Obstetric Ultrasonography - Tiny Beginnings
- Confirms Intrauterine Pregnancy (IUP), viability, and dates early gestation.
- Transvaginal Sonography (TVS) preferred over Transabdominal (TAS) for superior resolution.
- Key Milestones (TVS):
- Gestational Sac (GS): 4.5-5 wks. First reliable sign of IUP.
- Yolk Sac (YS): 5-5.5 wks. Confirms IUP definitively.
- Fetal Pole (Embryo): 5.5-6 wks.
- Cardiac Activity: Visible from ~5.5-6 wks; mandatory if CRL >7 mm.
- Discriminatory hCG: GS visible on TVS if β-hCG >1500-2000 mIU/mL.
- Dating: Crown-Rump Length (CRL) is most accurate (±3-5 days in 1st trimester).
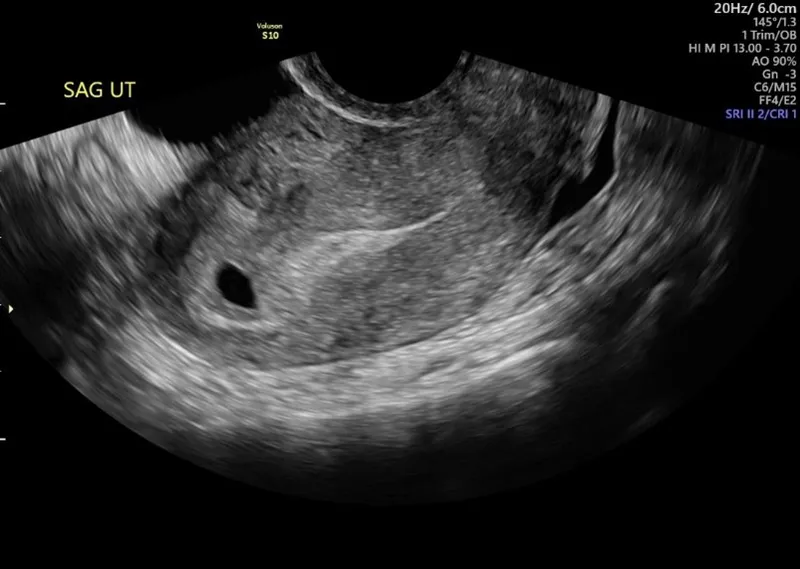
⭐ The Double Decidual Sac Sign (DDSS) on TVS is an early reliable indicator of IUP, seen around 4.5-5 weeks, before the yolk sac visualization is definitive for IUP confirmation prior to embryo visualization.
Obstetric Ultrasonography - Anomaly Detective
- A.k.a. TIFFA / Level II scan; optimal at 18-22 weeks gestation.
- Purpose: Comprehensive fetal anatomical survey for detecting structural anomalies.
- Key Systems Evaluated:
- CNS: Ventriculomegaly (atrial width >10mm), posterior fossa (e.g., banana sign for spina bifida).
- Cardiac: Four-chamber view, outflow tracts.
- GIT: Stomach bubble, bowel (e.g., "double bubble" for duodenal atresia).
- Renal: Kidneys (pelviectasis >4mm <28wks, >7mm ≥28wks), bladder.
- Skeletal: Limbs, spine.
- Also assesses: Placenta (position, grade), umbilical cord, amniotic fluid volume (AFI).
- Soft markers (e.g., nuchal fold >6mm, EIF) may indicate ↑ aneuploidy risk.
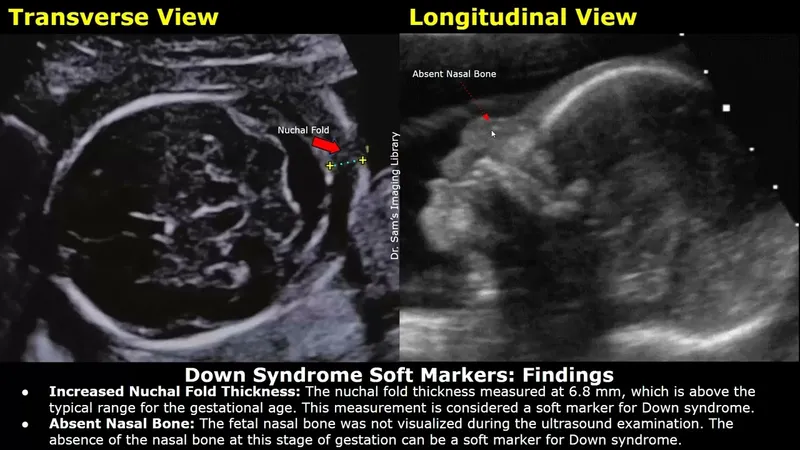
⭐ The "lemon sign" (frontal bone scalloping) and "banana sign" (cerebellar effacement, obliteration of cisterna magna) are classic cranial signs associated with open spina bifida on a mid-trimester scan.
