USG Basics & Artifacts - Pixel Puzzles
- Physics: Piezoelectric effect (PZT). ↑Frequency = ↑Resolution, ↓Penetration. Impedance mismatch → reflection.
- Modes: B-mode (2D), M-mode (motion), Doppler (Color/Spectral for flow).
- Echogenicity: Anechoic (fluid, black) 📌 All Fluid Black, Hypoechoic (dark), Hyperechoic (calcification/bone, white).
- Common Artifacts:
- Acoustic Shadowing: Post. to stones/bone.
- Acoustic Enhancement: Post. to cysts/fluid.
- Reverberation: Parallel lines (comet tail).
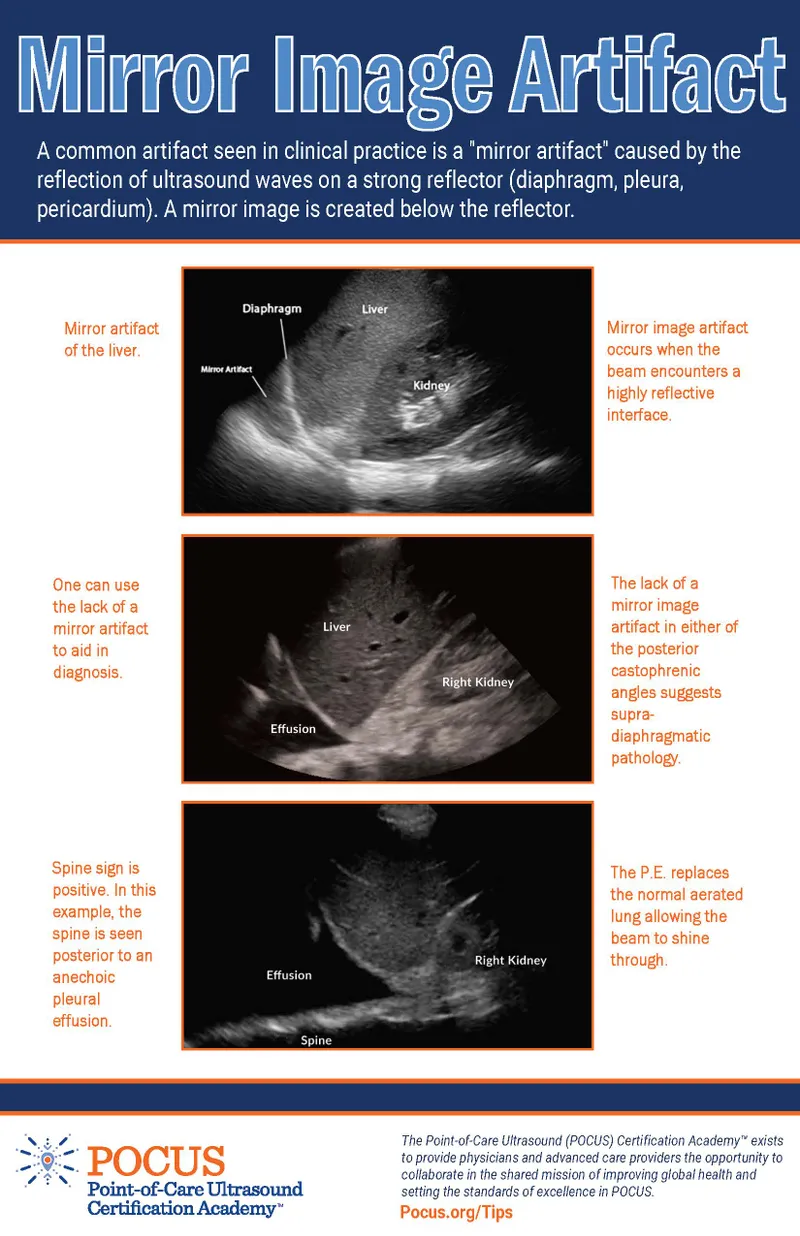
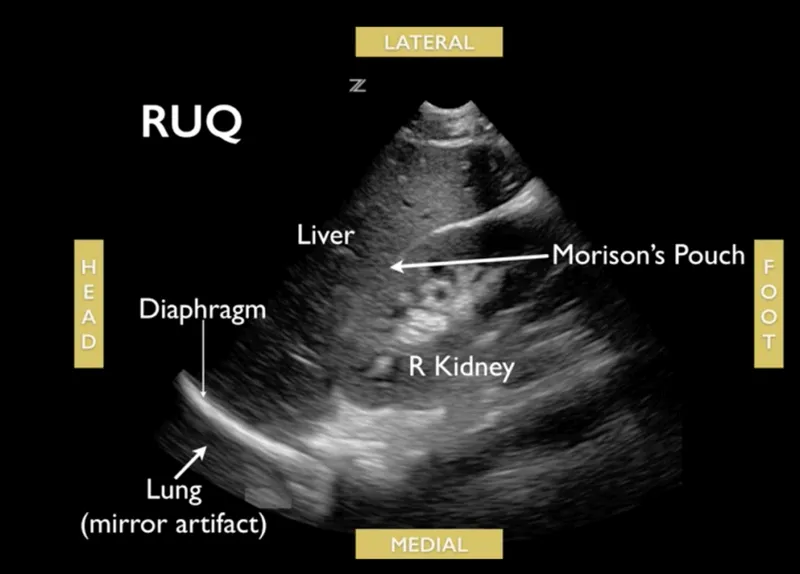
- Mirror Image: Mirror across reflector (diaphragm).
- Twinkle: Color Doppler, stones.
⭐ Posterior acoustic enhancement helps differentiate cystic vs. solid lesions.
Liver & Biliary USG - Bile Buddies 📌
- Liver Findings:
- Normal: Homogeneous, < 15.5 cm. Portal Vein < 13 mm.
- Fatty Liver (Steatosis): ↑Echogenicity (liver > R. kidney), vascular blurring.
- Cirrhosis: Coarse texture, nodular surface, caudate hypertrophy, ascites.
- Focal Lesions:
- Cyst: Anechoic, posterior acoustic enhancement.
