Radiation Effects on Normal Tissues - Hit & Harm Basics
- Damage Types:
- Stochastic: Probability ↑ with dose, no threshold (e.g., carcinogenesis, genetic effects).
- Deterministic (Tissue Reactions): Severity ↑ with dose, has a threshold dose (e.g., fibrosis, necrosis, skin erythema).
- Target Theory: DNA is the primary cellular target.
- Direct Action: Radiation directly ionizes DNA or other critical macromolecules.
- Indirect Action: Radiation ionizes water → free radicals (e.g., OH•) damage DNA; predominant for X-rays & gamma rays (low-LET).
- Cellular Radiosensitivity (Law of Bergonié & Tribondeau): Cells are more radiosensitive if:
- Actively dividing (high mitotic rate)
- Undifferentiated (primitive)
- Long mitotic future
- Cell cycle phase: M > G2 > G1 > S (late S phase is most resistant).
- Tissue Radiosensitivity Hierarchy: (📌 VIM > DIM > RPM > FPM)
- VIM (Vegetative Intermitotic cells): Most sensitive (e.g., bone marrow, intestinal crypts, gonads).
- FPM (Fixed Post-mitotic cells): Most resistant (e.g., adult nerve tissue, muscle).

⭐ The Oxygen Enhancement Ratio (OER) for low-LET radiation (X-rays, gamma rays) is typically 2.5-3.5, meaning hypoxic cells are 2.5-3.5 times more resistant to radiation damage than well-oxygenated cells.
Radiation Effects on Normal Tissues - Tissue Trauma Time
-
Acute (Early) Effects:
- Onset: Days-weeks (< 90 days / < 6 months post-RT).
- Pathogenesis: Mitotic death of rapidly proliferating cells (high α/β ratio).
- Tissues: Skin, GI mucosa, bone marrow.
- Manifestations: Dermatitis, mucositis, marrow suppression.
- Usually heal; may lead to consequential late effects.
-
Chronic (Late) Effects:
- Onset: Months-years (> 90 days / > 6 months post-RT).
- Pathogenesis: Vascular/stromal damage, fibrosis; affects slowly proliferating cells (low α/β ratio).
- Tissues: Lung, kidney, CNS, heart.
- Manifestations: Fibrosis, necrosis, telangiectasia, organ failure.
- Often progressive, irreversible.
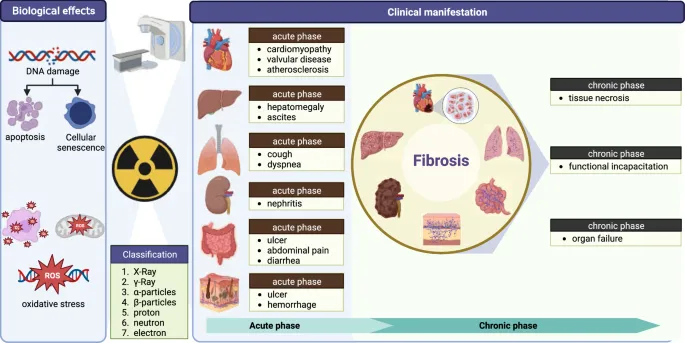
⭐ Late effects are more sensitive to fraction size (low α/β ratio tissues) than early effects (high α/β ratio tissues).
Radiation Effects on Normal Tissues - Organ System Alerts
- TD 5/5: Dose for 5% severe complication risk in 5 yrs (focal RT, specific volumes).
- Early Responders (High Sensitivity): Bone marrow, GI mucosa, skin, gonads (rapid turnover).
- Late Responders (Lower Sensitivity): Lung, kidney, CNS, liver (slow turnover).
Key Organ TD 5/5 & Effects (Typical Values):
- Bone Marrow (segmental): ~25-30 Gy (aplasia).
- GI (Small Intestine): ~45 Gy (mucositis, ulceration).
- Lungs (whole/partial): ~17 Gy (pneumonitis → fibrosis).
- Kidneys (whole/partial): ~20 Gy (nephropathy).
- CNS (Brain/Spinal Cord): ~50 Gy (necrosis/myelopathy).
- Lens: Cataracts. Threshold ~2 Gy (single), 5 Gy (fractionated).
- Gonads (Sterility): Ovary >2-3 Gy; Testes (permanent) >5-6 Gy.
- Skin (local): Erythema 2-6 Gy; Moist Desquamation >20 Gy; Necrosis >35 Gy.

Acute Radiation Syndromes (ARS) - Whole Body Irradiation:
⭐ Lhermitte's sign (electric shock on neck flexion) can indicate transient radiation myelopathy post-spinal cord RT.
High‑Yield Points - ⚡ Biggest Takeaways
- Lymphocytes are most radiosensitive; nerve/muscle cells are most radioresistant.
- Early effects (mucositis, dermatitis) are deterministic with a clear threshold dose.
- Late effects include fibrosis, necrosis, cataracts (threshold), and secondary malignancies (stochastic).
- Highly radiosensitive tissues: Bone marrow, gonads, lymphoid tissue, intestinal epithelium.
- Highly radioresistant tissues: Mature bone, muscle, brain, spinal cord.
- TD 5/5: Tolerance dose for 5% severe complication risk in 5 years.
- Fractionation spares normal tissues by allowing repair of sublethal damage between doses.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

