Indications & Mechanism - Why & Who Gets Sleeved
- Mechanism:
- Restrictive: Reduces stomach to ~15-20% of original size (approx. 100-150 mL).
- Hormonal: ↓ Ghrelin (fundectomy), ↑ GLP-1, PYY (satiety).
- Indications (General Criteria):
- BMI ≥ 40 kg/m².
- BMI ≥ 35 kg/m² with comorbidities (T2DM, HTN, OSA, dyslipidemia).
- BMI ≥ 30 kg/m² with uncontrolled T2DM (especially Asian populations).
- Failed supervised weight loss.
⭐ Sleeve gastrectomy's primary mechanism is restrictive, but significant hormonal effects (↓ Ghrelin, ↑ GLP-1) contribute to weight loss and comorbidity resolution.
oka
Procedure Highlights - The Gastric Trim

- Approach: Laparoscopic, typically 5-6 ports.
- Mobilization: Greater curvature of stomach, from antrum (approx. 2-6 cm from pylorus) up to Angle of His.
- Calibration: Bougie (32-40 Fr) inserted orally to size the gastric sleeve.
- Resection: Longitudinal resection using linear staplers along the bougie.
- The fundus and body are primarily resected.
- Staple Line: Often reinforced (sutures/buttressing material).
- Result: Narrow gastric tube created.
⭐ Approximately 75-80% of the stomach is resected, primarily along the greater curvature, including the fundus (key site of ghrelin production).
Advantages & Disadvantages - Sleeve's Edge & Hurdles
Advantages (Edge):
- Technically simpler than RYGB.
- ↓ Ghrelin (fundectomy) → ↓ hunger, ↑ satiety.
- No intestinal bypass → less malabsorption (vitamins/minerals) vs RYGB.
- Good weight loss (EWL ~50-60% at 2 years).
- Staged or convertible to other procedures (RYGB, SADI-S).
⭐ Preserves pylorus (↓ dumping syndrome vs RYGB); no foreign body (vs LAGB).
Disadvantages (Hurdles):
- Irreversible (stomach removed).
- Risk of new/worsening GERD (~20%).
- Staple line issues: leak/bleed/stenosis (~1-5%).
- Potential long-term weight regain (lifestyle adherence crucial).
- Nutrient deficiencies (B12, Fe, Vit D, Ca) need lifelong monitoring.
Complications - Navigating Risks
- Early (within 30 days)
- Staple line leak (most common site: gastroesophageal junction)
- Incidence: 1-3%
- Presentation: tachycardia, fever, abdominal pain
- Hemorrhage (intraluminal or intraperitoneal)
- Incidence: 1-2%
- Pulmonary embolism/DVT
- Wound infection
- Splenic injury
- Staple line leak (most common site: gastroesophageal junction)
- Late (after 30 days)
- Stenosis/Stricture (most common at incisura angularis)
- Incidence: 0.7-4%
- Presentation: dysphagia, vomiting
- Gastroesophageal Reflux Disease (GERD) (de novo or worsening)
- Incidence: up to 20-30%
- Nutritional deficiencies (Iron, B12, Calcium, Vit D, protein)
- Gallstones (due to rapid weight loss)
- Port-site hernia
- Stenosis/Stricture (most common at incisura angularis)
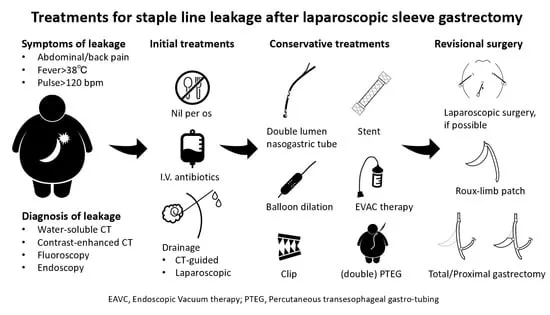
⭐ Staple line leak is the most feared early complication; GERD can be a significant long-term issue, sometimes requiring conversion to Roux-en-Y gastric bypass (RYGB).
Post-Op Care & Outcomes - Life Post-Trim
- Immediate Care: Pain management, DVT prophylaxis, early ambulation.
- Dietary Progression:
- Weight Loss: Expected %EWL ~60-70% by 1-2 years.
- Metabolic Benefits: High rates of T2DM, HTN, OSA remission.
- Key Considerations:
- GERD: May develop or worsen (~20%).
- Nutritional deficiencies: Lifelong monitoring for Iron, B12, Vit D, Calcium.
- Long-term: Regular follow-up essential.
⭐ Lifelong vitamin and mineral supplementation (e.g., B12, Iron, Calcium, Vit D) is crucial to prevent deficiencies.
High‑Yield Points - ⚡ Biggest Takeaways
- Restrictive procedure; ~80% of greater curvature resected, forming a gastric tube.
- Significantly ↓ ghrelin (hunger hormone), leading to ↓ appetite and ↑ satiety.
- Pylorus preserved, hence lower risk of dumping syndrome than bypass.
- Most common bariatric procedure worldwide; technically simpler than bypass.
- Major risks: staple line leak (most feared early complication), stenosis, and GERD.
- Lifelong multivitamin, B12, iron, calcium, Vit D supplementation crucial.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

