BBD Classification & Overview - Not Always Nasty
Benign Breast Diseases (BBD): common, non-cancerous breast conditions. Most lumps are benign; reassurance is key.
- ANDI Classification (Aberrations of Normal Development and Involution):
- Relates BBD to normal physiological breast changes (development, cyclical, involution).
- Histopathological Types & Cancer Risk:
- Non-proliferative: No significant ↑ risk (e.g., cysts, mild hyperplasia).
- Proliferative (no atypia): Slight ↑ risk (1.5-2x) (e.g., fibroadenoma, usual ductal hyperplasia, sclerosing adenosis).
- Atypical proliferative: Moderate ↑ risk (4-5x) (e.g., Atypical Ductal Hyperplasia (ADH), Atypical Lobular Hyperplasia (ALH)).
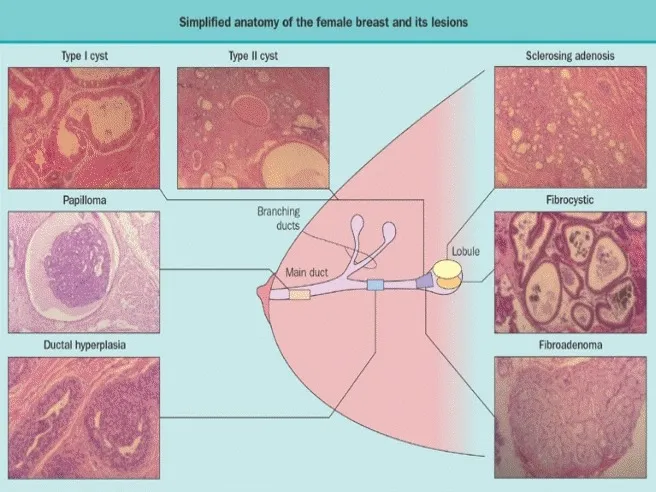
⭐ Fibrocystic change is the most common BBD, often presenting with cyclical mastalgia and lumpiness, and generally carries no increased cancer risk unless proliferative changes with atypia are present within it.
Fibrocystic Disease & Mastalgia - Hormonal Rollercoaster
- Most common benign breast condition, peak 30-50 yrs. Due to hormonal fluctuations.
- Clinically: Bilateral, lumpy, painful breasts, esp. premenstrually.
- Types & Cancer Risk:
- Non-proliferative (cysts, fibrosis): No ↑ risk.
- Proliferative w/o atypia (epithelial hyperplasia): Slight ↑ risk.
- Proliferative w/ atypia (ADH, ALH): Moderate ↑ risk.
- Mastalgia (breast pain):
- Cyclical: Common, premenstrual, bilateral, often dull/achy.
- Non-cyclical: Persistent, often unilateral; investigate to rule out malignancy.
- Mx: Reassurance, supportive bra, NSAIDs. Evening Primrose Oil. Severe cases: Tamoxifen.

⭐ Non-proliferative fibrocystic changes (cysts, fibrosis) are the most common type and do not increase breast cancer risk anaplasia or hyperplasia with atypia does increase risk significantly
Fibroadenoma & Benign Phyllodes - The Mobile Masses
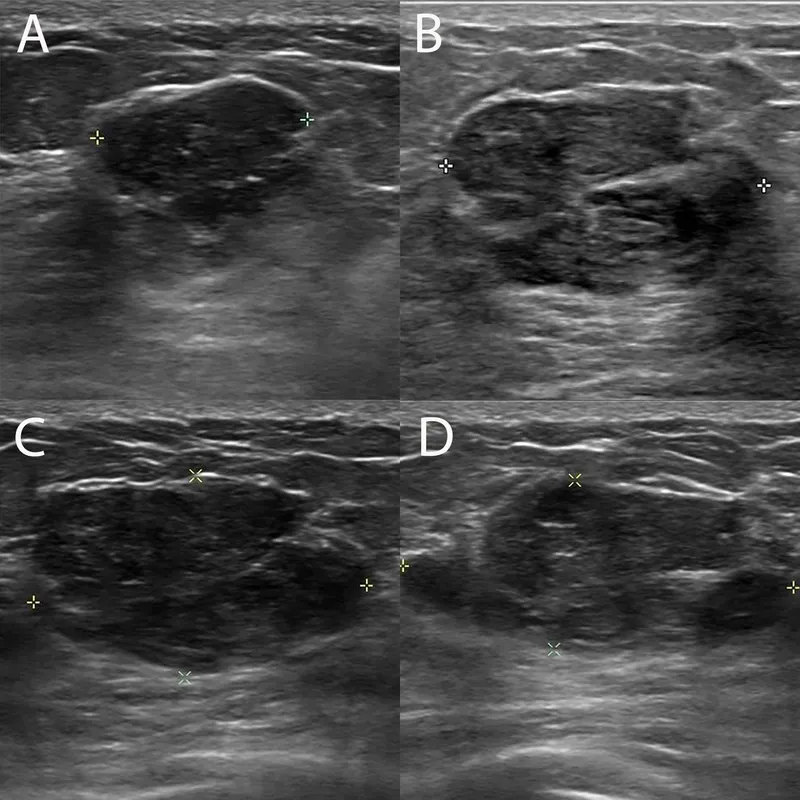
- Fibroadenoma (FA):
- Most common benign tumor; women <35 yrs.