- Hemangioma: Uniformly hyperechoic (most common benign).
- HCC: Variable echogenicity, halo, Doppler flow.
- Gallbladder & Biliary Tree Findings:
- Normal GB & CBD: GB wall < 3 mm. CBD < 7 mm (↑ 1mm/decade >60y; up to 10mm post-cholecystectomy).
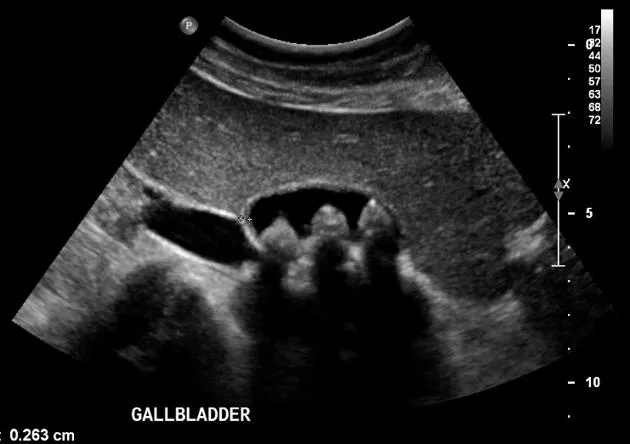
- Cholelithiasis: Mobile hyperechoic foci + posterior acoustic shadowing.
- Acute Cholecystitis: GB wall > 3 mm, pericholecystic fluid, +ve Sonographic Murphy's sign.
- Chronic Cholecystitis: Thick wall, WES sign (Wall-Echo-Shadow).
- Biliary Dilatation: Intrahepatic (parallel channel/"too many tubes"), Extrahepatic.
⭐ Sonographic Murphy's sign (focal tenderness over GB with transducer pressure) is highly specific for acute cholecystitis.
Pancreas & Spleen Scan - Belly Besties
- Pancreas:
- Normal: Homogeneous, echogenicity ≥ liver. Pancreatic duct < 3mm. Splenic vein posterior.
- Acute Pancreatitis: Enlarged, hypoechoic, peripancreatic fluid.
- Chronic Pancreatitis: Atrophic, calcifications, ductal dilatation.
- Masses: Adenocarcinoma (hypoechoic, often in head).
