Intro & Principles - Size Matters!
- Restrictive Bariatric Procedures: Reduce stomach volume → early satiety & ↓ food intake.
- Mechanism: Creation of a smaller gastric pouch or sleeve. Primarily no malabsorption.
- Indications: BMI ≥ 40 kg/m² OR BMI ≥ 35 kg/m² with significant comorbidities (e.g., T2DM, HTN, OSA, severe joint disease).
- Contraindications (General): Active substance abuse, uncontrolled severe psychiatric illness, end-stage organ disease, non-adherence history.
- Pre-op Evaluation: Multidisciplinary team (surgeon, dietitian, psychologist); UGI endoscopy often required.

⭐ Restrictive procedures achieve weight loss mainly by limiting the quantity of food intake, not by inducing significant malabsorption of nutrients across the GI tract like malabsorptive procedures do (though some minor effects can occur).
Adjustable Gastric Banding - The Squeeze Play

- Mechanism: Inflatable silicone band placed around the proximal stomach, creating a small gastric pouch (approx. 15-30 mL) and a narrow stoma, restricting food intake.
- Technique: Laparoscopically placed. Band adjusted by adding/removing saline via a subcutaneous port.
- Pros: Adjustable, reversible, no malabsorption, lower early morbidity.
- Cons: Slower weight loss, foreign body, requires frequent follow-up for adjustments, less effective for super-obese.
- Complications:
- Band slippage/prolapse (most common reason for re-operation)
- Band erosion into stomach
- Port/tubing issues (leak, infection, flip)
- Esophageal dilatation, GERD
- Outcomes: Average 40-50% Excess Weight Loss (EWL).
⭐ Band slippage is the most common long-term complication of AGB requiring re-operation.
📌 Mnemonic: "BAND": Bothersome Adjustments, Not for super-obese, Device-related issues (slippage, erosion).
Sleeve Gastrectomy - Stomach Staple Saga
- Laparoscopic procedure creating a narrow gastric tube (sleeve) by resecting ~80% of the stomach, primarily fundus and body.
- Mechanism:
- Restrictive: ↓ stomach volume (capacity ~100-150 mL).
- Hormonal: ↓ Ghrelin (hunger hormone) production from fundus → ↑ satiety.
- Technique:
- Stomach stapled along a bougie (e.g., 32-40 Fr) from antrum to Angle of His.
- Resected stomach removed.
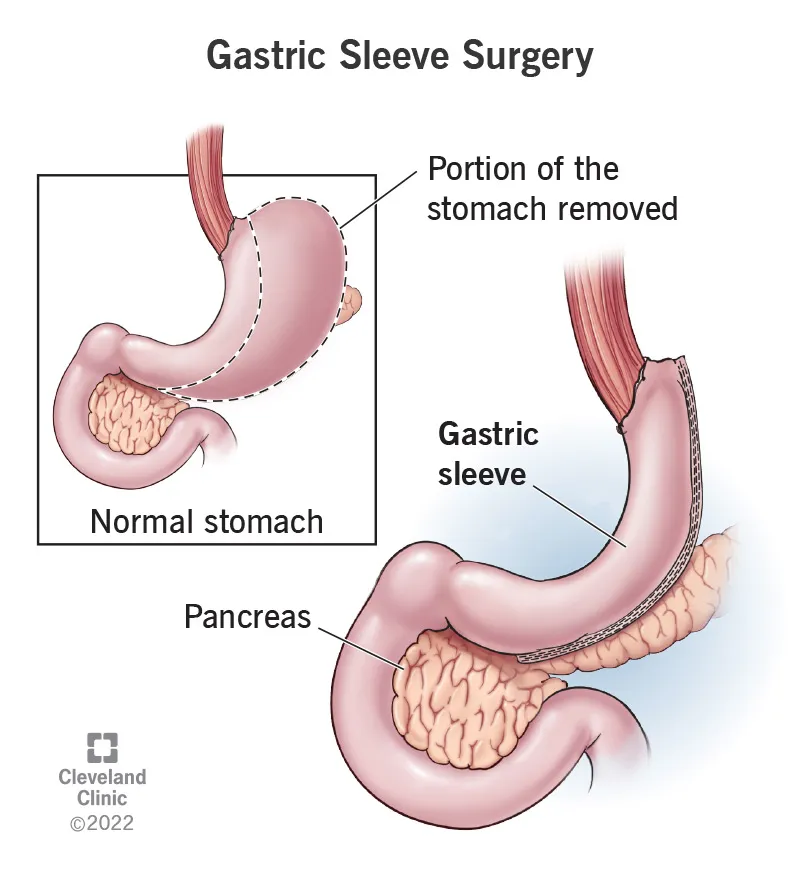
- Advantages:
- No malabsorption (vs. bypass).
- No foreign body (vs. band).
- Technically simpler than RYGB.
- Preserves pylorus; ↓ dumping syndrome risk.
- Disadvantages/Complications:
- Irreversible.
- Staple line leak (most common at gastroesophageal junction, 1-3%).
- Strictures.
- New-onset or worsening GERD (~20%).
- Bleeding.
- Outcomes: 50-60% Excess Weight Loss (EWL) at 5 years.
⭐ Most common site for a leak after sleeve gastrectomy is near the gastroesophageal (GE) junction.
Procedure Comparison - Band vs. Sleeve
- Adjustable Gastric Band (AGB)
- Mechanism: Pure restriction (external band).
- EWL: ~40-50%.
- Key Points: Reversible; higher re-operation rate (~50%); complications: slippage, erosion, port issues.
- Sleeve Gastrectomy (SG)
- Mechanism: Restrictive (removes ~80% stomach); hormonal (↓ghrelin).
- EWL: ~60-70%.
- Key Points: Irreversible; lower re-operation rate; complications: GERD, leaks (~1-3%), B12/Fe deficiency.
⭐ SG demonstrates greater, more sustained weight loss and resolution of comorbidities like Type 2 Diabetes than AGB.
Complications & Care - The Long Haul
- Early: Staple line leak (most feared), bleeding, VTE, stenosis.
- Late:
- Nutritional deficiencies (Fe, B12, Vit D, Ca - monitor).
- GERD (esp. Sleeve Gastrectomy, may need PPIs).
- Gallstones (rapid weight loss; prophylaxis: Ursodeoxycholic acid 6 months).
- Band (LAGB): slippage, erosion.
- Care: Regular F/U, lifelong vitamin/mineral supplements, endoscopy for issues.
⭐ Wernicke's encephalopathy (Thiamine deficiency) risk with persistent vomiting.

High‑Yield Points - ⚡ Biggest Takeaways
- Restrictive procedures primarily reduce gastric volume, inducing early satiety.
- LAGB: Safest, lowest mortality, but less effective weight loss and high reoperation rates.
- LSG: Most common; irreversible removal of ~80% stomach (fundus/body), reducing ghrelin.
- VBG: Historically significant, now rarely performed due to complications.
- Common complications: Stenosis, leakage, GERD (post-LSG), band issues (LAGB).
- Nutritional deficiencies are less severe than with malabsorptive procedures.
- No significant malabsorption is a key feature of restrictive types.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

