BCS Intro - Why We Screen
- Primary Aim: ↓ mortality from breast cancer.
- How: Early detection of asymptomatic cancer.
- Leads to "downstaging": smaller tumors, node-negative status.
- Improves prognosis & survival rates.
- Allows for less aggressive, breast-conserving therapies.
- Indian Context: Rising incidence, often in younger women, makes screening vital.
⭐ Screening mammography can reduce breast cancer mortality by 20-40% in women aged 50-69 years.
Screening Tools - Detection Arsenal
| Modality | Key Use | Pros | Cons |
|---|---|---|---|
| Mammography (MG) | Screening (women >40-50 yrs) | Reduces mortality; BI-RADS | Radiation; ↓ sens. dense breasts |
| DBT (3D Tomo) | Dense breasts; ↓ recalls | ↑ detection vs 2D MG | ↑ radiation vs 2D; longer read time |
| Ultrasound (USG) | Adjunct (dense breasts, young <30 symp.); lumps | No radiation; cystic/solid; guides bx | Operator-dep; high false positives |
| MRI | High-risk (BRCA, >20-25% lifetime risk); staging | Highest sensitivity | Costly; ↓ specificity; contrast req. |
| CBE | Physical exam; resource-limited | Inexpensive; accessible | ↓ sensitivity; operator-dep. |
| BSE | Breast awareness | No cost; promotes awareness | No mortality benefit; may ↑ anxiety |
Screening Protocols - Guideline Grid
Screening aims for early detection. Protocols vary by risk. (ACS/NCCN guidelines commonly followed).
- Average Risk Women:
- ACS Guidelines:
- Age 40-44: Optional annual mammography.
- Age 45-54: Annual mammography.
- Age ≥55: Biennial mammography, or continue annually.
- NCCN Guidelines:
- Age ≥40: Annual mammography.
- ACS Guidelines:
- High Risk (e.g., BRCA, Strong Family Hx, Prior Chest Radiation <30 yrs):
- Annual mammography: Start age 30 (not before 25).
- Annual breast MRI: Start age 25-29.
- Clinical Breast Exam (CBE): Every 6-12 months.
- 📌 Mnemonic: "High-Risk, High-Frequency, High-Tech (MRI)".