Obstetric Ultrasonography - Spurt Checkup
- Late pregnancy (typically 3rd trimester) evaluation focusing on fetal growth, development, and well-being.
- Key assessments:
- Estimated Fetal Weight (EFW): Tracks growth, identifies IUGR or macrosomia.
- Amniotic Fluid Index (AFI): Normal range 5-25 cm.
- Biophysical Profile (BPP): Score out of 8 (ultrasound only) or 10 (if Non-Stress Test included).
- Doppler studies: Umbilical Artery (UA), Middle Cerebral Artery (MCA) for fetal adaptation.
- Placental localization, grading (e.g., Grannum grade), and cervical length assessment.
⭐ An AFI <5 cm indicates oligohydramnios, while an AFI >25 cm suggests polyhydramnios; both require careful monitoring or intervention based on gestational age and clinical context.
Obstetric Ultrasonography - Vital Vibes
- Assesses fetal well-being, crucial in high-risk pregnancies.
- Biophysical Profile (BPP): Max 10 (US+NST) or 8 (US). Each 2 pts.
- Components: Breathing, Movements, Tone, AFV, NST.
- Doppler US:
- Umbilical Artery (UA): ↑S/D ratio, PI, RI → placental insufficiency.
- Middle Cerebral Artery (MCA): ↓PI → brain sparing (fetal hypoxia).
- Ductus Venosus (DV): Abnormal 'a' wave → severe compromise.
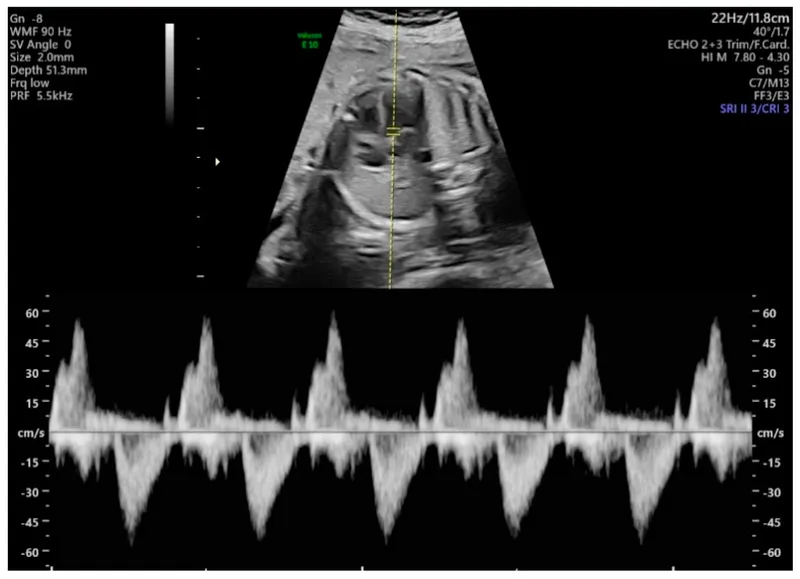
⭐ In Umbilical Artery Doppler, Absent or Reversed End-Diastolic Flow (AREDF) indicates severe fetal compromise.
Obstetric Ultrasonography - Clue Spotting
- 1st Trimester:
- Double bleb sign: IUP (yolk & amniotic sacs).
- Double decidual sign: Confirms IUP.
- Empty amnion sign: Anembryonic pregnancy.
- Snowstorm appearance: Molar pregnancy.
- 2nd/3rd Trimester Anomalies:
- Lemon sign & Banana sign: Spina bifida (Chiari II).
- Strawberry skull: Trisomy 18.
- Cloverleaf skull: Thanatophoric dysplasia.
- Double bubble sign: Duodenal atresia.
- Keyhole sign: Posterior urethral valves.
- Fetal Demise Clues:
- Spalding's sign: Overlapping skull bones.
- Robert's sign: Gas in vessels.
⭐ "Double bubble" sign (dilated stomach & duodenum) indicates duodenal atresia.
High‑Yield Points - ⚡ Biggest Takeaways
- CRL: Most accurate 1st trimester dating. NT (11-14 wks) for aneuploidy screening.
- TIFFA/Anomaly Scan (18-20 wks): For fetal structural defects.
- Doppler (UA, MCA): Assesses fetal well-being, IUGR, and hypoxia.
- Biophysical Profile (BPP): Score 8-10 is normal; evaluates fetal oxygenation.
- Earliest TVS signs: GS (4.5-5w), YS (5-5.5w), Fetal Heart (5.5-6w).
- AFI: Normal 5-25 cm. Crucial for fetal well-being.
- IUGR: AC is the single most sensitive parameter for detection.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

