Ultrasound-Guided Interventions - Guiding Principles
- Goal: Accurate, minimally invasive access for diagnosis (biopsy, aspiration) or therapy (drainage, ablation).
- Advantages: Real-time visualization, no ionizing radiation, portability, cost-effective.
- Indications: Fluid aspiration (cysts, abscesses, effusions), biopsy (FNA/core), catheter placement, nerve blocks, ablations.
- Contraindications (Relative): Uncooperative patient, uncorrectable coagulopathy, overlying infection, no safe access route.
- Pre-procedure: Informed consent, review imaging, check coagulation (INR < 1.5, platelets > 50,000/μL), antibiotics if indicated, local anesthesia.
- Techniques: Freehand vs. needle-guide. Parallel (in-plane) vs. perpendicular (out-of-plane) needle approach.
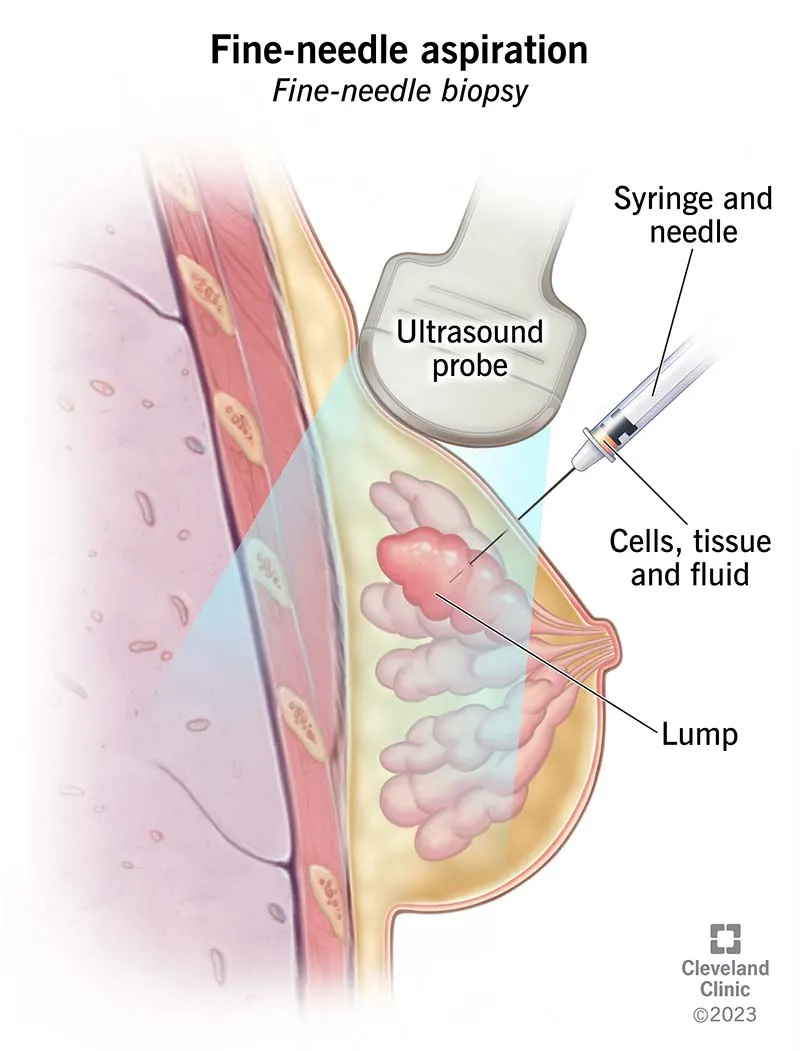
⭐ High-Yield Fact: The "tandem technique" or "free-hand technique" allows more flexibility in needle angulation compared to using a fixed needle guide, but requires greater operator skill for hand-eye coordination during US-guided procedures like biopsies or aspirations of deep-seated lesions or those with difficult access routes.
Ultrasound-Guided Interventions - Tools of Trade
- Ultrasound Machine & Probes:
- Linear: High frequency (superficial structures, vascular access).
- Curvilinear: Lower frequency (deeper structures, abdominal interventions).
