BPD: Intro & Types - Gut Game Changer
- Biliopancreatic Diversion (BPD): Primarily malabsorptive bariatric surgery.
- Mechanism: Creates significant malabsorption of fats & complex carbohydrates by diverting biliopancreatic secretions.
- Leads to substantial, sustained weight loss & metabolic improvements.
- Types:
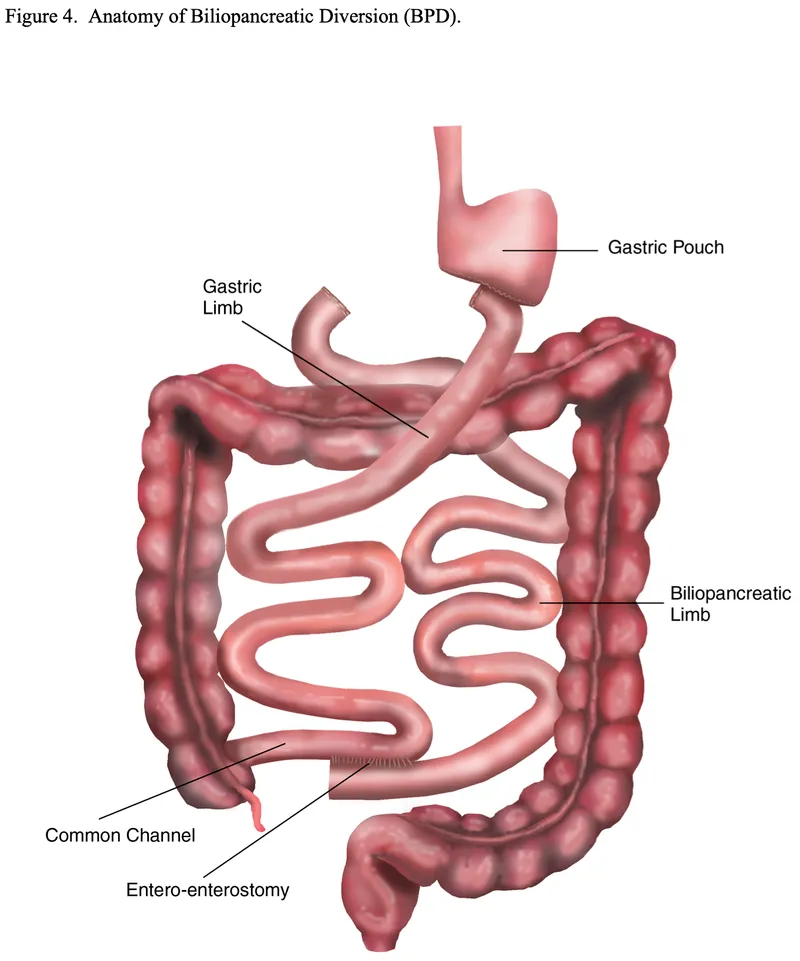
- Classic BPD (Scopinaro Procedure): Distal gastrectomy, long Roux limb (alimentary limb), short common channel (50 cm).
- BPD with Duodenal Switch (BPD/DS): Sleeve gastrectomy, duodenal transection post-pylorus, longer common channel (typically 75-150 cm, often 100 cm). Preserves pylorus, reducing dumping syndrome.
⭐ BPD/DS offers the highest and most sustained weight loss and comorbidity resolution among bariatric procedures.
 oka
oka
BPD: Candidacy - Who Gets What?
- Primary Indications:
- BMI ≥ 50 kg/m² (super-obesity).
- BMI ≥ 40 kg/m² with major obesity-related comorbidities (e.g., severe T2DM, OSA).
- BMI 35-39.9 kg/m² with refractory T2DM or severe metabolic syndrome.
- Key Considerations: Patient motivation, psychological stability, ability for lifelong adherence to follow-up & complex supplementation.
¹Major Comorbidities: Severe T2DM, OSA, etc. ²Refractory T2DM/MetS: Poorly controlled.
⭐ BPD/DS is a highly effective procedure, often reserved for super-obesity or as a revisional option when other bariatric surgeries fail.
BPD: Technique - Guts Re-Routed
- Restrictive Component: Partial/sleeve gastrectomy (stomach ~100-150 mL).
- Malabsorptive Component: Intestinal rerouting.
- Small intestine divided.
- Alimentary Limb (AL): ~250 cm; Roux-en-Y anastomosis from gastric pouch to ileum. Carries food.
- Biliopancreatic Limb (BPL): Carries bile/pancreatic enzymes.
- Common Channel (CC): 50-125 cm; AL & BPL join. Main site of absorption.
- BPD/DS (Duodenal Switch): Pylorus-preserving variant. Sleeve gastrectomy; duodeno-ileal anastomosis.

⭐ The length of the common channel (50-125 cm) is a critical determinant of malabsorption and nutritional risk.
BPD: Outcomes & Risks - Big Wins, Big Watchouts
- Wins:
- Highest weight loss: >70% EWL.
- Excellent comorbidity resolution (T2DM, HTN, OSA).
- Watchouts:
- Severe malabsorption leading to deficiencies.
- High surgical risk; lifelong follow-up crucial.
⭐ Protein-calorie malnutrition is a significant concern requiring lifelong monitoring and high protein intake.
Common Nutritional Deficiencies & Signs:
| Nutrient | Key Clinical Signs |
|---|---|
| Vit A | Night blindness, xerophthalmia, Bitot's spots |
| Vit D | Bone pain, fractures, osteomalacia, ↓Ca²⁺ |
| Vit E | Neuropathy, ataxia, hemolytic anemia (rare) |
| Vit K | Easy bruising, bleeding, ↑PT |
| Vit B12 | Megaloblastic anemia, peripheral neuropathy, glossitis |
| Iron | Microcytic anemia, fatigue, pallor, koilonychia |
| Calcium | Muscle cramps, tetany, osteoporosis, Chvostek/Trousseau |
| Protein | Edema, muscle wasting, hair loss, ↓albumin |
BPD: Post-Op - Lifelong Vigilance
- Lifelong, regular follow-up crucial.
- Monitor: Protein, vitamins (A,D,E,K, B12), minerals (Fe, Ca), LFTs, bone density.
- Mandatory: Lifelong high-dose vitamin/mineral supplements (esp. fat-soluble).
- Complications: Anemia, bone disease, kidney stones.
⭐ Lifelong, high-dose vitamin and mineral supplementation is mandatory for all BPD/DS patients.
High‑Yield Points - ⚡ Biggest Takeaways
- Biliopancreatic Diversion (BPD) offers the highest sustained weight loss and comorbidity resolution, especially Type 2 Diabetes.
- It is predominantly a malabsorptive procedure, leading to significant nutrient deficiencies.
- Lifelong supplementation of fat-soluble vitamins (A, D, E, K), iron, calcium, and B12 is mandatory.
- BPD with Duodenal Switch (BPD/DS) is a common variant, preserving the pylorus.
- Major concerns include protein-calorie malnutrition, steatorrhea, and anemia.
- Requires strict patient selection and rigorous long-term follow-up due to complexity and risks.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