⭐ Women with prior mantle radiation (ages 10-30) start annual mammography + MRI 8-10 years post-RT (not before age 25).
BI-RADS - Mammogram Speak
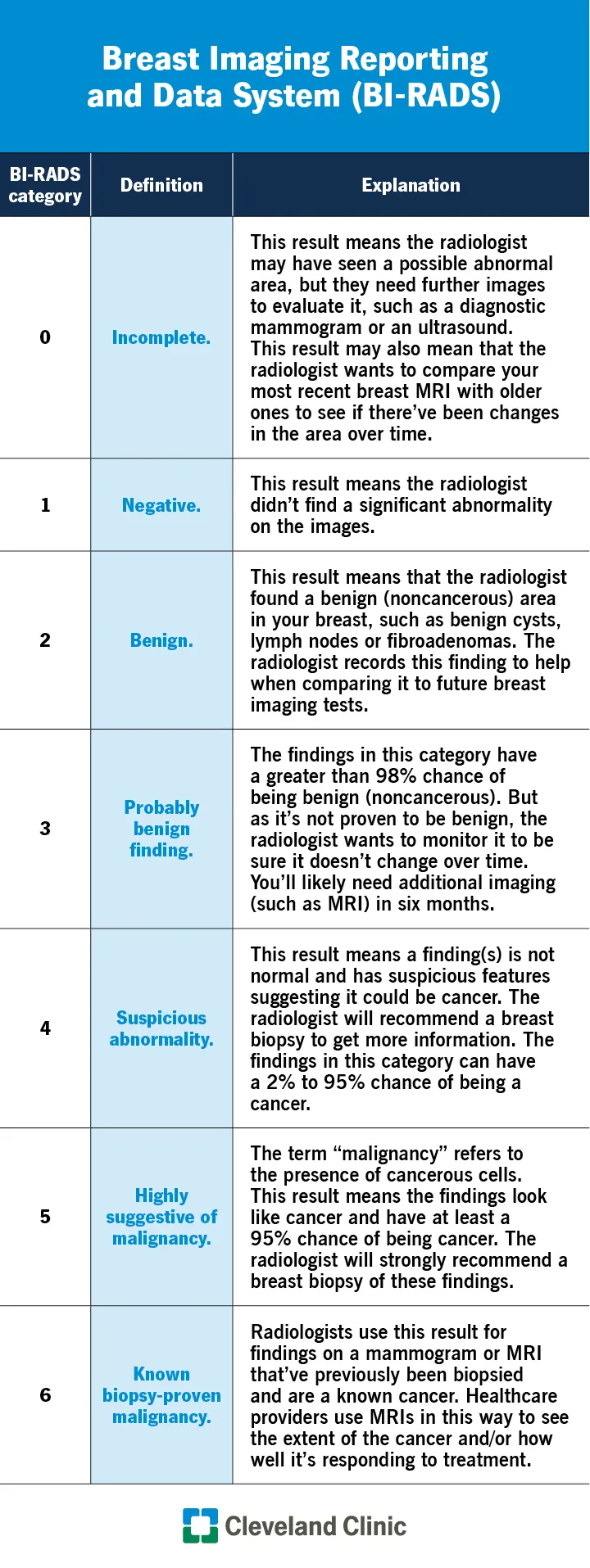
| BI-RADS | Description (Malignancy Risk %) | Management |
|---|---|---|
| 0 | Incomplete; needs more views | Additional imaging |
| 1 | Negative (0%) | Routine screening |
| 2 | Benign finding (0%) | Routine screening |
| 3 | Probably Benign (<2%) | Short-interval (6-mo) f/u |
| 4 | Suspicious. Subcategories A,B,C reflect ↑ risk (2-95%) | Biopsy |
| 5 | Highly Suggestive of Malignancy (>95%) | Biopsy |
| 6 | Known Biopsy-Proven Malignancy | Surgical excision/Treatment |
Special Cases - Nuance Navigator
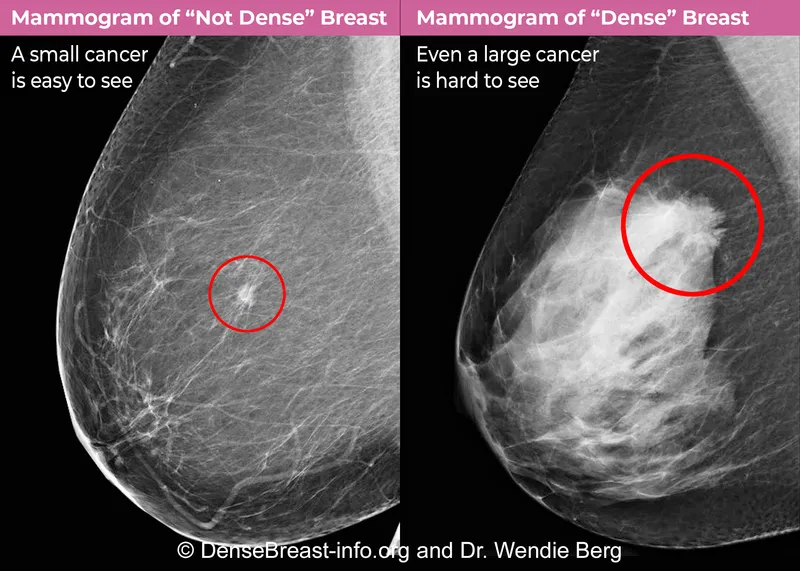
- Dense Breasts:
- Reduces mammography sensitivity, potentially obscuring lesions.
- Consider supplemental screening: Ultrasound (USG) or MRI.
- Pregnancy/Lactation:
- Ultrasound is preferred initial imaging. Shielded mammography if high suspicion.
- Male Breast Cancer:
- Routine screening not standard. Consider for high-risk (BRCA, strong family Hx).
- Post-Treatment Surveillance:
- Annual mammography. Clinical Breast Exam (CBE) every 6-12 months for 5 years, then annually.
⭐ For BRCA1/2 mutation carriers, annual breast MRI is often added to mammography for post-treatment surveillance.
High‑Yield Points - ⚡ Biggest Takeaways
- Screening mammography is the primary tool to reduce breast cancer mortality in asymptomatic women.
- Standard age for screening: 50-74 years, biennially.
- SBE & CBE alone have not shown mortality reduction in screening.
- High-risk women (e.g., BRCA carriers) need earlier screening, often including annual MRI.
- BI-RADS classification is essential for mammography reporting and guiding management.
- In India, opportunistic screening is more common than population-based programs.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