- Needles:
- Spinal, Chiba, Franseen, Menghini.
- Echogenic needles: Enhanced visibility (etched, coated).
- Gauge: 18-25G common for biopsies/aspirations.
- Guidewires: Various stiffness & tip configurations (J-tip, straight).
- Catheters: Drainage (pigtail, Malecot), vascular access.
- Biopsy Guns: Automated, spring-loaded for tissue sampling.
- Sterile Probe Covers & Gel.
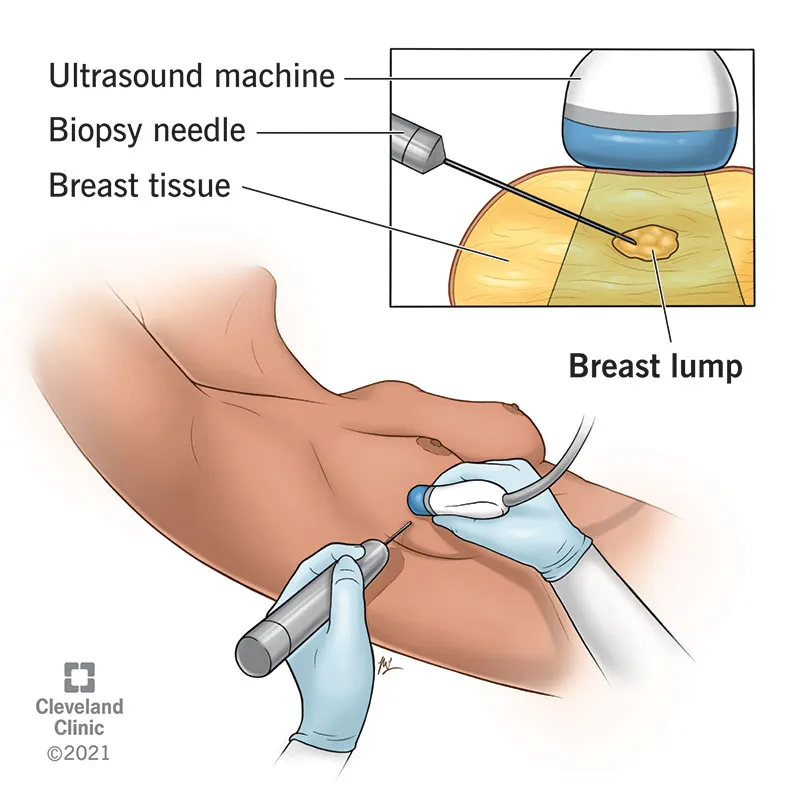
⭐ Most common needle for US-guided Fine Needle Aspiration Cytology (FNAC) is a 22-25G Chiba needle or a standard hypodermic needle. This minimizes trauma and bleeding risk while providing adequate cellularity for diagnosis in many cases, especially for thyroid or lymph node biopsies.
Ultrasound-Guided Interventions - Punctures & Probes
-
Needle Visualization Techniques:
- Freehand Technique: Probe in one hand, needle in the other. Greater flexibility.
- Parallel (In-plane): Needle shaft & tip visualized. Preferred for critical structures.
- Perpendicular (Out-of-plane): Needle seen as echogenic dot. Harder to see tip.
- Needle Guidance Systems: Attached to probe. Restricts angulation but aids alignment.
- Freehand Technique: Probe in one hand, needle in the other. Greater flexibility.
-
Needle Types & Features:
- Chiba: Thin, flexible, beveled tip.
- Spinal: Cutting stylet, various tip designs (Quincke, Whitacre).
- Trocar/Coaxial: Introducer sheath with inner needle/stylet.
- Echogenic needles: Enhanced visibility (e.g., dimpled, polymer-coated).
-
Probe Selection for Interventions:
- Linear array: High frequency, good near-field resolution. For superficial targets (e.g., thyroid, vascular access).
- Curvilinear array: Lower frequency, wider field of view, deeper penetration. For abdominal/pelvic interventions.
- Endocavitary: For transrectal, transvaginal procedures.