- Spleen:
- Normal: Homogeneous, echotexture like liver. Length < 12-13 cm.
- Splenomegaly: > 13 cm (causes: portal HTN, infections).
- Focal Lesions: Cysts (anechoic), infarcts (wedge-shaped, hypoechoic).
⭐ Accessory spleen (splenunculus): common variant near hilum/pancreatic tail; don't mistake for pathology.
Renal & Retroperitoneal USG - Kidney Chronicles
- Normal Kidney: Length 9-13 cm. Cortex typically hypoechoic or isoechoic to liver/spleen. Medullary pyramids more hypoechoic. Central sinus fat is hyperechoic.
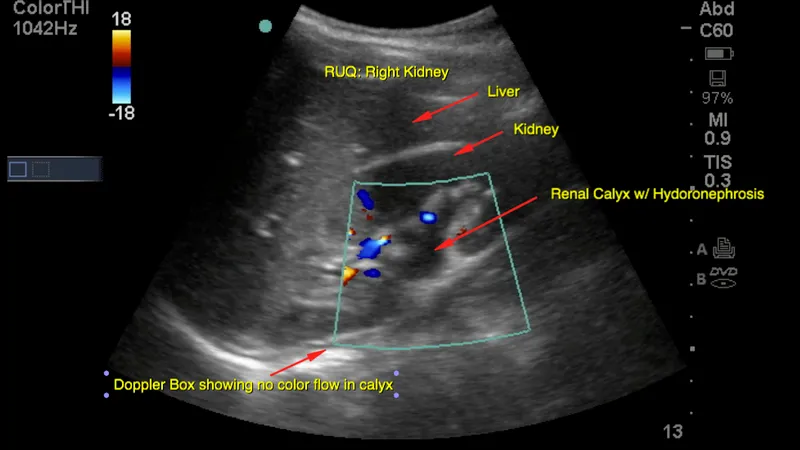
- Hydronephrosis: Dilation of pelvicalyceal system. Graded I-IV. Identify level & cause (e.g., stone, stricture, mass).
- Renal Calculi: Hyperechoic foci with posterior acoustic shadowing. 📌 Twinkling artifact on color Doppler is a key sign.
- Renal Cysts: Simple cysts: anechoic, thin smooth walls, posterior acoustic enhancement. Complex cysts: septations, wall thickening, calcifications, internal echoes.
- Renal Cell Carcinoma (RCC): Typically solid, variable echogenicity (often isoechoic/hyperechoic), may show internal vascularity on Doppler.
- Retroperitoneum: Scan for collections (hematoma, abscess), lymphadenopathy. Evaluate major vessels like aorta & IVC.
⭐ Angiomyolipomas (AMLs) are common benign renal tumors, typically markedly hyperechoic due to high fat content.
FAST & GI Tract Hints - Gut Feelings & Trauma Triage
- FAST: Rapid trauma scan for free fluid (hemoperitoneum, pericardial effusion).
- 4 Key Views: Morrison's, perisplenic, pelvic, subxiphoid.
- eFAST: Adds lung views (pneumothorax).
- GI Tract US:
- Appendicitis: Diameter >6mm, non-compressible, target sign.
- Intussusception: Target/doughnut sign. 📌 "Sausage Loves Doughnuts".
- Pyloric Stenosis: Muscle >3mm thick, canal >15mm long.
⭐ Key US criteria for hypertrophic pyloric stenosis: pyloric muscle thickness >3mm and length >15mm.
High‑Yield Points - ⚡ Biggest Takeaways
- First-line imaging for acute abdomen, especially cholecystitis, appendicitis (children/pregnant), and hydronephrosis.
- Gallstones: hyperechoic foci with posterior acoustic shadowing; cholecystitis: wall thickening >3mm, sonographic Murphy's.
- Liver: cirrhosis (coarse echotexture), fatty liver (↑echogenicity), focal lesions.
- Kidneys: hydronephrosis, stones (echogenic + shadowing), cysts.
- FAST scan detects free fluid/hemoperitoneum in trauma.
- Appendicitis: non-compressible tube >6mm, target sign.
- AAA: abdominal aorta >3cm.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

