Ultrasound Fundamentals - Wave Basics
- Ultrasound (US): Sound waves with frequency > 20 kHz.
- Diagnostic US range: 2-15 MHz.
- Nature: Longitudinal, mechanical waves; require a medium to propagate.
- Key Wave Properties:
- Wavelength ($\lambda$): Distance per cycle. $\lambda = c/f$. Shorter $\lambda$ (higher $f$) $\rightarrow$ better axial resolution.
- Frequency ($f$): Cycles per second (Hz). Determined by the transducer.
- Propagation Speed ($c$): Speed of sound in a medium. $c = f\lambda$.
- Average in soft tissue: 1540 m/s.
- Period ($T$): Time for one cycle. $T = 1/f$.
- Amplitude: Maximum particle displacement from equilibrium. Relates to loudness.
- Power ($P$): Rate of energy transfer (Watts). $P \propto \text{Amplitude}^2$.
- Intensity ($I$): Power per unit area (W/cm² or mW/cm²). $I = P/A$.

⭐ The speed of ultrasound ($c$) in a tissue is determined by the medium's density and stiffness, not by the frequency or wavelength of the ultrasound wave itself. It is generally highest in solids, lower in liquids, and lowest in gases. For example, $c_{\text{bone}} > c_{\text{soft tissue}} > c_{\text{air}}$.
Tissue Interactions & Attenuation - Echo Chamber
- US waves interact with tissues: Reflection, Refraction, Scattering, Absorption.
- Reflection: Forms images.
- Specular: Large, smooth interfaces (e.g., diaphragm). Angle-dependent.
- Diffuse (Scattering): From parenchyma; less angle-dependent.
- Acoustic Impedance (Z): $Z = \rho \cdot c$ (density $\times$ propagation speed).
- Key for reflection: ↑ Z mismatch = ↑ reflection (echo).
- Refraction: Beam bending at interfaces with different $c$. Snell's Law: $\frac{\sin \theta_i}{\sin \theta_t} = \frac{c_1}{c_2}$. Can cause artifacts.
- Scattering: Sound redirection. Rayleigh (e.g., RBCs) $\propto \text{frequency}^4$.
- Absorption: US energy to heat; primary attenuation cause. ↑ with frequency.
- Attenuation: Overall intensity loss.
- Coefficient ($\alpha$) in soft tissue: approx. 0.5 dB/cm/MHz.
- Total Attenuation (dB) = $\alpha \times f \text{ (MHz)} \times \text{path length (cm)}$.
- ↑ Frequency = ↑ Attenuation, ↓ Penetration, but ↑ Resolution.

⭐ Attenuation is the main reason why high-frequency probes (good resolution) cannot be used to image deep structures.
Transducers & Beam - Crystal Clear
- Transducer: Converts electrical ↔ ultrasound energy (piezoelectric effect).
- Material: Lead Zirconate Titanate (PZT).
- Crystal thickness: Inversely proportional to frequency ($f \propto 1/\text{thickness}$).
- Components & Function:
- Matching Layer: ↓ Impedance mismatch ($Z_{crystal} > Z_{match} > Z_{tissue}$), ↑ energy transmission.
- Damping Material: ↓ Spatial Pulse Length (SPL). 📌 Improves Axial resolution, ↑ Bandwidth (DAB).
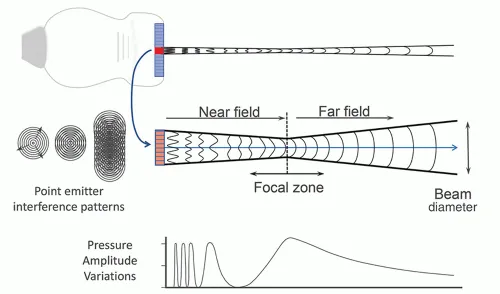
- Beam Shape:
- Near Field (Fresnel Zone): Converging. Length $L = D^2f/(4c)$.
- Focal Zone: Narrowest part of beam, best lateral resolution.
- Far Field (Fraunhofer Zone): Diverging. Divergence angle $\sin(\theta) = 1.22\lambda/D$.
- Focusing: Narrows beam width, improving lateral resolution (methods: curved element, lens, electronic phasing).
⭐ Higher frequency improves both axial and lateral resolution but reduces penetration depth.
Doppler & Artifacts - Motion & Mayhem
- Doppler Effect: US frequency shift from moving reflectors (RBCs).
- Doppler Shift ($f_D$): $f_D = \frac{2 \cdot f_t \cdot v \cdot \cos\theta}{c}$.
- Angle $\theta$: Beam-flow angle. Optimal 0°; keep <60° for accuracy.
- Types:
- CW: High velocities; range ambiguity.
- PW: Range-gated; aliasing if velocity > Nyquist limit ($PRF/2$).
- Color: Mean velocity, direction. 📌 BART: Blue Away, Red Towards.
- Power: Flow presence (sensitive); no direction/velocity.
- Artifacts: Image misrepresentations.
- Acoustic Shadowing: Signal loss deep to high attenuators (e.g., stone).

- Acoustic Enhancement: ↑ signal deep to low attenuators (e.g., cyst).
- Reverberation: Multiple linear echoes (e.g., comet tail).
- Mirror Image: Structure duplicated across strong reflector.
- Aliasing (Doppler): Velocity wrap-around if > Nyquist limit.
⭐ Aliasing: Most common Doppler artifact. Occurs if Doppler shift > $PRF/2$ (Nyquist limit).
- Twinkle Artifact: Color noise posterior to stones (e.g., renal calculi).
- Acoustic Shadowing: Signal loss deep to high attenuators (e.g., stone).
High‑Yield Points - ⚡ Biggest Takeaways
- Piezoelectric crystals in transducers convert energy forms.
- Acoustic impedance (Z = ρc) differences at interfaces cause echoes.
- High frequency = ↑ resolution, ↓ penetration; Low frequency = ↓ resolution, ↑ penetration.
- Attenuation (signal loss) is frequency-dependent, increasing with tissue depth.
- Doppler principle assesses blood flow velocity and direction.
- Recognize artifacts: acoustic shadowing (calcification/stones), posterior enhancement (cysts), reverberation.
- ALARA principle (As Low As Reasonably Achievable) minimizes patient exposure.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