- Sterile probe covers & gel are mandatory.
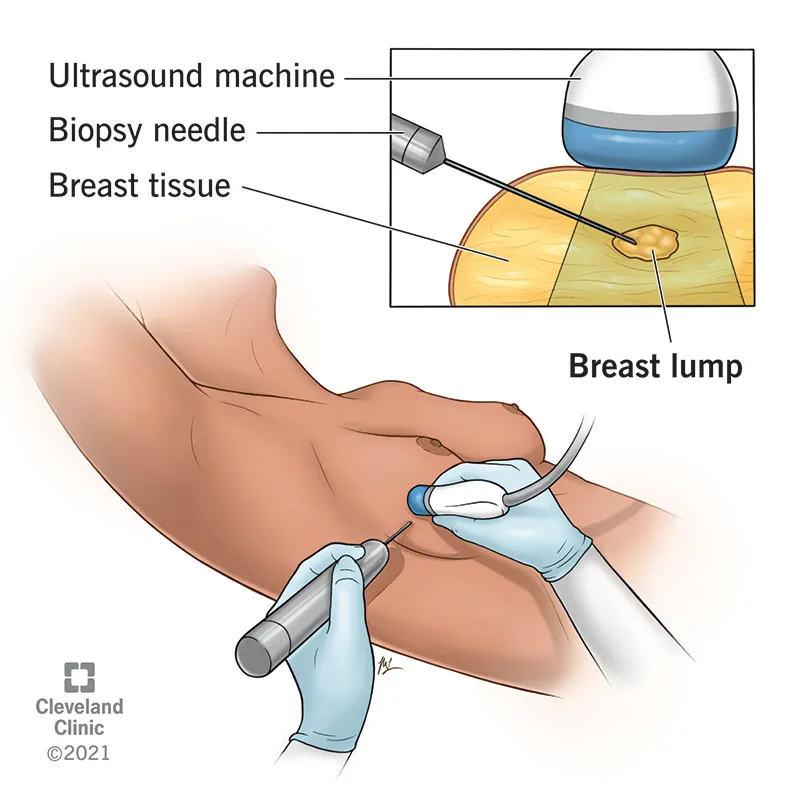
⭐ Free-breathing vs. Breath-hold: For abdominal biopsies, procedures are often done during suspended respiration (breath-hold) to minimize target motion and improve accuracy. However, for some patients or superficial lesions, free-breathing with tracking may be used.
- Puncture Routes: Shortest, safest path, avoiding vessels, bowel, vital organs. Consider patient position.
Ultrasound-Guided Interventions - Managing Mishaps
- Immediate Response:
- Recognize; Stop procedure; Ensure safety.
- ABCs assessment; Stabilize patient.
- Key Complications & Actions:
- Vasovagal: Trendelenburg, IV fluids. Atropine for severe bradycardia.
- Bleeding/Hematoma: Pressure, USG monitor. Severe: reversal agents, embolization, surgery.
- Infection: Strict asepsis. Antibiotics if signs of infection.
- Pneumothorax (Thoracic/upper abdomen): Oxygen. Chest drain if large/symptomatic.
- Non-target Puncture (e.g., bowel): USG confirm. Manage by organ; observation to surgery.
- Post-Event Steps:
- Communicate with patient/family.
- Arrange follow-up.
- Document event & actions.
⭐ For suspected arterial puncture post-biopsy, prolonged direct compression (15-20 min) and close USG follow-up for pseudoaneurysm are crucial.
High‑Yield Points - ⚡ Biggest Takeaways
- Real-time visualization is the primary advantage, allowing dynamic needle tracking.
- Absence of ionizing radiation ensures safety for patients and operators.
- Key procedures include FNAC/core biopsies, fluid aspirations, abscess drainages, and nerve blocks.
- Echogenic needles and saline injection (hydrodissection) enhance needle visibility.
- The "in-plane" technique (longitudinal to needle) is preferred for continuous visualization.
- High-frequency linear transducers for superficial lesions; low-frequency curvilinear for deep structures.
- Major complications like significant bleeding or sepsis are infrequent with proper technique.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

