USG Physics - Sound Wave Secrets
- Ultrasound: Longitudinal mechanical wave; frequency >20 kHz. Medical USG: 2-20 MHz.
- Velocity ($v$) = Frequency ($f$) × Wavelength ($\ ext{λ}$). $v = f \ ext{λ}$.
- Acoustic Impedance ($Z$): Tissue's sound resistance. $Z = \text{Density} (\rho) \times \text{Propagation Speed} (c)$. Unit: Rayl.
- Interactions: Reflection (image basis), refraction, scattering (e.g., Rayleigh from RBCs), absorption (heat).
- Attenuation: Sound intensity ↓ with depth. Proportional to frequency (approx. 0.5 dB/cm/MHz in soft tissue).
- Piezoelectric Effect: Transducer (PZT crystals) converts electrical ↔ mechanical energy.
- Curie Temperature: Max temp for piezoelectricity.

- Curie Temperature: Max temp for piezoelectricity.
⭐ Higher frequency offers better axial resolution but suffers from increased attenuation, limiting penetration depth.
Transducers & Beam - The Probe's Power
- Function: Converts electrical to ultrasound energy & vice-versa (Piezoelectric effect; PZT crystals).
- Matching Layer: $1/4 \lambda$ thick. ↓ Acoustic impedance mismatch (PZT > tissue), ↑ transmission.
- Damping Material: ↓ Spatial Pulse Length (SPL), ↑ axial resolution, ↑ bandwidth.

- Beam Shape:
- Near Field (Fresnel): Converging. Length $L \approx D^2 / (4\lambda)$.
- Focal Zone: Narrowest part; best lateral resolution.
- Far Field (Fraunhofer): Diverging.
- Common Probes: Linear (vascular), Convex (abdomen), Phased Array (cardiac).
⭐ Higher frequency = ↑ Resolution (axial, lateral), ↓ Penetration. Lower frequency = ↓ Resolution, ↑ Penetration.
Imaging Modes & Display - Pixel Perfect Pictures
- A-Mode (Amplitude): 1D display. Echo strength as spikes vs. depth. Ophthalmic use.
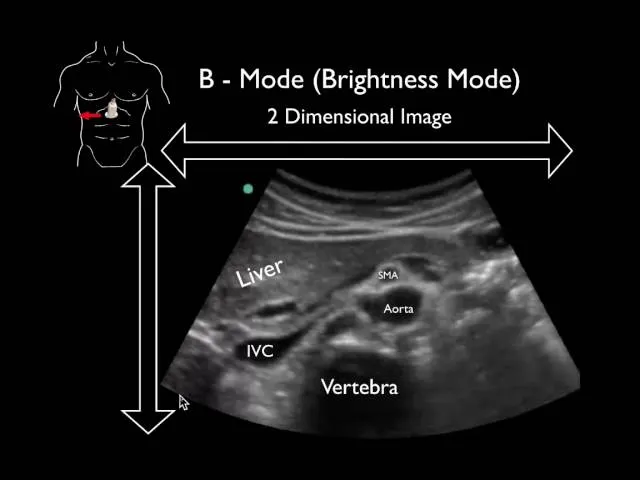
- B-Mode (Brightness): 2D grayscale. Echo strength as dot brightness. Foundation of US imaging.
- M-Mode (Motion): "Ice-pick" view. Displays motion of structures along a single scan line over time. Echocardiography.
- Digital Scan Converter (DSC):
- Converts analog signals to digital; stores image data.
- Pixel: Smallest image unit. ↑Pixels = ↑Spatial Resolution.
- Bit Depth: No. of gray shades per pixel. ↑Bit depth = ↑Contrast Resolution.
⭐ B-mode (Brightness mode) forms the basis of most ultrasound examinations, creating 2D anatomical images that are fundamental for diagnosis across various medical specialties.
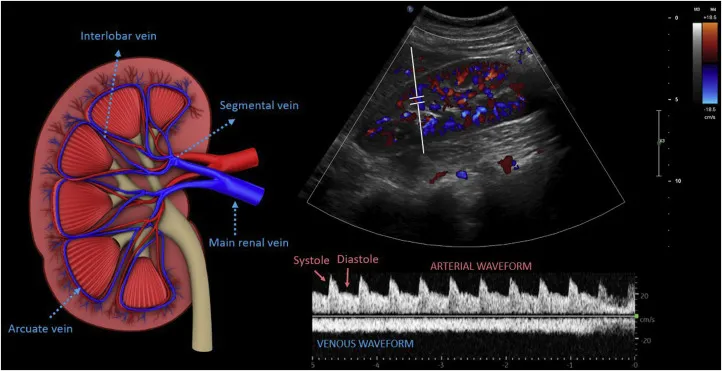
Doppler Ultrasound - Chasing the Flow
- Principle: Detects flow via Doppler shift ($f_D$) from moving RBCs. $f_D = (2 \cdot f_t \cdot v \cdot \cos\theta) / c$.
- Doppler Angle ($\theta$): Angle (beam to flow). Optimal 0°, acceptable <60°. At 90°, no shift.
- Types:
- CW Doppler: High velocity, no range gate. No aliasing.
- PW Doppler: Range gate. Aliasing if velocity > Nyquist limit (PRF/2).
- Color Doppler: Mean velocity & direction. 📌 BART: Blue Away, Red Towards.
- Power Doppler: Slow flow detection, less angle-dependent.
- Spectral Display: Velocity vs. time. Window: laminar; broadening: turbulent.
⭐ For accurate velocity, maintain Doppler angle <60°. At 90°, flow appears absent.
Artifacts & Safety - Glitches & Guidelines
- Common Artifacts:
- Reverberation: Multiple echoes (comet tail: metal; ring down: gas).
- Shadowing: ↓ signal (clean: stones; dirty: gas).
- Enhancement (PAE): ↑ signal posterior to fluid (cysts).
- Mirror Image: Duplication across strong reflector.
- Side Lobe: Spurious echoes in anechoic structures.
- Anisotropy: Tendon echogenicity varies with angle.
- Safety (ALARA Principle):
- Thermal Index (TI): Tissue heating. Keep TI < 1.0.
- Mechanical Index (MI): Cavitation risk. Keep MI < 1.9.
- Obstetric US: Prudent use; limit 1st trimester Doppler.

⭐ Posterior acoustic enhancement is a key feature distinguishing cysts from solid masses.
High-Yield Points - ⚡ Biggest Takeaways
- Piezoelectric effect is crucial for transducer operation, converting energy types.
- Higher frequency yields superior resolution but shallower penetration.
- Acoustic impedance mismatch between tissues generates echoes, forming images.
- Doppler effect enables assessment of blood flow direction and velocity.
- Key artifacts include acoustic shadowing, posterior acoustic enhancement, and reverberation.
- Transducer selection (linear, curvilinear, phased array) depends on the application and depth.
- Gain and TGC optimize image brightness and compensate for attenuation.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more