Z0011: For T1/T2 tumors, 1-2 positive SLNs, WBRT planned & no ENE → ALND omission safe.
⭐ ACOSOG Z0011 showed no difference in overall survival or locoregional recurrence for omitting ALND in eligible early breast cancer patients.
- AMAROS: Axillary RT non-inferior to ALND for SLNB+ patients; associated with less lymphedema.
- ACOSOG Z0011: For T1/T2 tumors, 1-2 positive SLNs, WBRT planned & no ENE → ALND omission safe.
Complications & Contraindications - SLNB Safety Net
- Complications:
- Seroma (most common), lymphedema (↓ vs ALND)
- Intercostobrachial nerve injury: pain, numbness
- Allergic reaction (dye/radiotracer), infection/hematoma
- Axillary web syndrome, shoulder stiffness
- Contraindications (Absolute):
- Clinically positive nodes (palpable/biopsy-proven)
- Inflammatory breast cancer (IBC)
- Locally advanced breast cancer (LABC)
- Contraindications (Relative):
- Prior axillary surgery/radiotherapy
- Pregnancy (radiotracer concern)
- Multifocal/multicentric disease
- Factors ↑ False Negative Rate (FNR):
- Surgeon experience (<20 cases)
- Single tracer use (vs dual)
- Large tumor, LVI, post-NACT (Neoadjuvant Chemotherapy)
⭐ Dual mapping (blue dye + radiocolloid) is crucial to minimize FNR, especially post-NACT.
High‑Yield Points - ⚡ Biggest Takeaways
- SLNB is standard for axillary staging in clinically node-negative (cN0) invasive breast cancer.
- Dual tracer (blue dye + radiocolloid) is preferred for optimal detection and lower false negative rates.
- A negative SLN avoids axillary lymph node dissection (ALND), significantly reducing morbidity (e.g., lymphedema).
- Key contraindications: inflammatory breast cancer, palpable axillary nodes (cN+), pregnancy (for radiocolloid).
- ACOSOG Z0011 trial impacts management for 1-2 positive SLNs in select patients with breast conserving therapy.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

