Pelvic US: Basics & Probes - Pelvic Peep Show
- Key approaches: Transabdominal (TAS) & Transvaginal (TVS).
- TAS: Uses lower frequency (3.5-5 MHz) curvilinear probe.
- Provides wider field of view.
- Requires full bladder as acoustic window.
- Best for general pelvic overview, large masses.
- TVS: Uses higher frequency (5-9+ MHz) endocavitary probe.
- Offers superior image resolution for details.
- Requires empty bladder.
- Optimal for uterus, endometrium, ovaries.

⭐ TVS provides superior detail for endometrial assessment and early pregnancy.
Normal Anatomy on US - Womb With A View
- Uterus: Pear-shaped. Position: Anteverted (common) or retroverted.
- Myometrium: Homogeneous, mid-grey echotexture.
- Endometrium: Appearance varies with menstrual cycle.
- Proliferative: Trilaminar ("three-line sign"). Max thickness 4-8 mm.
- Secretory: Thick, echogenic. Max thickness 7-16 mm.
- Menstrual: Thin, echogenic line.
- Cervix: Lower segment, more fibrous. Nabothian cysts (anechoic) common.

- Ovaries: Almond-shaped, hypoechoic stroma with peripheral anechoic follicles.
- Location: Ovarian fossa, posterolateral to uterus.
- Size: Variable, approx. 3 x 2 x 2 cm. Volume < 10 cc premenopausal.
⭐ Ovarian follicles are best visualized in the follicular phase; a dominant follicle can reach 18-25 mm before ovulation.
- Adnexa:
- Fallopian tubes: Usually not visualized unless fluid-filled (e.g., hydrosalpinx).
- Pouch of Douglas (Cul-de-sac):
- Posterior to uterus. Small anechoic free fluid can be normal (physiological).
Uterine Pathologies - Womb Worries Unveiled
- Leiomyomas (Fibroids): Most common benign uterine tumors.
- USG: Well-defined, hypoechoic masses, often with posterior acoustic shadowing.
- Types: Subserosal, Intramural (commonest), Submucosal (associated with abnormal uterine bleeding, infertility).

- Adenomyosis: Endometrial glands/stroma within myometrium.
- USG: Diffusely enlarged, globular uterus; heterogeneous myometrium; myometrial cysts ("Swiss cheese" appearance); indistinct endometrial-myometrial junction; Venetian blind shadowing. Junctional zone > 12 mm.
- Endometrial Hyperplasia/Carcinoma:
- USG: Thickened endometrium.
- Postmenopausal: > 5 mm (if bleeding), > 11 mm (asymptomatic).
- Premenopausal: Variable, > 15-20 mm often considered suspicious.
- May show irregularity, heterogeneity, increased vascularity on Doppler. Tamoxifen effect: thickened, cystic endometrium.
- USG: Thickened endometrium.
- Asherman's Syndrome: Intrauterine adhesions.
- USG: Thin or absent endometrial stripe, echogenic bands traversing uterine cavity. Hysterosonography is more diagnostic.
⭐ A thickened junctional zone (> 12 mm) on transvaginal ultrasound is a key diagnostic feature of adenomyosis, often described as a "bulky uterus with poor demarcation between endometrium and myometrium."
Ovarian & Adnexal Pathologies - Ovary Action & Alerts
- Common Cysts:
- Follicular: Anechoic, <3 cm.
- Corpus Luteum: "Ring of fire" (vascular).
- Hemorrhagic: Lace-like/reticular, avascular.
- Endometrioma: "Ground glass" echoes.
- Dermoid: Hyperechoic (fat), Rokitansky nodule, "tip of iceberg".
- ⚠️ Ovarian Torsion: Surgical Emergency!
- Enlarged ovary (>4 cm), stromal edema, peripheral follicles.
- "Whirlpool sign" (twisted pedicle). Doppler: ↓/absent flow (variable, may be present).
- ⚠️ Ectopic Pregnancy: Life-threatening!
- Empty uterus, adnexal mass (tubal ring), free fluid. β-hCG vital.
- PID / TOA: Hydrosalpinx ("cogwheel"), complex TOA.
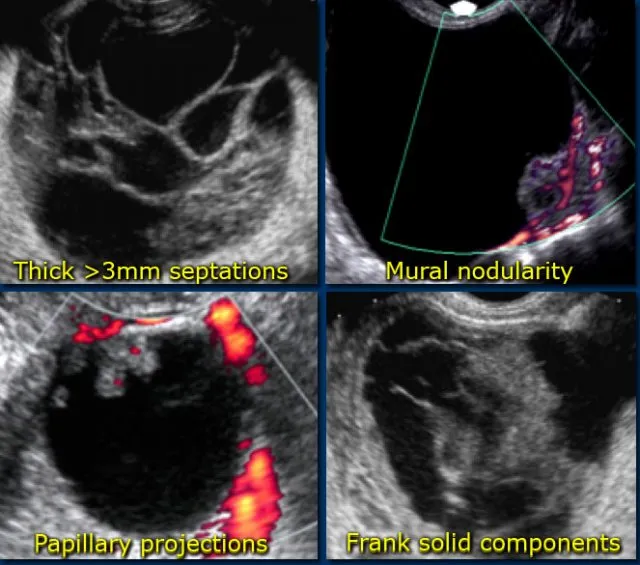
- Malignancy Red Flags (US):
- Solid irregular components, thick septa (>3 mm), papillary projections (≥4).
- Ascites, ↑vascularity (low RI <0.4).
- 📌 IOTA Simple Rules for risk.
⭐ Meigs' Syndrome: Benign ovarian tumor (fibroma) + ascites + pleural effusion.
High‑Yield Points - ⚡ Biggest Takeaways
- Transvaginal Sonography (TVS) provides superior resolution for uterus and adnexa over transabdominal USG.
- Endometrial thickness >5mm (postmenopausal bleeding) or >15mm (premenopausal, symptomatic) often warrants further investigation/biopsy.
- PCOS: Ultrasound shows "String of pearls" appearance, ovarian volume >10cc, and/or ≥12 antral follicles (2-9mm) per ovary.
- Uterine fibroids (leiomyomas): Typically hypoechoic, well-defined masses; sonographic appearance can vary, location is critical.
- Ovarian torsion: Key signs include an enlarged ovary, stromal edema, peripherally displaced follicles, and absent/reduced Doppler flow.
- Ectopic pregnancy: Suspect with an adnexal mass (often with "ring of fire" sign), an empty uterus, and possible free fluid in the pelvis, correlating with β-hCG levels.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

