Doppler Fundamentals - Wave Wisdom
- Doppler Effect: Frequency shift from moving RBCs.
- Doppler Equation: $f_D = \frac{2 \cdot f_t \cdot v \cdot \cos\theta}{c}$
- $f_D$: shift; $f_t$: transmitted freq; $v$: velocity; $c$: sound speed (1540 m/s).
- $\theta$: Doppler angle. Optimal $\le \textbf{60}^\circ$; $\textbf{90}^\circ \implies$ no shift.
- Modes:
- CW: No aliasing/range gate. For high velocities.
- PW: Range-gated; aliasing if $f_D >$ Nyquist Limit ($PRF/2$).
- Color Doppler: Mean velocity & direction. 📌 BART: Blue Away, Red Towards.
- Power Doppler: ↑ sensitivity for low flow; no direction/velocity info.
- Spectral Doppler: Velocity-time waveform.
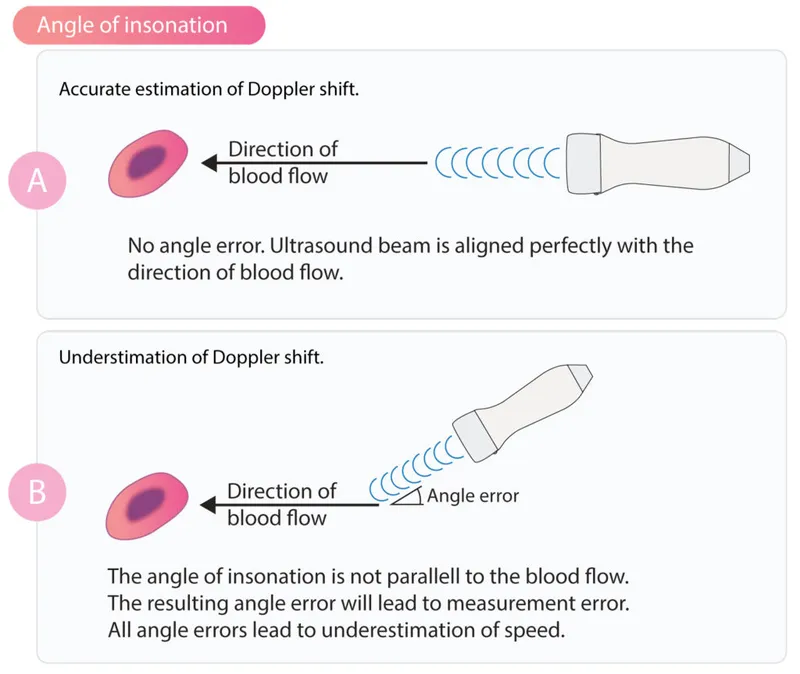
⭐ Velocity accuracy depends on Doppler angle ($\theta$); $> extbf{60}^\circ$ causes significant error. At $\textbf{90}^\circ$, no shift detected.
Arterial Assessment - Plaque Patrol
- Plaque Morphology:
- Echogenicity: Hypoechoic (lipid-rich, higher risk ⚠️), isoechoic, hyperechoic (fibrous), calcified (acoustic shadowing).
- Surface: Smooth, irregular, ulcerated (embolic risk ↑).
- Location & Extent.
- Stenosis Quantification:
- B-mode: Direct visualization.
- Color Doppler: Flow acceleration, aliasing.
- PW Doppler: ↑PSV, spectral broadening. PSV ratio: $PSV_{stenosis} / PSV_{pre-stenosis}$.
- Carotid Stenosis Grading (SRU Consensus Criteria Simplified):
- <50%: PSV <125 cm/s.
- 50-69%: PSV 125-230 cm/s, ICA/CCA PSV ratio 2.0-4.0.
- ≥70% (but not near occlusion): PSV >230 cm/s, ICA/CCA PSV ratio >4.0.
- Near Occlusion: Markedly reduced lumen, low velocity flow ("string sign").
- Total Occlusion: No flow.
- Peripheral Arterial Disease (PAD):
- Waveform changes: Triphasic (normal) → Biphasic (mild/mod) → Monophasic (severe).
⭐ Distal to significant stenosis, a "Tardus Parvus" waveform (slow systolic upstroke, low amplitude) is characteristic.
Venous Evaluation - Clot Quest
Error: Failed to generate content for this concept group.
Specialized Scans - Vascular Virtuoso
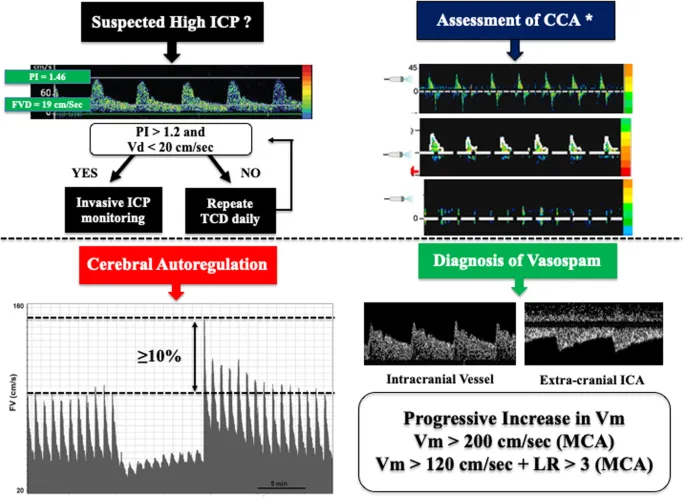
- Transcranial Doppler (TCD):
- Assesses intracranial arteries (MCA, ACA, PCA, VA, BA).
- Indications: Vasospasm (post-SAH; Lindegaard ratio >3), sickle cell stroke risk (MCA TAMMV >200 cm/s), brain death, PFO detection.
- Contrast-Enhanced Ultrasound (CEUS):
- Microbubble contrast improves vessel/perfusion imaging, lesion characterization.
- Uses: TIPS patency, endoleak detection (post-EVAR).
- Intravascular Ultrasound (IVUS):
- Catheter-based, detailed vessel wall/plaque imaging. Crucial for guiding interventions (stenting).
- Specific Applications:
- Popliteal Artery Entrapment (PAES): Dynamic scan with flexion.
- Thoracic Outlet Syndrome (TOS): Positional Doppler.
- Erectile Dysfunction: Penile Doppler (PSV <30 cm/s = arterial insufficiency).
⭐ TCD in sickle cell: MCA TAMMV >200 cm/s indicates high stroke risk, guiding prophylactic transfusions.
High‑Yield Points - ⚡ Biggest Takeaways
- Doppler effect is fundamental for assessing blood flow direction and velocity.
- Color Doppler visualizes flow: BART (Blue Away, Red Towards transducer).
- Spectral Doppler quantifies flow velocity and displays characteristic waveforms (e.g., triphasic).
- Primary diagnostic tool for DVT (deep vein thrombosis) - non-compressibility of vein is key.
- Crucial for carotid artery stenosis assessment (PSV, EDV, ICA/CCA ratio).
- Evaluates peripheral arterial disease (PAD), often correlating with Ankle-Brachial Index (ABI).
- Monitors renal transplant vascularity for complications like stenosis or thrombosis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