- "Breast mouse": firm, mobile, well-defined, rubbery.
- Hormone-sensitive. Biphasic (stroma + epithelium).
- USG: Hypoechoic, wider-than-tall.
- Mx: Observe; excise if >3 cm/symptomatic.
- Benign Phyllodes Tumor (PT):
- Less common; women 40-50 yrs.
- Rapid growth, often larger. Mobile.
- Biphasic; more cellular stroma than FA; "leaf-like" pattern.
- USG: May show cystic spaces.
- Mx: Wide local excision (WLE) with ≥1 cm margin.
⭐ Phyllodes tumors, even benign, require WLE with clear margins due to recurrence risk.
Ductal Conditions & Discharge - Leaks & Lumps
- Duct Ectasia:
- Peri-menopausal women; dilated ducts, inspissated secretions.
- Nipple discharge: green/brown, sticky, often bilateral.
- May present with lump, pain, nipple retraction.
- Tx: Reassurance; microdochectomy if persistent.
- Intraductal Papilloma:
- Usually solitary; benign epithelial tumor in duct.
- Presents with serous/bloody nipple discharge.
- Mammography/USG: ductal filling defect.
- Tx: Microdochectomy or total duct excision.
⭐ Solitary intraductal papilloma is the most common cause of pathological nipple discharge.
- Galactocele:
- Milk-filled cyst; during/after lactation.
- Smooth, mobile, non-tender lump.
- Dx: Aspiration (milky fluid).
- Tx: Aspiration; rarely excision.

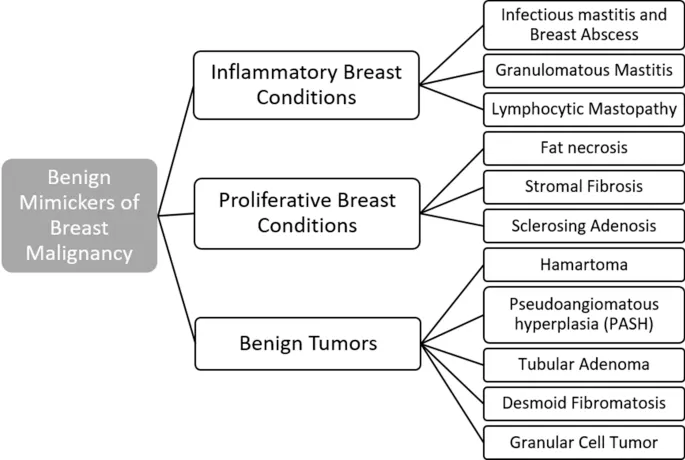
Inflammatory Conditions & Mimics - Red Flags & Oddballs
- Mastitis & Abscess:
- Lactational: Commonest, S. aureus. Pain, fever. Abscess: I&D.
- Periductal (Zuska's Disease): Smokers. Recurrent subareolar abscess, fistula. Squamous metaplasia of ducts.
- Granulomatous: Idiopathic (steroids, methotrexate) vs. TB (ATT). Mimics carcinoma.
- Other Inflammations & Mimics:
- Mondor's Disease: Superficial thrombophlebitis of thoracoepigastric vein. Tender cord. Self-limiting.
- Fat Necrosis: Post-trauma/surgery. Oil cysts, dystrophic calcification. Biopsy diagnostic.
- Diabetic Mastopathy: T1DM (long-standing). Firm, painless, ill-defined mass. Lymphocytic infiltration.
- Red Flags (suspect malignancy): Persistent mass post-antibiotics, non-resolving skin changes (peau d'orange, retraction), bloody nipple discharge.
⭐ Fat necrosis can present with spiculated masses and microcalcifications on mammography, closely mimicking malignancy; biopsy is crucial for differentiation.
High‑Yield Points - ⚡ Biggest Takeaways
- Fibroadenoma: Most common benign tumor, mobile "breast mouse", common in young women.
- Fibrocystic change: Most common breast condition, cyclical pain, lumpy; "blue-domed cysts" (pathology).
- Intraductal papilloma: Leading cause of pathological (bloody/serosanguinous) nipple discharge.
- Phyllodes tumor: Large, rapidly growing, leaf-like tumor; requires wide local excision.
- Duct ectasia: Dilated ducts with multicolored, sticky nipple discharge; perimenopausal women.
- Acute mastitis: Usually lactational, S. aureus common; continue breastfeeding_._
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more